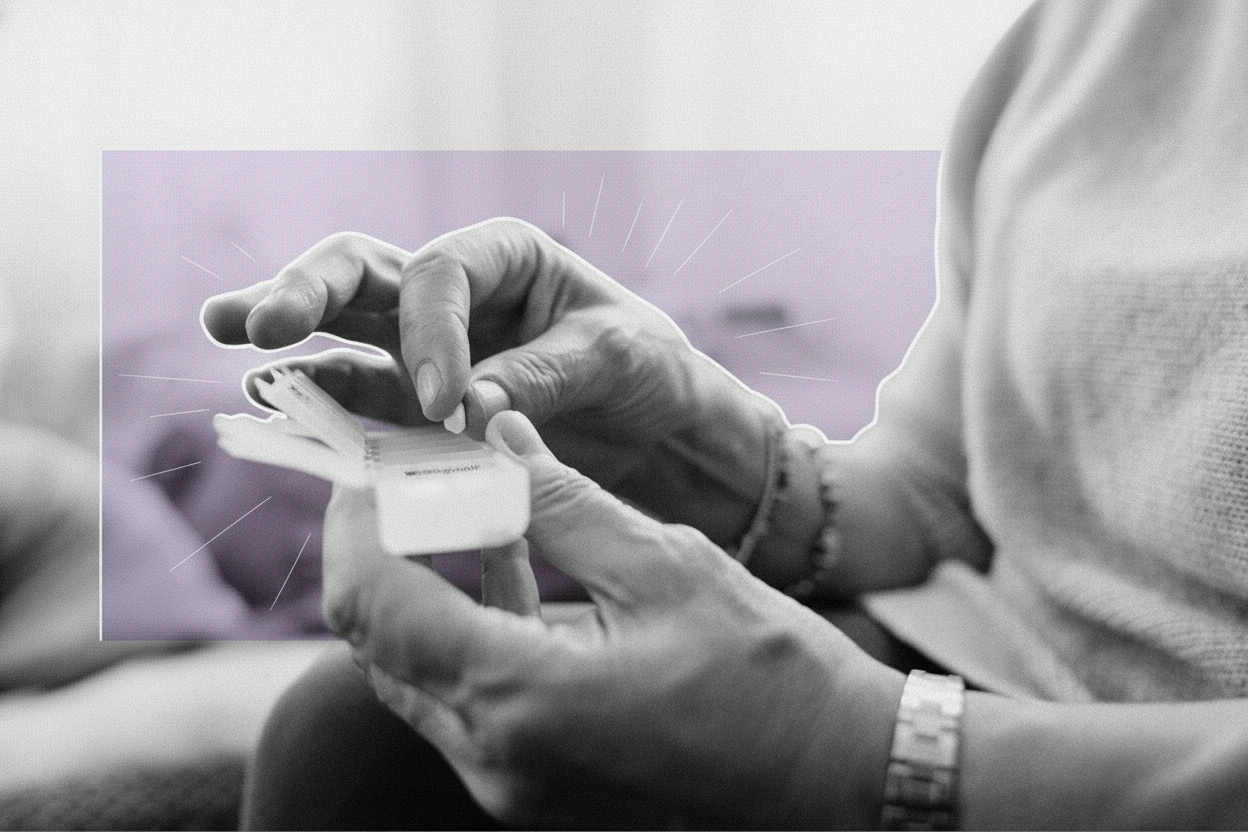
One in four older adults take aspirin at least three times a week, mainly to prevent heart attacks and strokes1 . However, more than half of these individuals aged 50 to 80 do not have a history of cardiovascular disease, raising concerns about the appropriateness of aspirin use in this group1 . As aspirin use carries risks such as bleeding, especially in older adults, understanding current trends and recommendations is crucial for safe and effective care2 .
Because aspirin increases bleeding risk, especially in older adults, it is crucial to weigh individual health factors before starting or continuing therapy. Regular consultation with healthcare providers ensures safer medication use. 24
Daily Aspirin Use Trends
Daily aspirin use for primary prevention of cardiovascular disease (CVD) has declined in recent years, yet a significant number of older adults continue to take it, often without medical advice . Approximately 57% of people aged 50 to 80 who regularly use aspirin have no history of cardiovascular disease, indicating widespread use beyond established indications1 . Furthermore, 42% of adults aged 75 to 80 are taking aspirin, despite guidelines advising caution in this age group1 .
