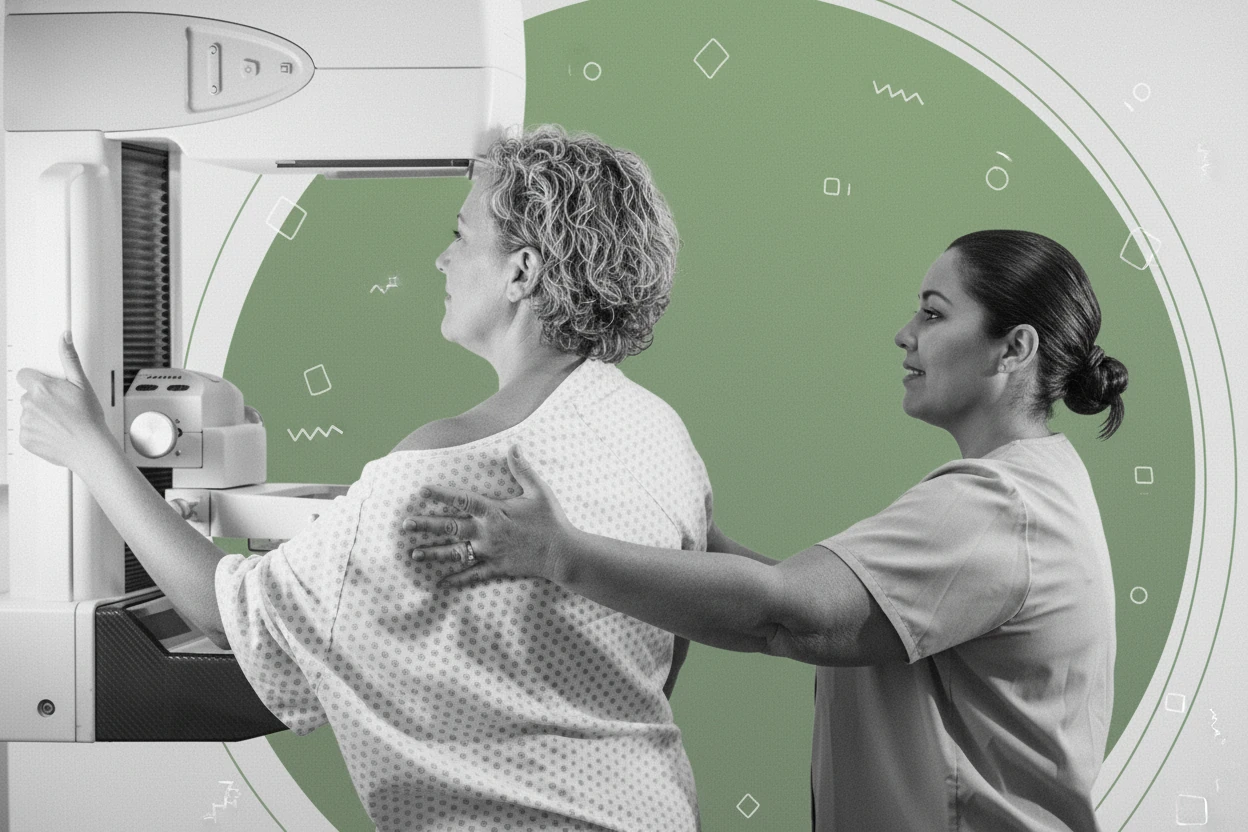
Nearly half of women over 40 have dense breast tissue, a common finding on mammograms that can affect breast cancer screening and risk assessment1 2. Dense breasts contain more fibroglandular tissue than fatty tissue, making it harder to detect cancer on mammograms and slightly increasing breast cancer risk3 4. Understanding what dense breasts mean and how to manage this diagnosis is essential for personalized breast health care5 6.
Understanding Dense Breast Tissue
Dense breast tissue refers to the proportion of fibrous and glandular (fibroglandular) tissue compared to fatty tissue in the breast, as seen on a mammogram7 3. The breast is composed of lobules (milk-producing glands), ducts (milk-carrying tubes), connective tissue, and fat. Dense breasts have more glandular and connective tissue and less fat, which appears white on mammograms, while fatty tissue appears dark7 4.
