Staphylococcus aureus, commonly known as staph, is a bacterium found on the skin and in the noses of about 30% of people without causing harm1 . While many staph infections are mild and treatable, these bacteria can sometimes cause serious and even life-threatening illnesses if they enter deeper tissues or the bloodstream2 . Antibiotic resistance, especially in strains like MRSA, complicates treatment and increases the risk of severe outcomes3 .
Types of Staph Infections
Staphylococcus aureus is the most clinically significant species among over 30 identified staphylococci species4 . It causes a wide range of infections, from minor skin conditions to severe systemic diseases5 . Strains of S. aureus are classified based on their antibiotic resistance profiles:
- Methicillin-Susceptible Staphylococcus aureus (MSSA): These strains are susceptible to methicillin and related beta-lactam antibiotics and typically cause skin and soft tissue infections that are generally more treatable6 7.
- Methicillin-Resistant Staphylococcus aureus (MRSA): MRSA strains carry the mecA gene, which confers resistance to methicillin and related beta-lactam antibiotics. MRSA frequently spreads in healthcare settings, causing more difficult-to-treat infections7 89.
- Vancomycin-Intermediate Staphylococcus aureus (VISA): These strains show intermediate resistance to vancomycin, complicating treatment, and often occur in patients with prior healthcare exposure, such as surgery or indwelling devices10 .
- Vancomycin-Resistant Staphylococcus aureus (VRSA): VRSA strains exhibit full resistance to vancomycin and are associated with healthcare exposure and underlying comorbidities like lung disease, posing serious treatment challenges10 .
Staph infections can be community-acquired or hospital-acquired, with hospital-associated MRSA (HA-MRSA) primarily transmitted in healthcare settings8 . The diversity of strains and resistance patterns makes diagnosis and treatment complex11 .
Staph Infection Symptoms
Symptoms of staph infections depend largely on the site and severity of the infection. They range from localized skin issues to systemic signs affecting multiple organs5 .
Skin Symptoms
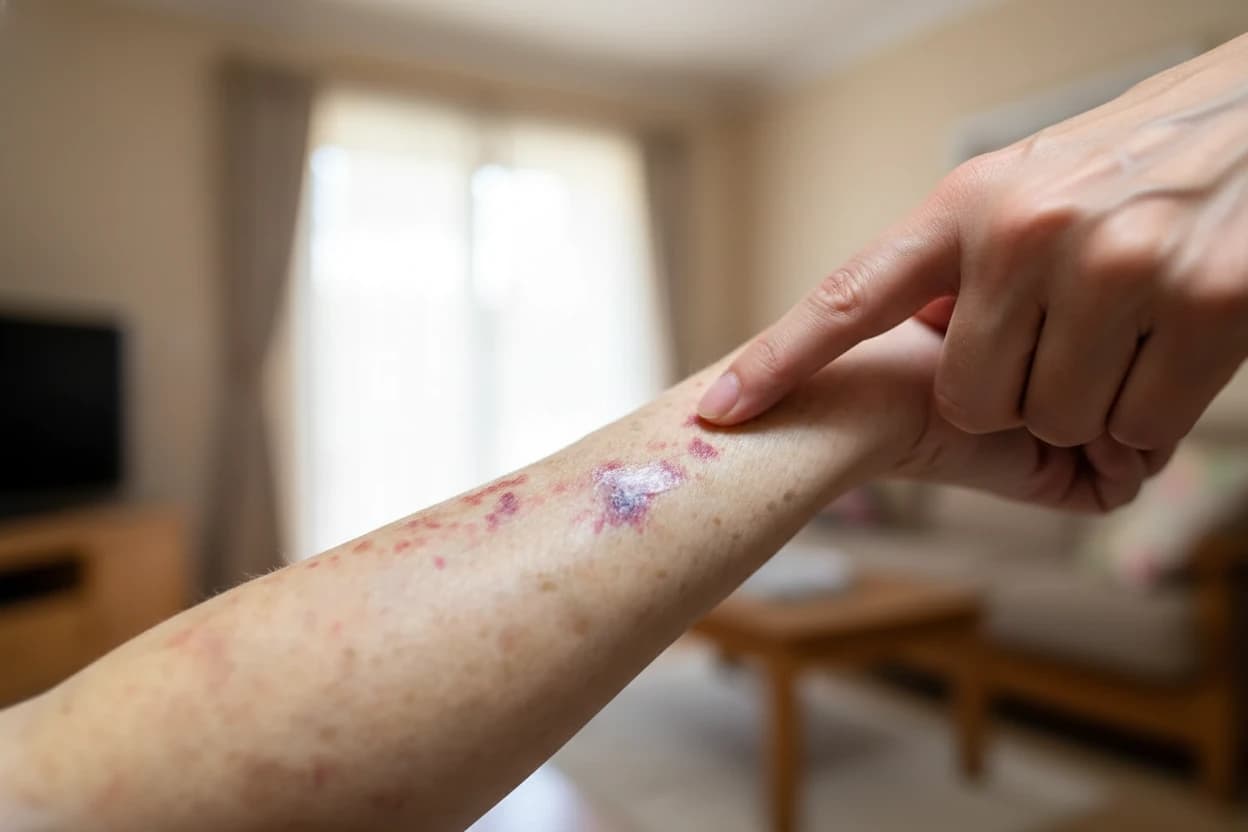
Skin and soft tissue infections are the most common presentation of S. aureus infection6 . These infections often start where the skin is damaged or broken2 . Common skin symptoms include:
- Abscesses or boils: painful, swollen lumps filled with pus that may rupture12 13.
- Impetigo: contagious sores, especially in children, characterized by honey-colored crusted lesions14 2.
- Cellulitis: red, swollen, warm, and painful areas of skin12 .
- Folliculitis: inflammation of hair follicles causing red, itchy bumps resembling pimples12 .
