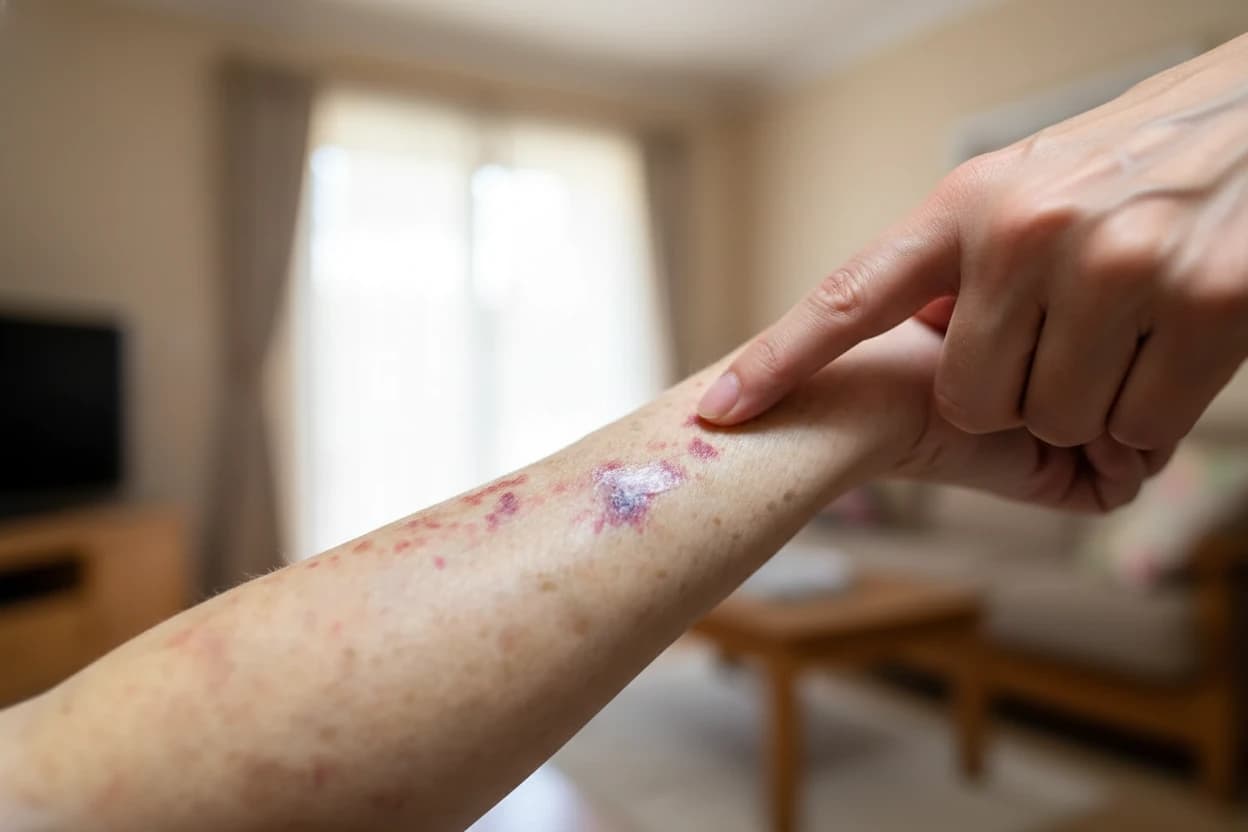
Shingles affects about one in three people in the United States during their lifetime, with roughly one million new cases annually1 2. This painful viral infection results from the reactivation of the varicella-zoster virus (VZV), the same virus responsible for chickenpox1 3. While shingles can occur at any age, its incidence rises sharply after age 50, especially among those with weakened immune systems4 5. Understanding the causes and risk factors of shingles is crucial for prevention and timely treatment.
Is Shingles Genetic?
Shingles arises from the reactivation of latent varicella-zoster virus in nerve cells, primarily triggered by immune system decline rather than clear hereditary patterns6 7. Although some studies suggest a weak genetic link, the role of genetics in shingles susceptibility remains uncertain and requires further research7 8. Family history and specific gene variants, particularly in the human leukocyte antigen (HLA) region such as HCP5 and HLA-B, have been associated with increased risk, but the exact genetic mechanisms are not fully understood9 107.
