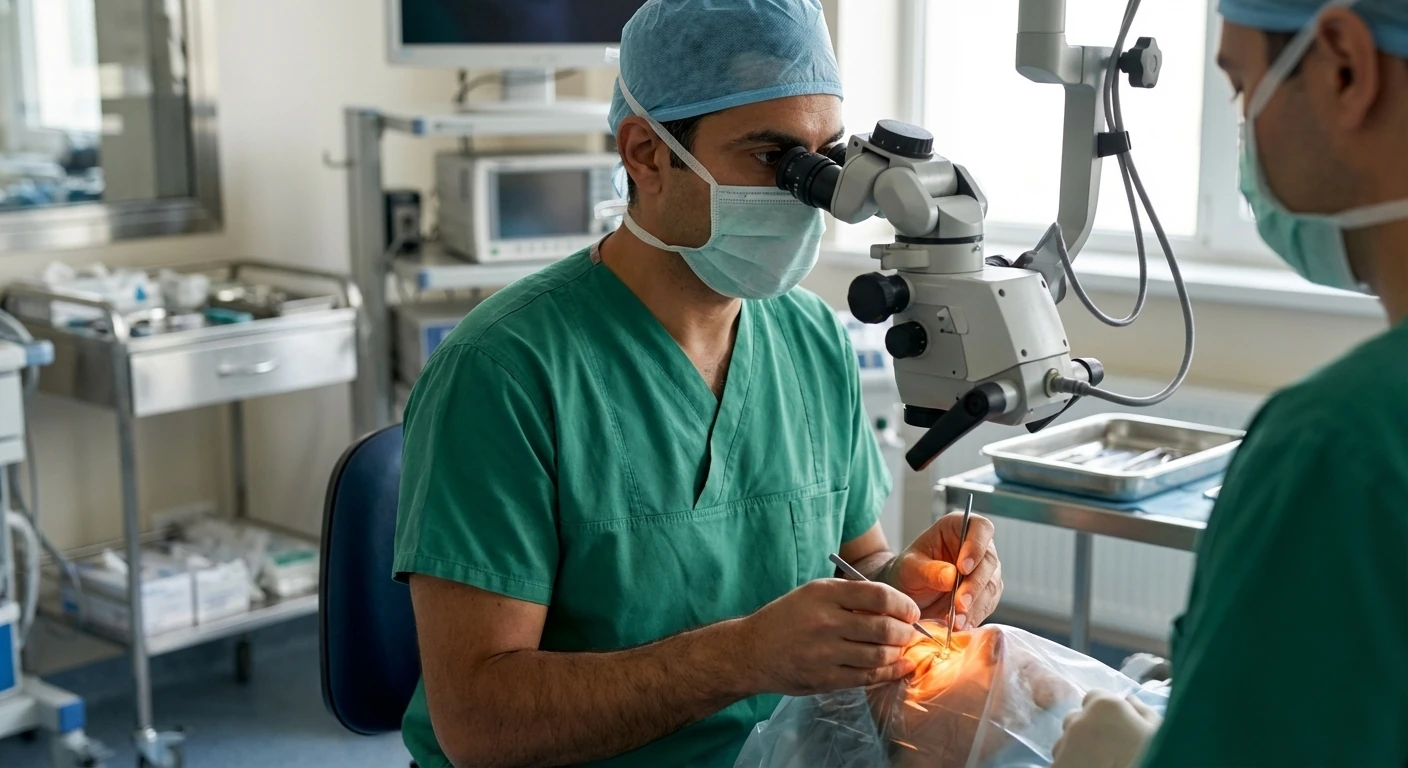
Glaucoma affects over 70 million people worldwide and is a leading cause of irreversible vision loss and blindness1 . This group of eye diseases damages the optic nerve, often due to increased pressure inside the eye, called intraocular pressure (IOP) 1. While medications and laser treatments are the first steps to control glaucoma, surgery may be necessary when these methods fail to prevent further vision loss2 . Glaucoma surgery cannot restore lost vision but can help protect remaining sight by lowering eye pressure3 .
When Is Glaucoma Surgery Necessary?
Medical therapy is typically the first-line treatment for glaucoma, focusing on lowering intraocular pressure with eye drops or oral medications4 . However, surgery is considered when medication fails to adequately control IOP or if the patient cannot tolerate the medications due to side effects or allergies4 5. Poor adherence to medication regimens is another common reason for surgical intervention4 .