- Furuncles and carbuncles: deeper pockets of pus often found under the arms, groin, or buttocks2 15.
The infected skin may become discolored, swollen, warm, painful, and sometimes blistered or raw2 . Pus from these infections contains bacteria that can spread to others12 .
Blood Symptoms
When staph bacteria enter the bloodstream, it causes bacteremia, which can progress to sepsis, a life-threatening systemic infection16 2. Symptoms of bloodstream infection include:
- Fever or chills16 .
- Rapid heart rate (tachycardia) 16.
- Low blood pressure (hypotension) 16.
- Confusion or disorientation2 .
- Cold, sweaty skin and severe pain2 .
Sepsis requires urgent medical attention to prevent organ failure and death16 .
Digestive Symptoms
Staphylococcal enterotoxins in contaminated food can cause food poisoning, leading to rapid-onset digestive symptoms17 2. These include:
- Nausea and vomiting2 .
- Stomach cramps2 .
- Diarrhea17 2.
Symptoms usually appear within hours of eating contaminated food and typically resolve without antibiotics2 .
Heart Symptoms
S. aureus can infect the heart valves, causing infective endocarditis, a serious condition16 . Symptoms may include:
- Fever and sweating2 .
- Rapid heartbeat16 .
- Weight loss2 .
- Shortness of breath16 .
Diagnosis often requires echocardiography to assess valve involvement16 .
Other Symptoms
Severe staph infections may cause toxic shock syndrome (TSS), characterized by sudden high fever, rash, muscle aches, vomiting, diarrhea, and confusion2 . Septic arthritis, an infection of the joints, presents with joint swelling, severe pain, and fever2 .
Causes of Staph Infections
Staph infections occur when S. aureus bacteria breach the skin or mucosal barriers and evade the immune system18 . These bacteria commonly colonize the anterior nares (inside the nose) and skin without causing symptoms19 . Infection can result from direct contact with infected wounds, secretions, or contaminated objects8 .
Risk Factors
Certain conditions and exposures increase the risk of developing staph infections:
- Broken skin from wounds, burns, trauma, or surgical procedures2 20.
- Presence of indwelling medical devices such as catheters or implants, which promote biofilm formation and infection19 .
- Chronic illnesses like diabetes, immunosuppression, vascular disease, and lung disease19 20.
- Recent hospitalization or healthcare exposure, especially in intensive care units or after surgery8 1.
- Dialysis treatment, which increases bloodstream infection risk19 .
- Injection drug use and contact sports, which facilitate skin-to-skin transmission1 3.
Staph bacteria can also spread through contaminated food, causing food poisoning17 .
