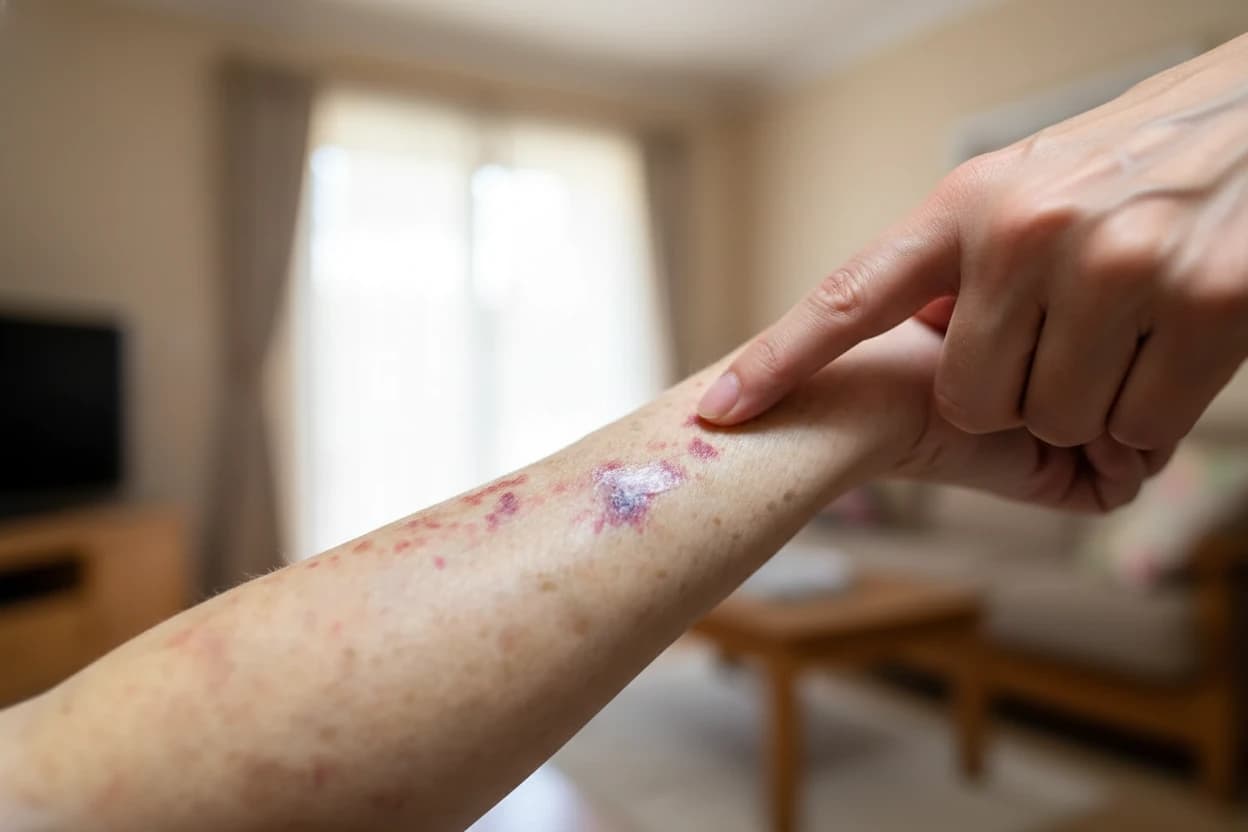
Venous stasis dermatitis is a common skin condition that affects millions of adults, especially those over 50 years old1 . It occurs when blood pools in the lower legs due to poor vein function, leading to swelling, skin discoloration, and discomfort1 . If left untreated, this condition can progress to more serious complications such as venous ulcers and infections2 . Understanding the symptoms, causes, diagnosis, and treatment options is essential for managing venous stasis effectively3 .
Venous Stasis Symptoms and Signs
Venous stasis dermatitis is a chronic inflammatory skin disease primarily affecting the lower legs. It typically presents with nonspecific symptoms such as itching (pruritus), dry skin (xerosis), aching legs, and areas of skin discoloration or dyspigmentation4 . The skin changes often include redness, scaling, and thickening, with the acute phase showing erythema and crusting, while the chronic phase is marked by hemosiderin (iron pigment) deposition causing brownish hyperpigmentation5 .