In cases of advanced glaucoma or acute angle-closure glaucoma—a sudden and severe rise in eye pressure caused by blockage of the drainage angle—surgery is often urgently required to prevent permanent vision loss6 7. Acute angle-closure glaucoma is a medical emergency demanding prompt treatment to protect vision6 .
Surgical options may also be recommended for patients who have difficulty using topical medications consistently or have multiple medication allergies5 . Some patients may undergo surgery without prior medication use if deemed appropriate by their ophthalmologist5 .
Types of Glaucoma Surgery Procedures
Glaucoma surgeries aim to lower intraocular pressure by improving fluid drainage or reducing fluid production in the eye. The main types include Micro Invasive Glaucoma Surgery (MIGS), laser treatments, trabeculectomy, and implant surgery4 7.
Micro Invasive Glaucoma Surgery (MIGS)
MIGS procedures are designed to be less invasive alternatives to traditional glaucoma surgeries, involving small incisions and microscopic devices to enhance aqueous humor drainage4 8. These surgeries are primarily indicated for patients with mild to moderate glaucoma8 . MIGS typically have fewer complications, shorter surgical times often under 10 minutes, and faster recovery compared to conventional surgeries9 8.
MIGS techniques include:
- Microtrabeculectomy: Insertion of tiny stents to facilitate fluid drainage through natural pathways4 .
- Trabecular bypass: Creating a small incision in the trabecular meshwork and placing a device to improve outflow; devices may remove part of the meshwork or leave a stent in place4 .
- Suprachoroidal shunts: Devices that connect the anterior chamber to the suprachoroidal space to enhance drainage4 .
- Laser photocoagulation: Targeting the ciliary body to reduce aqueous humor production4 .
MIGS can be combined with cataract surgery to improve outcomes10 . These procedures are less disruptive to eye anatomy and often do not require stitches11 .
Laser Treatments
Laser glaucoma procedures use focused light beams to improve fluid drainage or reduce fluid production in the eye3 . They are often performed in an office setting with minimal recovery time6 . Laser trabeculoplasty, for example, targets the trabecular meshwork to increase aqueous outflow3 .
Laser treatments are typically recommended before incisional surgeries unless the eye pressure is very high or optic nerve damage is severe3 . They are suitable for early-stage glaucoma and can help delay or reduce the need for more invasive surgery4 .
Common laser procedures include:
- Laser trabeculoplasty: Enhances drainage through the trabecular meshwork.
- Laser photocoagulation: Reduces fluid production by treating the ciliary body4 .
Trabeculectomy
Trabeculectomy is considered the gold standard for glaucoma surgery, especially for open-angle glaucoma2 3. It involves creating a tiny opening in the sclera (the white part of the eye) under the eyelid to allow aqueous humor to drain out, lowering intraocular pressure2 . The surgery is usually done with local anesthesia and sedation, and patients often go home the same day with someone to drive them2 .
Special medications may be used during surgery to prevent scarring and closure of the new drainage opening, which is critical for long-term success3 . Postoperative adjustments, such as removing releasable sutures or using laser to melt stitches, can help maintain the function of the drainage site11 .
Trabeculectomy is generally more effective at lowering eye pressure than MIGS but carries higher risks and longer recovery times7 3.
Implant Surgery
Glaucoma implant surgery involves placing a tiny tube or shunt on the white part of the eye to help drain excess fluid and reduce eye pressure2 . This surgery is used for various types of glaucoma, including congenital, neovascular, and trauma-related glaucoma2 .
The implant directs aqueous humor out of the eye through an alternative drainage pathway, bypassing the natural drainage system3 . Implant surgery is typically reserved for cases where other treatments have failed or are unsuitable7 .
Potential Risks and Complications
All glaucoma surgeries carry some risk, with the severity and type of complications varying by procedure7 . MIGS procedures are generally safer and less invasive, with fewer complications than traditional surgeries8 . However, even MIGS can cause transient increases in intraocular pressure and temporary changes in vision4 .
Glaucoma surgery reduces eye pressure and helps prevent future vision loss. MIGS offers a less invasive option with faster recovery, while trabeculectomy and implants provide more effective pressure control but with higher risks and longer healing times11 7.
