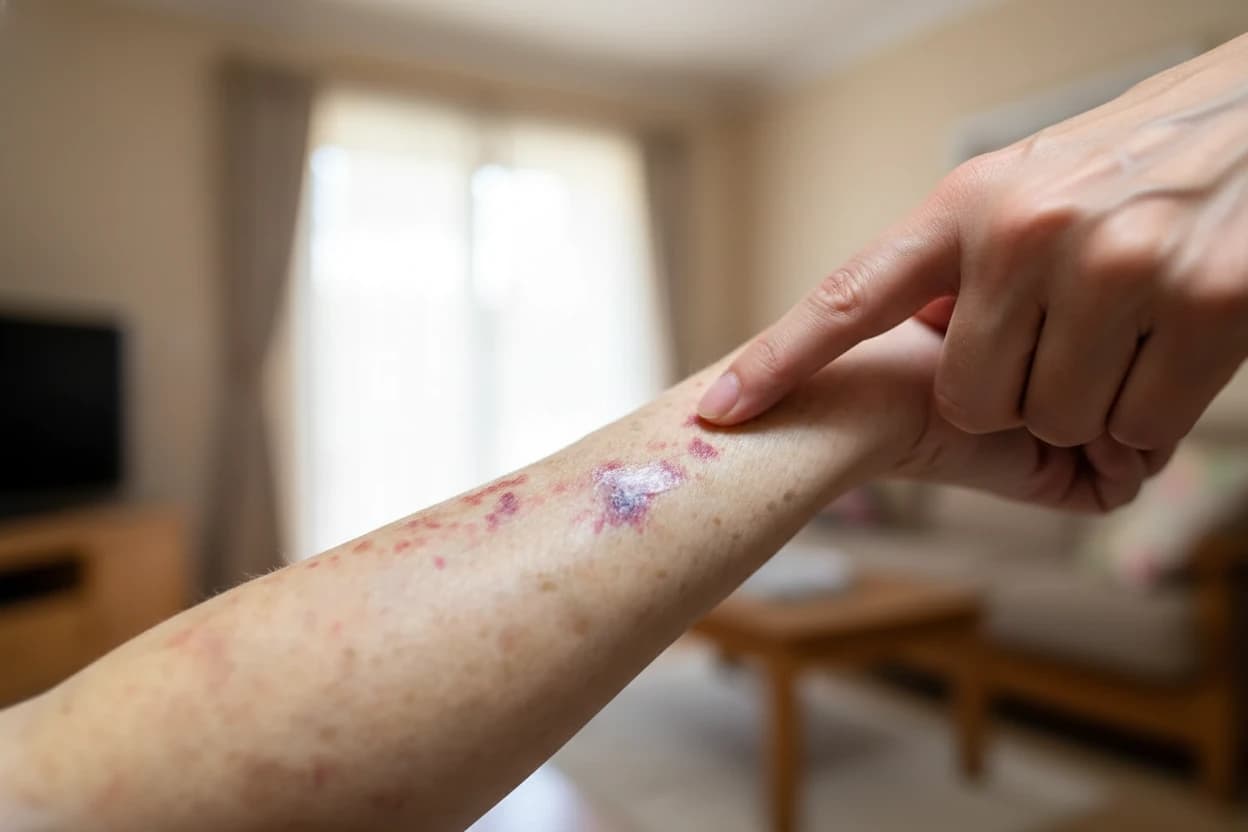
Shingles, also known as herpes zoster, is a viral infection caused by the reactivation of the varicella-zoster virus (VZV), the same virus responsible for chickenpox1 . It commonly affects older adults and individuals with weakened immune systems, presenting as a painful, blistering rash typically confined to a single dermatome2 3. Accurate and timely diagnosis is crucial for initiating antiviral treatment early, which can reduce symptom severity and prevent complications such as postherpetic neuralgia4 1.
Diagnostic Criteria for Shingles
Physical Exam
The diagnosis of shingles is primarily clinical and begins with a thorough physical examination5 . The hallmark sign is a painful, blistering rash that appears in a dermatomal distribution, usually on one side of the body1 . The rash often manifests as a single stripe of fluid-filled blisters that follow the path of a sensory nerve, most commonly on the trunk or face2 6. Prodromal symptoms such as tingling, itching, or numbness may precede the rash by several days7 .
Key physical exam features include:
- Unilateral, painful rash with clusters of vesicles on an erythematous base1 2
- Rash confined to one or two adjacent dermatomes without crossing the midline8
- Possible involvement of the ophthalmic branch of the trigeminal nerve, which requires urgent ophthalmologic evaluation to prevent vision loss7 8
- In immunocompromised patients, disseminated shingles may present with widespread lesions beyond the primary dermatome9
Physical examination alone has a high positive predictive value (approximately 90.8%) for diagnosing herpes zoster10 . The presence of a characteristic rash combined with pain in a dermatomal pattern is usually sufficient for diagnosis1 10.
Medical History
A detailed medical history complements the physical exam and helps confirm the diagnosis. Important historical elements include:
- Previous varicella (chickenpox) infection, as shingles results from reactivation of dormant VZV in sensory ganglia1 3
- Onset and progression of symptoms, including prodromal pain, burning, or tingling sensations before rash appearance7 3
- Immunosuppressive conditions or treatments that increase shingles risk, such as HIV infection, cancer, or immunosuppressive medications2 3
- Age over 50 years, as risk increases with advancing age due to declining cell-mediated immunity2 3
- History of similar episodes or prior shingles infections, as recurrence is possible though uncommon8
The medical history also helps differentiate shingles from other conditions that may mimic its presentation, such as herpes simplex virus infection, contact dermatitis, or bacterial skin infections11 12.
