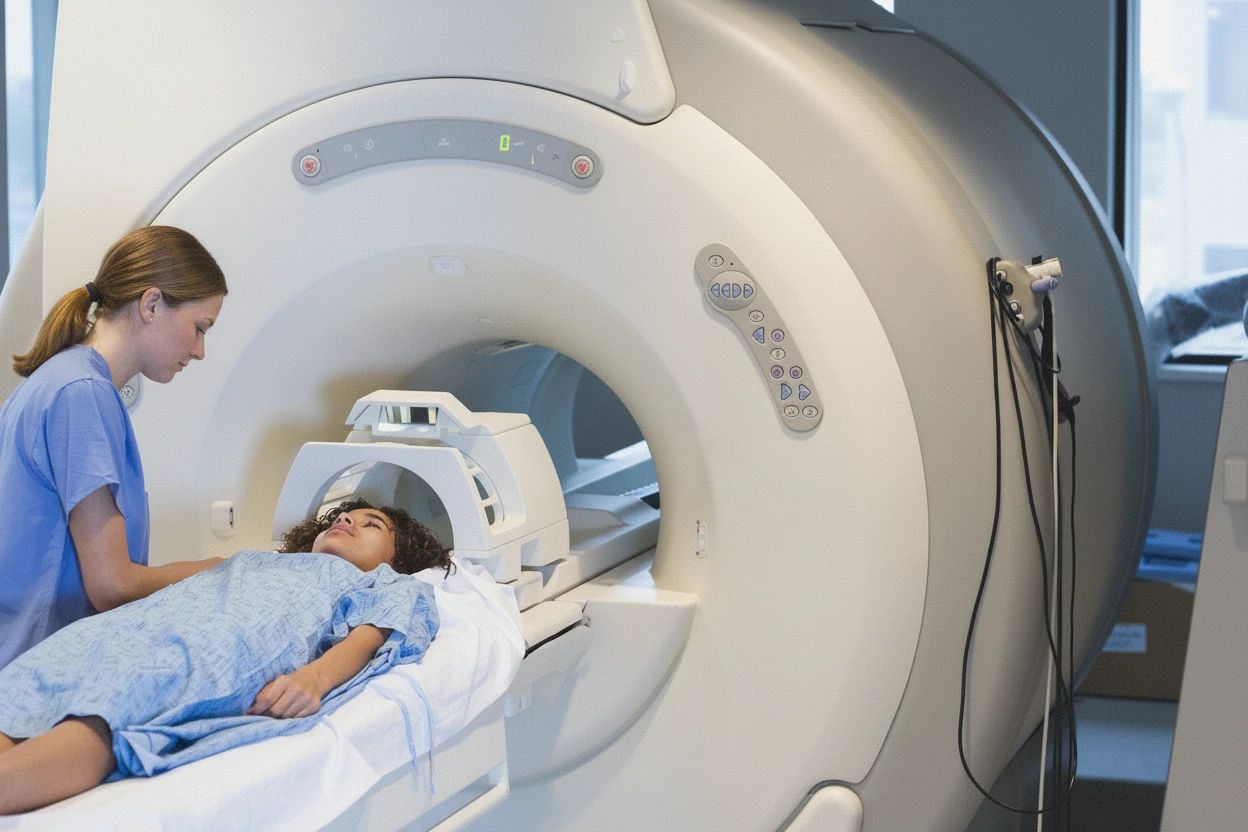
Whole-body magnetic resonance imaging (MRI) scans have gained popularity as a comprehensive health screening tool, offering a panoramic view of the body in a single session1 . While this technology promises early detection of hidden diseases, including cancers and aneurysms, its benefits for the general population remain uncertain2 . Moreover, full-body MRIs may uncover incidental findings that lead to unnecessary anxiety and additional testing, raising questions about their overall value in preventive health3 .
Full-Body MRI Explained
A full-body MRI, also known as whole-body MRI (WB-MRI), is an imaging technique that uses magnetic fields and radio waves to create detailed pictures of the entire body without exposing patients to ionizing radiation4 . Typically completed within an hour, WB-MRI provides anatomical and functional information across multiple organ systems, making it a radiation-free alternative to other imaging modalities like CT scans4 2.
Advancements such as diffusion-weighted imaging (DWI) have improved the ability of WB-MRI to detect and characterize lesions, enhancing its diagnostic potential4 5. This modality is particularly valuable for cancer screening and staging in patients with genetic cancer predisposition syndromes, such as Li-Fraumeni syndrome, where early detection can significantly improve outcomes6 7. WB-MRI is also increasingly used in pediatric oncology and rheumatology due to its safety profile and ability to assess systemic disease without radiation exposure8 9.
Despite these advantages, WB-MRI protocols vary widely across institutions, and its role in screening asymptomatic individuals remains controversial due to inconsistent findings and unclear cost-effectiveness10 11. The technique is not standardized, and image quality can differ depending on the scanner and protocol used12 .