Common risks and side effects include:
- Swelling, soreness, and irritation, especially after laser procedures6 .
- Dry eye and corneal abrasions, which are usually self-limiting6 .
- Blurred vision and foreign body sensation during recovery6 11.
- Infection risk, particularly with trabeculectomy and implant surgeries7 .
- Cataract formation and corneal problems following invasive surgeries7 12.
- Rare complications such as bleeding inside the eye or fluid pockets behind the retina due to very low eye pressure12 .
Damage to corneal endothelial cells can occur with any surgery involving the anterior chamber, potentially reducing cell density and affecting corneal health13 .
Some forms of glaucoma surgery, including trabeculectomy, can be modified in the postoperative period to encourage long-term function. For instance, your eye doctor might remove releasable sutures from the eye or melt stitches placed underneath the outer covering of the eye using a laser. This works best only during the first few weeks after surgery, and so attending all your postoperative appointments is critical11 .
Glaucoma Surgery Recovery Process
Recovery time after glaucoma surgery varies depending on the type of procedure performed. MIGS procedures typically allow patients to see well the day after surgery with minimal discomfort due to their less invasive nature11 . In contrast, recovery from trabeculectomy and implant surgeries can take longer and require more careful monitoring11 .
Laser trabeculoplasty generally has a quick recovery, often allowing patients to resume normal activities the day after treatment without needing a ride home6 . More invasive surgeries may require activity restrictions for up to four weeks to protect the healing eye6 .
💡 Did You Know?
Glaucoma is caused by damage to the optic nerve at the back of the eye, often linked to increased eye pressure. Surgery is recommended when medicines and laser treatments do not adequately control the disease2 .
Postoperative care usually includes prescription eye drops for several weeks to prevent infection and reduce inflammation6 . Patients have multiple follow-up appointments to monitor healing and eye pressure, and to manage any complications11 .
Important recovery tips include:
- Avoid heavy lifting, bending over, vigorous activity, or straining, especially if eye pressure is low11 .
- Do not drive for at least one day after surgery due to sedation effects11 .
- Avoid swimming, hot tubs, reusable contact lenses, eye makeup, and face creams during early recovery to reduce infection risk11 .
Visual recovery depends on the surgery and on the eye's healing response. Some patients see as well the day after surgery as they did before, and experience no discomfort. This is more common with MIGS procedures, since they have minimal effect on the shape of the eye and use only tiny incisions and often no stitches. Recovering from other glaucoma surgeries, including trabeculectomy and tube shunt surgery, can take longer11 .
Glaucoma Surgery Summary
Glaucoma surgery is an important option to lower intraocular pressure and prevent further vision loss when medications and laser treatments are insufficient7 . The choice of surgery depends on the type and severity of glaucoma, as well as the overall health of the eye3 .
| Surgery Type | Indication | Advantages | Recovery Time | Risks |
|---|---|---|---|---|
| MIGS | Mild to moderate glaucoma | Less invasive, fewer complications, quick recovery8 11 | Days to weeks11 | Transient IOP rise, vision changes4 |
| Laser Treatments | Early-stage glaucoma | Office procedure, minimal recovery6 3 | Hours to days6 | Swelling, soreness, dry eye6 |
| Trabeculectomy | Advanced open-angle glaucoma | Effective IOP lowering2 3 | Weeks to months11 | Infection, cataracts, scarring7 12 |
| Implant Surgery | Complex or refractory glaucoma | Alternative drainage pathway2 3 | Weeks to months11 | Infection, corneal damage7 12 |
| Sources: 12345678910111213 | ||||
Glaucoma surgery does not reverse vision loss but helps protect remaining vision by controlling eye pressure2 3. Success rates vary, with trabeculectomy lowering eye pressure in about 70% of patients, especially those without prior eye injury or surgery2 . Some patients may require repeat surgery if the drainage opening closes over time2 .
Because of the sedation used during glaucoma surgery, you will not be able to drive for a day following your procedure, so you will need to find someone to accompany you home. After the patch is removed the day after surgery, some patients may be able to resume driving. This is based on level of vision in both eyes and your comfort level in safely operating a vehicle during the recovery period11 .
— Thomas V. Johnson, III, Wilmer Eye Institute, Johns Hopkins Medicine11