Breast density is classified into four categories by the American College of Radiology's Breast Imaging Reporting and Data System (BI-RADS):
- Category A: Almost entirely fatty – breasts mostly composed of fat5 7.
- Category B: Scattered areas of fibroglandular density – mostly fatty with some dense tissue5 7.
- Category C: Heterogeneously dense – mostly dense tissue with some fatty areas5 3.
- Category D: Extremely dense – almost entirely dense tissue with very little fat5 3.
Women with categories C or D are considered to have dense breasts, which applies to about 40–50% of women over 40 in the United States2 8. Breast density tends to decrease with age but can remain high in some women1 9.
Dense breast tissue is normal and not abnormal, but it has two important implications:
- Masking effect: Dense tissue appears white on mammograms, the same color as many breast cancers, making it harder to detect tumors4 10.
- Increased cancer risk: Women with the highest breast density have nearly a fivefold increased risk of breast cancer compared to those with the lowest density4 2.
“These cancers can be growing and getting larger and more advanced until they finally peek out of the corner of that density and you can see them on a mammogram.”
— Robert Smith, American Cancer Society19
Breast density is influenced by genetics, body mass index (BMI), age, and hormone therapy. Women with a family history of dense breasts are more likely to have dense tissue themselves9 . Hormone therapy for menopause can increase breast density7 .
Dense breast tissue reduces the sensitivity of mammography, meaning cancers can be missed or detected later10 11. This "masking" effect leads to a higher rate of interval cancers—cancers diagnosed between regular screenings—in women with dense breasts12 . Mortality reduction from mammography is also lower in women with dense breasts due to this challenge11 .
Despite these challenges, mammography remains an effective screening tool and is recommended annually or biennially for women over 40, including those with dense breasts13 5. Newer technologies such as digital mammography and 3D mammography (tomosynthesis) improve visualization and cancer detection in dense breasts5 .
“Genetics, body mass index, and age are some of the main drivers. So, if your mother or other close relative has dense breast tissue, you might, too.”
— Ethan Cohen, M.D., MD Anderson Cancer Center9
Managing Your Dense Breast Diagnosis
If your mammogram report indicates dense breasts, it is important to discuss what this means for your breast cancer risk and screening options with your healthcare provider6 5. Many states require that women be notified about their breast density after mammography, with 38 states and the District of Columbia having laws mandating such notifications6 .
Breast density is one factor among many that influence breast cancer risk. Your healthcare provider will consider your overall risk based on:
- Family history of breast cancer
- Genetic mutations (e.g., BRCA1/2)
- Personal medical history
- Age and hormonal factors
- Breast density category6 2
Women at average risk with dense breasts usually continue with routine mammography screening13 5. For women at higher risk, supplemental screening may be recommended14 15.