Shingles Tests and Procedures
While clinical diagnosis is often sufficient, laboratory tests may be necessary in atypical or unclear cases13 . Tests help confirm VZV infection and exclude other causes of rash or pain.
“The incidence of herpes zoster ranges from 1.2 to 3.4 per 1000 persons per year among younger healthy individuals, while it ranges from 3.9 to 11.8 per 1000 persons per year among patients older than 65 years.”
— Pragya A. Nair, University of Utah3
Common diagnostic tests include:
- Polymerase Chain Reaction (PCR): Detects VZV DNA in vesicular fluid, blood, cerebrospinal fluid (CSF), or skin scrapings with high sensitivity and specificity13 1415. PCR is the preferred confirmatory test, especially in cases without typical rash or in immunocompromised patients13 .
- Direct Fluorescent Antibody (DFA) Testing: Used on vesicular or corneal fluid to identify VZV antigens, particularly in ocular involvement13 16.
- Tzanck Smear: Microscopic examination of blister fluid showing multinucleated giant cells; less sensitive and specific than PCR3 .
- Serological Tests: Detection of VZV-specific IgM antibodies may indicate active infection, but serology is less useful for acute diagnosis13 .
- Skin Sampling: Swabbing the base of a blister with synthetic fiber swabs (e.g., polyester) or scraping lesions for PCR analysis17 .
- Electromyography (EMG) and Nerve Conduction Velocity (NCV): Occasionally used to assess nerve damage in complicated cases17 .
- Lumbar Puncture (Spinal Tap): CSF analysis may be performed if central nervous system involvement is suspected17 .
- Magnetic Resonance Imaging (MRI): Imaging of brain or spinal cord may be indicated in neurological complications17 .
Laboratory testing is particularly important when the rash is absent (zoster sine herpete), the presentation is atypical, or when complications such as meningitis or encephalitis are suspected14 1518.
Early recognition and appropriate testing are crucial to avoid misdiagnosis and ensure timely treatment, especially in atypical presentations or immunocompromised patients13 4.
Screening for Related Conditions
Shingles diagnosis should prompt screening for related conditions and complications, especially in high-risk populations.
Key considerations include:
- Immunosuppression: Patients with weakened immune systems are at increased risk for severe or disseminated shingles and complications2 9. Screening for HIV or other immunodeficiencies may be warranted in younger patients or those with recurrent shingles19 .
- Ophthalmic Involvement: Herpes zoster ophthalmicus requires urgent ophthalmologic evaluation to prevent vision loss and manage keratitis, uveitis, or optic nerve palsies7 168.
- Neurological Complications: Shingles can cause cranial nerve palsies, myelitis, meningitis, or encephalitis. Neurological assessment and imaging may be necessary if symptoms suggest central nervous system involvement3 18.
- Postherpetic Neuralgia (PHN): Persistent nerve pain following shingles rash resolution is common, especially in older adults. Early antiviral treatment may reduce acute pain but does not conclusively prevent PHN1 419.
- Differential Diagnoses: Conditions that can mimic shingles include herpes simplex virus infection, bacterial skin infections (e.g., impetigo), contact dermatitis, folliculitis, scabies, and candidiasis11 12. Accurate differentiation is essential to guide appropriate treatment.
Screening for these conditions ensures comprehensive care and reduces the risk of long-term complications.
“Antiviral medicines may reduce the duration of the rash and associated pain, however, they do not reduce the risk of patients developing post-herpetic neuralgia, the most common long-term complication of shingles.”
— Mark Thomas, Associate Professor, University of Auckland19
Shingles Diagnosis Overview
Shingles is a common viral infection with an incidence ranging from 1.2 to 3.4 per 1000 persons per year in younger healthy individuals and 3.9 to 11.8 per 1000 persons per year in those over 65 years3 . It results from reactivation of VZV, which remains dormant in sensory ganglia after chickenpox infection1 3.
The clinical course typically involves three stages:
- Preeruptive Stage: Prodromal symptoms such as burning pain, tingling, or itching in the affected dermatome appear 48 hours before rash onset, often accompanied by malaise or fever7 3.
- Acute Eruptive Phase: Painful vesicular rash develops unilaterally in one or more dermatomes. Lesions evolve from erythematous papules to vesicles, which rupture and crust over within 2–4 weeks1 3.
- Chronic Phase: Some patients experience postherpetic neuralgia, characterized by persistent neuropathic pain lasting months or years after rash resolution1 20.
Diagnosis is primarily clinical, based on the characteristic dermatomal rash and associated symptoms1 10. Laboratory confirmation by PCR or serology is reserved for atypical cases or when complications are suspected13 3.
Early diagnosis is essential to initiate antiviral therapy within 72 hours of rash onset, which can reduce rash duration, severity, and acute pain4 19. However, antiviral treatment does not conclusively prevent postherpetic neuralgia19 .
Differential diagnosis includes herpes simplex virus infection, bacterial skin infections, contact dermatitis, and other dermatological conditions that may mimic shingles11 12.