The persistence of aspirin use among older adults may be partly due to long-standing recommendations that have since evolved. Notably, 71% of older adults who take aspirin started four or more years ago, suggesting they may be following outdated advice1 . Additionally, 31% of older adults taking aspirin are unaware of the increased bleeding risks associated with its use1 .
💡 Did You Know? The elderly face risks when taking drugs regularly including drug ineffectiveness, adverse drug effects, underdosage, overdosage, inadequate monitoring of usage, nonadherence, and drug interactions3 .
Older adults face unique challenges with medication use, including drug ineffectiveness, adverse effects, underdosage, overdosage, inadequate monitoring, nonadherence, and drug interactions3 . These factors complicate the risk-benefit balance of aspirin therapy in this population.
Key points about aspirin use trends in older adults:
- One in four older adults take aspirin regularly, mostly for heart attack and stroke prevention1 .
- Over half of these users have no cardiovascular disease history, indicating primary prevention use1 .
- Aspirin use remains common in adults over 75, despite bleeding risks increasing with age1 .
- Many older adults started aspirin years ago and may be unaware of updated guidelines1 .
- Medication risks in the elderly include side effects and interactions that may amplify aspirin’s harms3 .
Aspirin use in older adults is often based on outdated guidelines, leading many to take it without fully understanding the bleeding risks. Regular review of medication regimens is essential to ensure safety and appropriateness. 13
Daily Aspirin Recommendations
Current guidelines emphasize individualized assessment of the risks and benefits of daily aspirin therapy, especially for adults aged 60 and older . The primary concern is the increased risk of bleeding, including gastrointestinal bleeding and hemorrhagic stroke, which often outweighs the cardiovascular benefits in those without pre-existing heart disease2 .
Daily aspirin therapy may be used for two main purposes:
- Primary prevention: For individuals who have never had a heart attack or stroke.
- Secondary prevention: For those with a history of heart attack, stroke, or known cardiovascular disease.
“Aspirin is no longer a one-size-fits-all preventive tool for older adults, which for decades it was touted as.”
— Jordan Schaefer, M.D., M.Sc., Michigan Medicine1
For primary prevention, recent recommendations generally advise against starting aspirin in adults aged 60 or older without known cardiovascular disease due to bleeding risks2 14. Some guidelines suggest stopping aspirin after age 70 in those without cardiovascular disease2 . In contrast, aspirin remains a common and recommended therapy for secondary prevention, where the benefits of preventing recurrent cardiovascular events outweigh bleeding risks1 .
The risk of bleeding increases with age and can be exacerbated by factors such as alcohol consumption, use of other medications (e.g., NSAIDs), and underlying health conditions2 5. Aspirin’s blood-thinning effect reduces clot formation but also raises the chance of bleeding complications.
Older adults often take multiple medications for chronic conditions, increasing the likelihood of adverse drug effects and interactions5 . Nonsteroidal anti-inflammatory drugs (NSAIDs), for example, can increase the risk of stomach ulcers and bleeding, which may compound aspirin’s effects5 . Careful medication review is essential to minimize harm.
“If you're taking a daily low-dose aspirin 81 milligrams (mg) — but you're at low risk for heart disease, stroke, or bleeding risks (say, from a peptic ulcer), talk to your doctor as soon as possible about whether you should continue taking it.”
— Heidi Godman, Harvard Health Letter4
Risks and considerations for daily aspirin use in older adults:
- Bleeding risks increase with age and can include gastrointestinal bleeding and hemorrhagic stroke2 6.
- Aspirin is generally not recommended for primary prevention in adults 60 years or older without cardiovascular disease1 4.
- Secondary prevention remains a key indication for aspirin use in those with prior heart attack or stroke .
- Concurrent medications and alcohol use can increase bleeding risks2 5.
- Older adults are more sensitive to medications and prone to adverse effects and drug interactions3 5.
| Indication | Recommendation for Older Adults (≥60 years) | Risk Considerations |
|---|---|---|
| Primary prevention | Generally not recommended to start aspirin | Increased bleeding risk outweighs benefit2 14 |
| Secondary prevention | Recommended for those with history of heart attack or stroke | Benefits usually outweigh bleeding risks1 |