Additional imaging tests can help detect cancers that mammography might miss in dense breasts. These include:
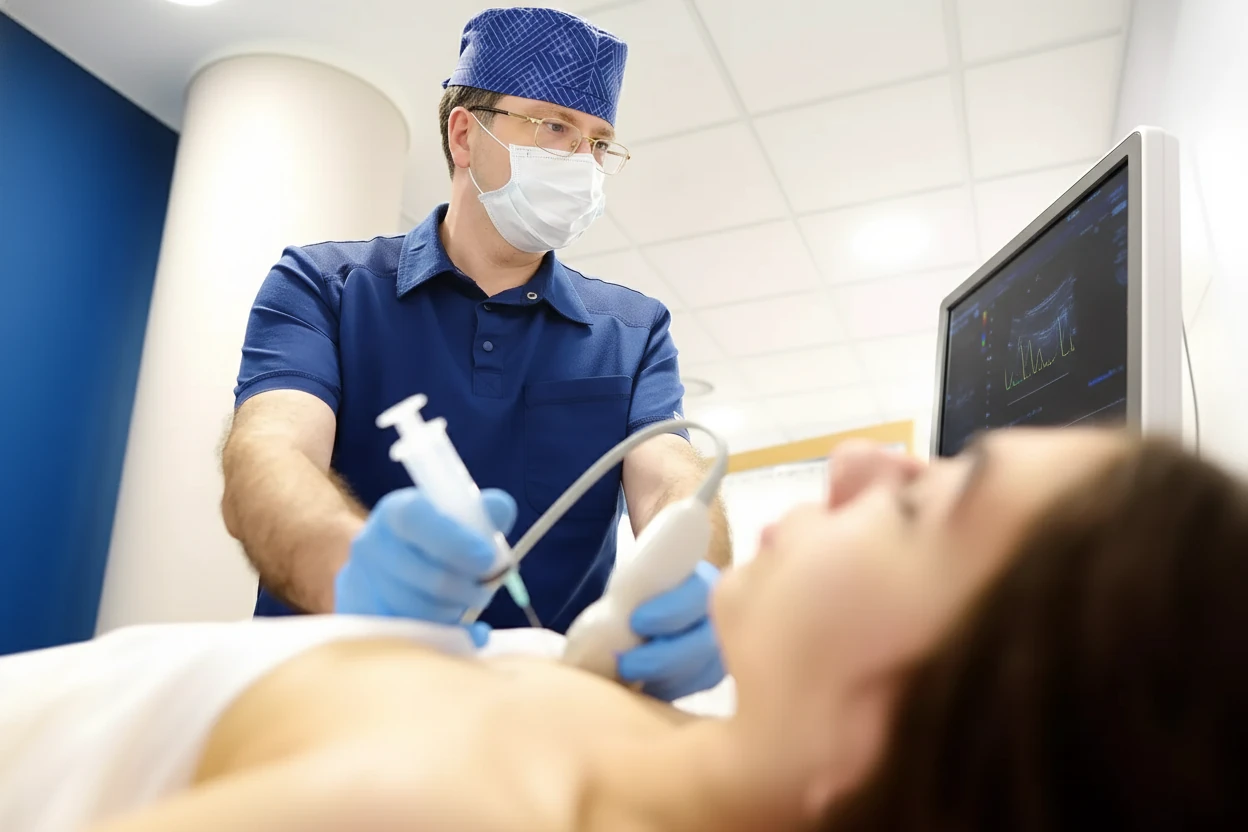
- Breast ultrasound: Uses sound waves to image breast tissue and can detect abnormalities not visible on mammograms. It is widely available but less sensitive than MRI and may result in false positives10 16.
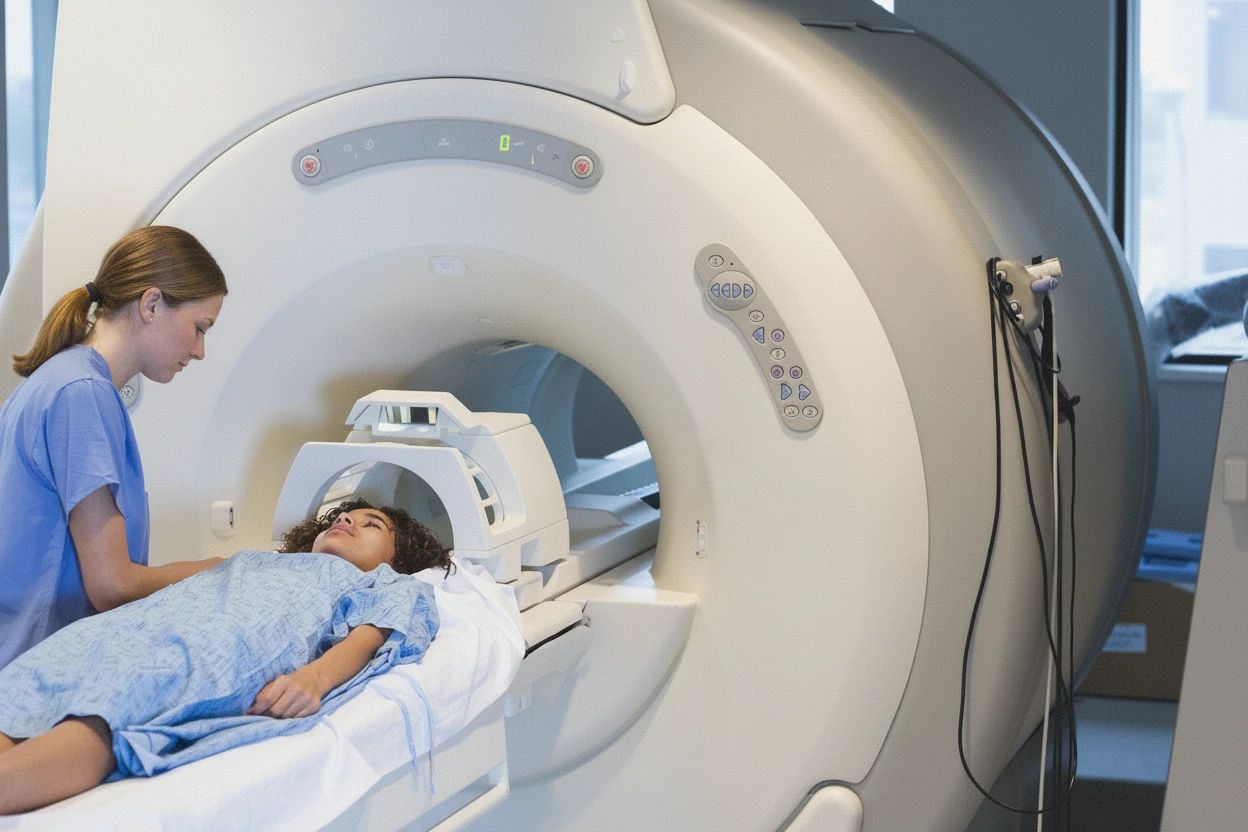
- Breast MRI: Uses magnetic fields and radio waves to produce detailed images. MRI is the most sensitive supplemental screening but is costly and less accessible. It is recommended for women at high risk and has shown to reduce interval cancer rates by over 80% in women with extremely dense breasts12 14.
- Contrast-enhanced mammography (CEM): Uses iodine-based contrast to highlight suspicious areas on mammograms17 .
- Molecular breast imaging: Uses radioactive tracers and specialized cameras to detect cancerous tissue10 .
The choice of supplemental screening depends on individual risk, preferences, availability, and insurance coverage6 18. Currently, there is no consensus on routine supplemental screening for all women with dense breasts, emphasizing shared decision-making13 19.
| Screening Modality | Sensitivity Range | Specificity Range | Notes |
|---|---|---|---|
| MRI | 71–100% 12 | 81–98% 12 | Most sensitive, costly, less accessible |
| Ultrasound | Moderate10 | Variable | Widely available, risk of false positives |
| Contrast-enhanced Mammography | Not specified | Not specified | Emerging option, uses contrast agent |
| Molecular Breast Imaging | Not specified | Not specified | Uses radioactive tracer |
“You cannot counsel an entire population of women with dense breasts with one policy that’s going to be appropriate for everybody.”
— Dr. Mark Pearlman, University of Michigan Medical School19
Twenty-one states and DC have insurance laws covering supplemental breast imaging, with Oklahoma requiring coverage for diagnostic breast imaging6 . Coverage varies widely, so patients should verify their insurance benefits.
Women with dense breasts and additional risk factors (e.g., genetic mutations, strong family history) may benefit from more intensive screening, such as alternating mammograms and MRI every six months14 9. This approach aims to detect cancer as early as possible.
- Continue regular mammogram screening as recommended13 .
- Discuss your breast density and overall risk with your healthcare provider6 .
- Consider supplemental screening if you have additional risk factors or if recommended by your provider10 .
- Be aware of the benefits and potential harms of additional tests, including false positives and increased anxiety19 .
- Stay informed about your insurance coverage and local laws regarding breast density notification and supplemental screening6 .