Common signs and symptoms include:
- Skin discoloration ranging from red to brown, often around the ankles and lower legs3
- Itching and dryness that can be persistent and bothersome3
- Scaling and thickened skin patches3
- Aching or heavy sensation in the legs, especially after prolonged standing or sitting4
- Swelling in the legs that typically improves with leg elevation or overnight rest4
- Presence of varicose veins and edema (leg swelling) 5
These symptoms can be debilitating, affecting quality of life and leading to further complications if untreated6 . The skin may also develop blisters, oozing, or crusting in severe cases, and the legs can take on a characteristic "upside-down bowling pin" shape due to chronic swelling and skin changes7 .
Venous stasis dermatitis causes swelling and pressure in the lower legs, leading to skin redness, itchiness, and a heavy or achy feeling. Without treatment, it can cause sores that may become infected1 .
Causes of Venous Stasis
Venous stasis results from chronic venous insufficiency (CVI), a condition where the valves in the leg veins become damaged or incompetent, allowing blood to pool and increase pressure in the veins2 . This venous hypertension leads to leakage of fluids and blood cells into surrounding tissues, triggering inflammation and skin changes characteristic of stasis dermatitis8 .
Key causes and risk factors include:
- Venous reflux: Incompetent venous valves fail to prevent backward blood flow, causing increased hydrostatic pressure in leg veins2
- Venous obstruction: Chronic occlusion of major veins such as the common iliac or femoral veins can impair blood flow and cause stasis9
- Age: Older adults are more prone due to natural valve degeneration and vein dilation8
- Deep vein thrombosis (DVT): Previous blood clots damage valves and increase risk of venous stasis10
- Prolonged sitting or standing: Immobility reduces calf muscle pump function, worsening venous return10
- Obesity and pregnancy: Both increase pressure on leg veins, contributing to valve incompetence10
- Genetic predisposition: Family history of venous disease increases susceptibility10
- Insufficient walking or physical activity: Sedentary lifestyle promotes blood pooling in legs10
Venous stasis can also be secondary to conditions or injuries affecting blood flow in the legs, such as surgery or trauma3 . The resulting venous hypertension promotes local inflammation and skin damage, leading to the clinical manifestations of stasis dermatitis2 .
Chronic venous insufficiency (CVI) occurs when the valves in leg veins are damaged and cannot function properly, leading to blood pooling in the legs instead of flowing back to the heart11 .
Diagnosing Venous Stasis
Diagnosis of venous stasis dermatitis is primarily clinical, based on a healthcare provider’s examination of the skin and review of the patient's medical history12 . The history often includes questions about heart problems, blood clots, stroke, medications, recent leg injuries, or surgeries that may contribute to venous insufficiency3 .
Additional diagnostic tools may include:
- Ultrasound (venous duplex scan): To assess venous valve function, detect reflux, and rule out blood clots3
- CT scan or MRI: Occasionally used to evaluate deeper venous structures or exclude other causes of leg swelling3
- Allergy testing: To differentiate stasis dermatitis from allergic contact dermatitis, which commonly coexists3
The diagnosis can be challenging because stasis dermatitis shares features with other skin conditions such as cellulitis, contact dermatitis, and fungal infections13 . Imaging helps confirm venous reflux or obstruction and guides treatment planning3 .
Venous Stasis Treatment Options
Effective management of venous stasis dermatitis targets both the underlying venous insufficiency and the skin symptoms. Treatment is multidisciplinary and includes conservative measures, medications, and sometimes surgical interventions.
Swelling
Reducing leg swelling is a cornerstone of therapy. Key strategies include:
- Compression therapy: Use of compression stockings or bandages to improve venous return and reduce venous pressure3
- Leg elevation: Raising legs above heart level to facilitate blood drainage and decrease edema3
- Physical activity: Light exercises such as walking to activate the calf muscle pump and enhance circulation3
These measures help relieve discomfort, reduce swelling, and prevent progression of skin changes6 .