Diagnosing Staph Infections
Diagnosis depends on the infection site and clinical presentation18 . Initial steps include a thorough medical history and physical examination18 . Laboratory tests may involve:
- Culture of clinical specimens, the gold standard for detecting S. aureus18 .
- Molecular assays such as PCR for rapid detection of staph DNA9 .
- Imaging studies like echocardiography for suspected endocarditis16 .
- CT scans to identify abscesses or organ involvement in invasive infections18 .
- Chest X-rays to evaluate pulmonary complications21 .
Because S. aureus commonly colonizes skin and mucous membranes without causing infection, laboratory results must be interpreted carefully18 11.
Staph Infection Treatment
Treatment of staph infections varies with the infection type, severity, and antibiotic susceptibility of the strain18 . Management often combines antibiotics with supportive care and, when necessary, surgical intervention.
Topical Antibiotics
For localized skin infections, topical antibiotics are effective6 . Common agents include:
- Mupirocin18 .
- Fusidic acid18 .
Some topical antibiotics require prescriptions, while others may be available over the counter depending on the region6 .
Oral Antibiotics
Mild to moderate infections beyond the skin are treated with oral antibiotics18 . The choice depends on susceptibility:
- Beta-lactam antibiotics for MSSA infections18 .
- Vancomycin or linezolid for MRSA infections18 .
Completing the full course of antibiotics is essential to prevent resistance and recurrence11 .
Intravenous (IV) Antibiotic Therapy
Severe or disseminated staph infections require hospitalization and IV antibiotics18 . Treatment duration often extends to 4–6 weeks for deep or complicated infections like bacteremia or endocarditis16 . Vancomycin remains a mainstay for MRSA, although resistance is emerging10 .
Fluid Drainage
Incision and drainage are critical for abscesses caused by S. aureus12 . This procedure must be performed by healthcare professionals to avoid complications12 . Drainage reduces bacterial load and improves antibiotic effectiveness.
“Folks are dying simply because there is no antibiotic available to treat their infection, infections that not too long ago were easily treatable.”
— Dr. Jean Altapure22
Staph Infection Prevention
Preventing staph infections focuses on minimizing contact with the bacteria and maintaining good hygiene8 . Key preventive measures include:
- Frequent handwashing with soap and water for at least 20 seconds8 .
- Using gloves and protective equipment in healthcare settings8 .
- Avoiding sharing personal items such as towels, razors, and athletic equipment8 .
- Proper wound care, including cleaning and covering wounds with sterile dressings8 .
- Safe food handling and preparation to prevent staphylococcal food poisoning17 .
These steps reduce bacterial transmission and infection risk in both community and healthcare environments8 .
Complications of Staph Infections
Untreated or severe staph infections can lead to serious complications, including:
- Sepsis, a life-threatening systemic inflammatory response16 .
- Infective endocarditis, damaging heart valves16 .
- Toxic shock syndrome, causing sudden high fever and organ failure16 .
- Embolic events, where infected clots travel to other organs16 .
Early diagnosis and treatment are essential to reduce the risk of these outcomes18 .
Key Points About Staph Infections
- Staphylococcus aureus is a common bacterium found on skin and in the nose of many healthy individuals1 .
- Most staph infections are skin-related and treatable with antibiotics6 .
- MRSA and other resistant strains pose significant treatment challenges10 3.
- Good hygiene, wound care, and safe food handling are critical for prevention8 17.
- Prompt medical evaluation and appropriate treatment reduce the risk of severe complications18 .
Staph Infection FAQs
What are the most common symptoms of a staph infection?
Most staph infections cause skin symptoms such as boils, abscesses, impetigo, and cellulitis. Systemic infections may cause fever, chills, and signs of sepsis12 16.
Can staph infections be serious?
Yes, if untreated, staph infections can spread to the bloodstream, heart, lungs, or bones, causing life-threatening conditions like sepsis and endocarditis16 2.
How do you prevent staph infections?
Prevention includes good hand hygiene, wound care, avoiding sharing personal items, and proper food safety practices8 17.
Are all staph infections resistant to antibiotics?
No, many staph infections are caused by methicillin-susceptible strains (MSSA) that respond well to common antibiotics. However, MRSA and other resistant strains require specific treatments7 3.
What should I do if I suspect a staph infection?
Seek medical care promptly, especially if the infection worsens, spreads, or is accompanied by fever or systemic symptoms18 2.