- WB-MRI uses magnetic fields and radio waves, avoiding radiation exposure4 2.
- Typically completed in about one hour, providing a comprehensive body overview4 .
- Enhanced by diffusion-weighted imaging (DWI) for better lesion detection4 5.
- Valuable for patients with genetic cancer risks like Li-Fraumeni syndrome6 7.
- Expanding use in pediatric oncology and rheumatology for safe systemic imaging8 9.
💡 Did You Know?
A full-body MRI scan is like a 40,000-foot flyover: it offers a broad view but cannot detect every detail, especially small tumors13 .
Targeted vs. Full-Body MRI Scans
Targeted MRI scans focus on specific organs or regions of the body, offering superior spatial resolution and shorter scan times compared to full-body MRI14 . This makes them the preferred choice for evaluating localized symptoms or known disease sites. For example, dedicated breast MRI uses contrast agents and patient positioning optimized for breast tissue, which full-body MRI typically lacks, limiting the latter’s ability to detect certain cancers effectively3 .
In contrast, full-body MRI provides a broad overview of the entire body in one session, which can occasionally detect unexpected pathologies outside the symptomatic area15 . This wide-ranging approach is particularly useful for patients with cancer predisposition syndromes who may develop tumors in multiple locations6 13. However, the lower resolution of WB-MRI for specific organs means it cannot replace organ-specific imaging or routine cancer screenings recommended for the general population14 16.
- Targeted MRI offers higher resolution and faster scans for specific body parts14 .
- Full-body MRI scans the entire body but with lower organ-specific detail14 16.
- Targeted scans are essential for symptom-driven diagnostics and routine cancer screening3 .
- Full-body MRI can detect unexpected abnormalities beyond the symptomatic region15 .
- Best suited for patients with genetic risks for multiple cancers, such as Li-Fraumeni syndrome6 13.
| Feature | Targeted MRI | Full-Body MRI |
|---|---|---|
| Scan focus | Specific organ or body region | Entire body |
| Spatial resolution | High | Lower for individual organs |
| Scan duration | Shorter | Typically around one hour |
| Use case | Symptom evaluation, routine screening | Screening in high-risk patients |
| Detection of incidental findings | Less common | More frequent |
| Sources: 3613141516 | ||
Full-body MRIs can detect many abnormalities, but most are harmless and lead to extra testing that may not benefit patients. For most healthy individuals, the risks and costs outweigh the potential benefits1 3.
Potential Risks of Full-Body MRI
While full-body MRI scans offer a radiation-free and comprehensive imaging option, they carry several risks and limitations, especially when used for screening asymptomatic individuals.
One of the most significant challenges with WB-MRI is the high prevalence of incidental findings—abnormalities detected that are unrelated to any symptoms and often benign17 15. Studies report that up to 95% of individuals undergoing WB-MRI have at least one abnormal finding, but the vast majority of these do not indicate serious disease3 . These incidentalomas can lead to a cascade of further diagnostic procedures, including invasive biopsies and surgeries, which may not improve patient outcomes but increase healthcare costs and patient anxiety17 1518.
Discovering incidental findings can cause considerable psychological distress. Patients who undergo WB-MRI may start viewing themselves as ill despite feeling healthy, leading to anxiety and a negative shift in their perception of quality of life19 1. The uncertainty associated with indeterminate findings often results in prolonged stress while awaiting further testing or monitoring15 1.
“People may hope the scan will find nothing and that will be reassuring, which I understand. Unfortunately, most whole-body MRIs generate incidental findings. Though most of these are not relevant, they may require additional workup and can heighten and prolong anxiety.”
— Brian N. Dontchos, MD3
Full-body MRI is not foolproof. It may miss small or aggressive tumors, leading to false-negative results that give patients a misleading sense of security3 1. Additionally, the lack of intravenous contrast in many WB-MRI protocols limits the detection of certain cancers, such as breast cancer, where contrast-enhanced imaging is critical3 . The sensitivity of WB-MRI is comparable to CT for some tumors, but neither modality guarantees detection of all lesions15 .
WB-MRI is an expensive diagnostic tool, often costing thousands of dollars per scan and typically not covered by insurance for healthy individuals without specific indications18 3. The high out-of-pocket cost limits accessibility and may contribute to healthcare disparities if used widely without proven benefit12 .
- High rate of incidental findings leading to unnecessary follow-up tests and procedures17 15.
- Increased patient anxiety and psychological distress from uncertain or benign findings19 1.
- Potential for false negatives, missing small or aggressive tumors3 1.
- Limited sensitivity for certain cancers due to lack of contrast and lower resolution3 .
- High cost and limited insurance coverage for screening in asymptomatic individuals18 12.