Blood Flow
Improving blood flow in the legs is essential to prevent blood pooling and venous hypertension:
- Compression therapy and leg elevation both aid venous return3
- Exercise encourages circulation and prevents stasis3
- Avoiding prolonged immobility reduces risk of worsening venous insufficiency10
Medications
Medications may be used to manage inflammation and secondary skin symptoms:
- Topical corticosteroids: To reduce inflammation and itching in affected skin areas3
- Antibiotics: Prescribed if secondary bacterial infections or cellulitis develop3
- Anti-inflammatory agents: Occasionally used to address venous inflammation3
Currently, no treatments are specifically approved for the skin symptoms of stasis dermatitis, highlighting the need for new therapeutic options3 .
Intense Pulsed Light
There is limited evidence regarding the use of intense pulsed light (IPL) therapy for venous stasis or stasis dermatitis. IPL is not a standard treatment and requires further research before recommendation.
Surgery and Procedures
In some cases, surgical or interventional procedures may be necessary to correct underlying venous reflux or obstruction:
- Vein surgery: To repair or remove incompetent veins causing venous hypertension3
- Endovenous ablation: Minimally invasive techniques to close damaged veins3
- Stenting: For chronic venous occlusions such as iliac vein stenosis9
These interventions aim to restore proper venous flow and prevent disease progression2 .
Compression therapy and leg elevation are primary treatments for chronic venous insufficiency and stasis dermatitis, helping to reduce swelling and improve blood flow in the legs6 .
Preventing Venous Stasis
Prevention focuses on managing risk factors and maintaining healthy venous circulation. Recommended measures include:
- Avoiding prolonged sitting or standing to prevent blood pooling3
- Engaging in regular light physical activity such as walking to promote circulation3
- Quitting smoking to reduce vascular stress3
- Maintaining a healthy weight to decrease pressure on leg veins3
- Moisturizing legs and feet regularly to prevent skin dryness and cracking3
- Managing blood pressure, blood sugar, and cholesterol levels to support vascular health3
Addressing sedentary lifestyle and obesity can significantly reduce the risk of developing venous stasis-related skin lesions10 .
Venous Stasis Complications
If untreated, venous stasis dermatitis can lead to serious complications, including:
- Venous ulcers: Open sores that develop due to chronic skin breakdown and poor healing2
- Contact dermatitis: Allergic reactions to topical treatments or irritants, common in stasis dermatitis patients6
- Superinfections: Bacterial or fungal infections facilitated by skin breaks and ulcers3
- Cellulitis: A potentially serious bacterial skin infection3
- Chronic pain and disability: Due to persistent swelling and skin changes6
Skin inflammation and itching can cause scratching, leading to minor skin breaks that increase infection risk3 . Allergic contact dermatitis occurs in a large proportion of patients and may complicate management6 .
Venous stasis syndrome clinically presents as chronic dependent leg edema with leg pain, skin hyperpigmentation, and induration; in severe cases, venous ulcers may develop14 .
Managing Life with Venous Stasis
Living with venous stasis requires ongoing management to control symptoms and prevent complications. Key strategies include:
- Consistent use of compression stockings or bandages to reduce leg swelling3
- Regular leg elevation to aid blood flow3
- Maintaining physical activity to improve circulation3
- Using prescribed topical corticosteroids to manage skin inflammation3
- Monitoring skin for signs of infection or ulceration and seeking prompt medical care3
While venous stasis cannot be cured due to irreversible valve damage, symptoms can be effectively managed to improve quality of life3 .
Stasis dermatitis is a chronic inflammatory skin condition of the lower extremities, typically occurring in older adults, and is a cutaneous manifestation of venous hypertension caused by venous reflux13 .
Venous Stasis FAQs
Can venous stasis dermatitis be cured?
Damage to vein valves caused by venous stasis cannot be reversed, but symptoms can be managed with treatments like compression stockings, anti-inflammatory medication, and exercise3 .
What happens if stasis dermatitis is left untreated?
If undiagnosed or untreated, stasis dermatitis may progress to venous ulcers, which are difficult to heal and prone to infection2 .
How can I reduce swelling in my legs?
Light physical activity such as walking, leg elevation, and wearing compression stockings can help reduce swelling by improving blood flow3 .
Are there any lifestyle changes that help?
Yes, quitting smoking, managing weight, exercising regularly, and moisturizing the skin are important preventive and management strategies3 .