Meta-analyses indicate that having multiple first-degree relatives with shingles markedly increases individual risk, suggesting some hereditary influence11 10. However, some HLA gene variants may also confer protective effects against shingles7 . Overall, the interplay between genetics, aging, and immune status complicates risk assessment, and more genetic studies are needed to clarify hereditary contributions7 12.
Shingles Risk Groups
Anyone who has had chickenpox or received the varicella vaccine can develop shingles because the virus remains dormant in the nervous system6 71. However, certain groups are at higher risk:
- Older adults: Shingles incidence increases significantly after age 50, with half of cases occurring in people aged 60 or older. By age 85, about 50% of individuals will have experienced shingles4 57.
- Ethnic groups: Non-Hispanic Whites have higher incidence rates of shingles compared to other ethnicities5 7.
- Gender: Females consistently show about 28% higher incidence of shingles than males, though the reasons for this disparity are unclear13 1.
- Immunocompromised individuals: People with weakened immune systems due to disease or treatment are at the greatest risk7 23.
This risk profile highlights the importance of targeted prevention and vaccination efforts in these populations.
“Shingles is caused by the varicella zoster virus. The name reflects two different conditions caused by the same virus: varicella (chickenpox) and zoster (shingles).”
— Ankush Bansal, MD, American Medical Association1
Shingles Risk Factors Explained
Shingles results from the reactivation of VZV, which lies dormant in sensory ganglia after initial chickenpox infection or vaccination6 7. Various factors can trigger this reactivation by weakening the immune system or causing nerve inflammation.
Cancer
Cancer patients, especially those with hematologic malignancies like leukemia and lymphoma, have a significantly increased risk of shingles14 7. The risk peaks within the first year after cancer diagnosis and is about 40% higher than in the general population14 . Cancer treatments such as chemotherapy and radiation further suppress immunity, increasing susceptibility and the likelihood of hospitalization due to shingles complications14 7.
Human Immunodeficiency Virus (HIV)
HIV infection impairs cellular immunity, increasing shingles risk by 12 to 17 times compared to the general population4 7. This immune suppression facilitates VZV reactivation. Shingles occurring in younger or atypical patients may prompt HIV testing to identify underlying immunodeficiency4 .
Diabetes
Diabetes mellitus increases shingles risk by approximately 60%, likely due to immune dysregulation associated with the disease5 7. Poorly controlled blood sugar levels can impair the body's ability to fight infections, making reactivation of VZV more likely5 .
Immunosuppressive Treatments
Medications that suppress the immune system, such as long-term corticosteroids, biologic agents for autoimmune diseases, or drugs to prevent organ transplant rejection, increase shingles risk7 1. Immunosuppression is the strongest risk factor for shingles and its complications, including hospitalization and death7 15.
Physical Trauma
Physical trauma, including head injuries, has been linked to increased shingles risk, particularly in older adults1 7. The exact mechanism is unclear, but trauma may trigger nerve inflammation or immune changes that facilitate VZV reactivation1 .
Stress
Shingles affects about one in three people in the U.S. during their lifetime, with most cases occurring after age 50. Immunosuppression and aging are the strongest risk factors for shingles and its complications1 23.
Both physical and psychological stress can trigger shingles by weakening immune defenses6 71. Illness, injury, or severe mental stress may precipitate viral reactivation, leading to shingles outbreaks1 .
- Age over 50 years is the strongest risk factor for shingles4 .
- Immunosuppression from disease or therapy significantly increases risk and severity7 .
- Cancer, especially hematologic malignancies, raises shingles risk and hospitalization rates14 .
- HIV infection increases risk 12–17-fold by impairing cellular immunity4 .
- Diabetes mellitus increases shingles susceptibility by about 60% 5.
- Physical trauma and stress can trigger shingles by weakening immune defenses6 71.
Early treatment with antiviral medications can shorten the duration of shingles and reduce complications such as postherpetic neuralgia, a common and painful long-term nerve condition16 6.
Shingles Key Takeaways
- Shingles is caused by reactivation of the varicella-zoster virus, which remains dormant after chickenpox or vaccination6 7.
- The risk of shingles increases with age, especially after 50 years, and is higher in women and non-Hispanic Whites4 513.
- Immunosuppression is the most significant risk factor, with cancer, HIV, diabetes, and immunosuppressive treatments markedly increasing susceptibility14 45.
- Physical trauma and stress can also trigger shingles by weakening immune function6 71.
- Genetic factors may play a minor role, but the hereditary link is weak and not fully understood11 107.