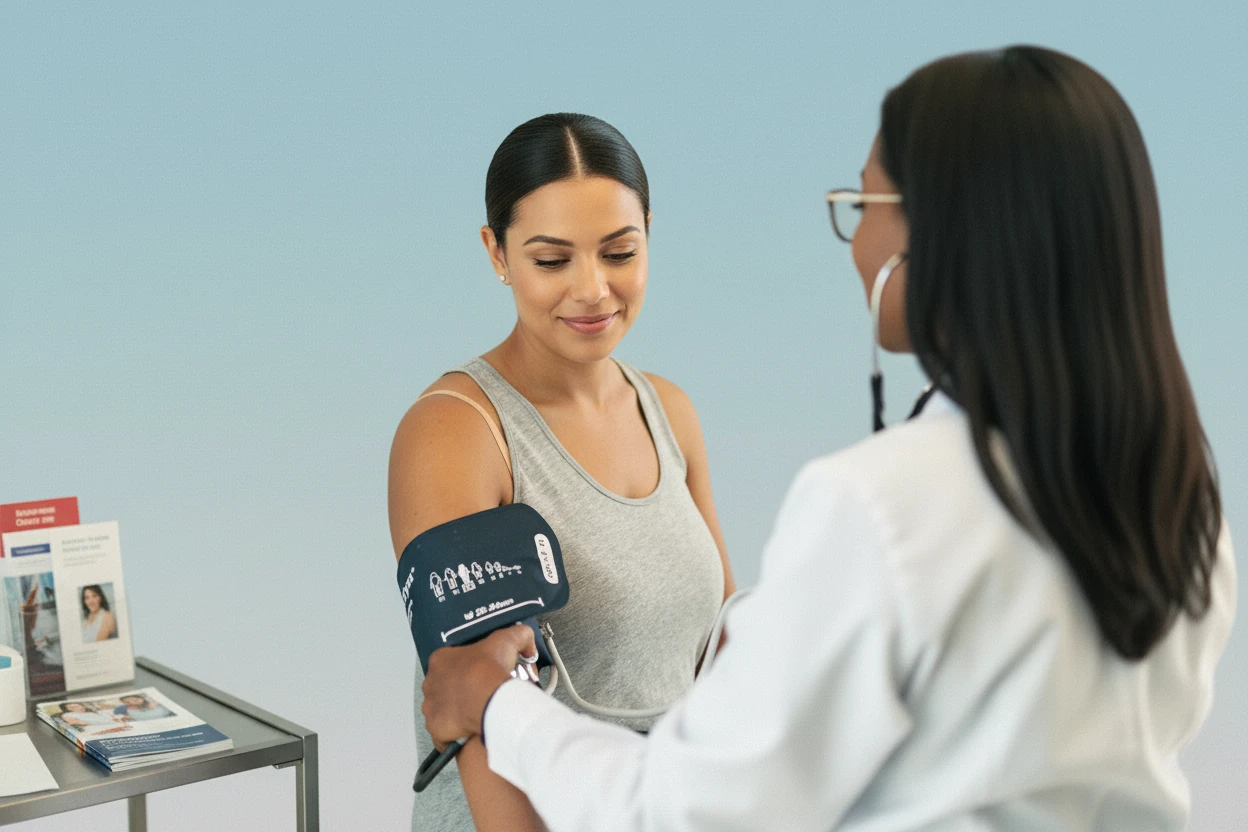
Blood pressure readings can vary significantly depending on how your arm is positioned during measurement. Commonly used arm positions, such as resting the arm on the lap or letting it hang unsupported by the side, can lead to substantial overestimations of blood pressure. These inaccuracies may cause misdiagnosis of hypertension and unnecessary treatment1 2. Understanding the impact of arm positioning is essential for accurate blood pressure assessment and proper clinical management1 .
Arm Positions and Blood Pressure Results
The position of the arm during blood pressure measurement plays a crucial role in the accuracy of the readings. A randomized crossover trial involving 134 middle-aged adults showed that blood pressure readings differed markedly depending on whether the arm was supported at heart level, resting on the lap, or hanging unsupported by the side3 . When the arm was supported on a desk at heart level—the recommended position—blood pressure readings served as the reference standard3 .
Blood pressure increased progressively when the arm was positioned lower than heart level. Resting the arm on the lap caused systolic and diastolic pressures to be overestimated by approximately 3.9 mm Hg and 4.0 mm Hg, respectively3 1. When the arm hung unsupported at the side, systolic pressure was overestimated by about 6.5 mm Hg, and diastolic pressure by 4.4 mm Hg3 12. Among individuals with hypertension, the overestimation of systolic pressure reached up to 9 mm Hg when the arm was unsupported at the side2 4.
“The findings confirm that arm position makes a 'huge difference' when it comes to an accurate blood pressure measurement.”
— Tammy Brady, Johns Hopkins University School of Medicine1
These differences are clinically significant. For example, an overestimation of 6.5 mm Hg in systolic blood pressure can shift a reading from 123 mm Hg to 130 mm Hg, or from 133 mm Hg to 140 mm Hg, potentially reclassifying a patient from normal or stage 1 hypertension to stage 2 hypertension1 . Such misclassification may lead to unnecessary medication and increased risk of side effects.
| Arm Position | Systolic BP Overestimation (mm Hg) | Diastolic BP Overestimation (mm Hg) | Notes |
|---|---|---|---|
| Supported at heart level | 0 (reference) | 0 (reference) | Recommended position3 5 |
| Arm resting on lap | ~3.9 | ~4.0 | Commonly used but causes overestimation3 15 |
| Arm hanging at side | ~6.5 | ~4.4 | Largest overestimation; especially in hypertensive patients3 124 |
Proper arm support at heart level is essential to avoid these errors and ensure accurate blood pressure measurement6 5.
“If you are consistently measuring blood pressure with an unsupported arm, and that gives you an overestimated BP of 6.5 mmHg, that's a potential difference between a systolic BP of 123 and 130, or 133 and 140 — which is considered stage 2 hypertension.”
— Sherry Liu, Johns Hopkins Bloomberg School of Public Health1
How Arm Position Changes Blood Pressure
The reason arm position affects blood pressure readings lies mainly in the hydrostatic pressure effect and muscle activity. Blood pressure reflects the force exerted by circulating blood on the walls of arteries, with systolic pressure indicating pressure during heart contraction and diastolic pressure during heart relaxation7 .
When the arm is positioned below heart level, gravity increases the hydrostatic pressure in the blood vessels of the arm. This pressure gradient in a closed fluid system causes blood pressure readings to be artificially elevated6 8. The ARMS trial demonstrated that unsupported arm positions caused overestimations of systolic and diastolic pressures by up to 6.5 and 4.4 mm Hg, respectively3 .
Additionally, muscle contraction during unsupported arm positions can increase vascular resistance, further elevating blood pressure readings3 6. Unsupported arms require muscle activity to maintain position, which can raise vascular tone and pressure compared to a fully supported arm.
“A person may feel perfectly fine, yet have dangerously elevated blood pressure. The only way to know that one's blood pressure is normal is by measuring it.”
— Ian Del Conde Pozzi, Baptist Health Miami Cardiac & Vascular Institute5
These physiological factors explain why blood pressure readings taken with the arm hanging or resting unsupported tend to be higher than those taken with the arm supported at heart level. This hydrostatic effect is similar to the pressure changes experienced underwater, where pressure increases with depth due to gravity6 .
Clinical guidelines emphasize that blood pressure should be measured with the arm supported at heart level to minimize these hydrostatic and muscular effects and avoid misclassification of hypertension6 9.
- Hydrostatic pressure increases with vertical distance below heart level, raising BP readings8 6.
- Muscle contraction in unsupported arm positions elevates vascular resistance and BP3 6.
- Blood pressure measurement errors due to arm position can lead to hypertension misdiagnosis9 .
- Even small measurement errors can affect treatment decisions and patient outcomes9 .
- Proper arm positioning reduces variability and improves measurement reliability9 7.
“For the most accurate reading, the arm should be supported on a desk or surface, with the middle of the cuff aligned with the level of the heart.”
— Ian Del Conde Pozzi, Baptist Health Miami Cardiac & Vascular Institute5
Accurate Blood Pressure Measurement Steps
Accurate blood pressure measurement requires standardized techniques that address arm position, patient posture, and environmental factors. Adhering to these steps helps reduce variability and prevents misdiagnosis or overtreatment of hypertension9 7.
💡 Did You Know? Commonly used ways of positioning the patient's arm during blood pressure screenings can substantially overestimate test results and may lead to misdiagnosis of hypertension. Lap support overestimated systolic pressure by nearly 4 mm Hg, and an unsupported arm hanging at the side overestimated systolic pressure by nearly 7 mm Hg1 .
- Position the arm supported at heart level: Rest the arm on a desk or table so that the middle of the blood pressure cuff is aligned with the heart3 95.
- Use the correct cuff size: Ensure the cuff fits the upper arm properly, with the bladder centered over the brachial artery10 9.
- Patient posture: Sit with back supported, feet flat on the floor, and legs uncrossed9 11.
- Prepare the patient: Avoid stimulants like caffeine, tobacco, and exercise for at least 30 minutes before measurement. Have the patient rest quietly for five minutes9 12.
- Measure on a bare arm: Place the cuff directly on the skin, not over clothing, to avoid inaccurate readings13 .
- Take multiple readings: Measure blood pressure in triplicate and average the results to improve accuracy3 .
- Avoid talking and movement: The patient should remain still and silent during measurement to prevent transient BP elevation11 .
Additional factors influencing accuracy include avoiding a full bladder, which can raise systolic pressure by 10 to 15 mm Hg, and minimizing the white coat effect by considering home or ambulatory blood pressure monitoring12 1415.
- Training and periodic recertification of healthcare providers improve measurement quality16 .
- Common deviations from protocols in clinical practice can lead to inaccurate readings16 .
- Home blood pressure monitoring is valuable for confirming hypertension diagnosis and reducing white coat effect15 .
- Consistent use of proper technique is critical for appropriate hypertension management9 7.