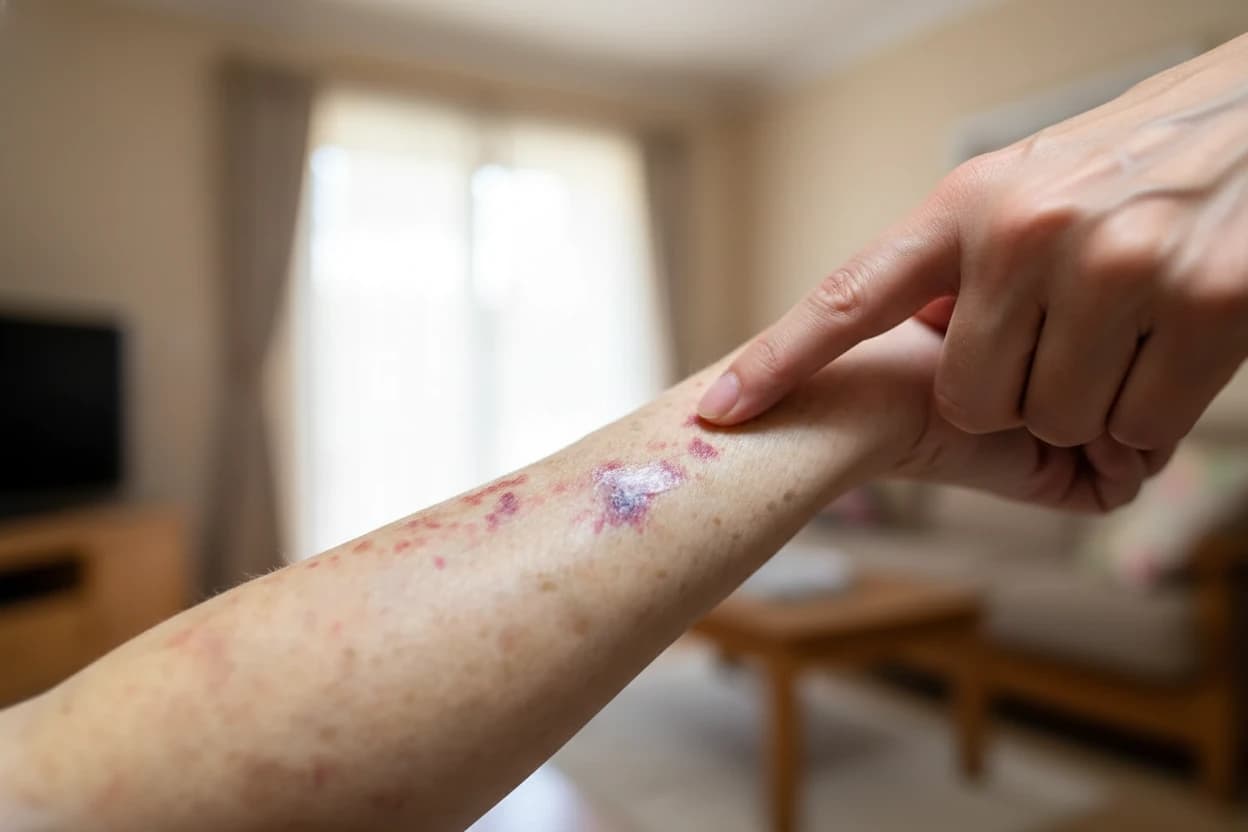
Merkel cell carcinoma (MCC) is a rare but aggressive skin cancer that affects about 3,000 people annually in the United States1 . It most commonly occurs in older adults, especially those over 50, and tends to grow rapidly and spread to other parts of the body2 1. Early detection and treatment are critical because MCC often appears as a painless bump on sun-exposed areas such as the face, head, or neck2 3.
Types of Skin Cancer
Skin cancer includes several types, each with distinct characteristics and risks. Merkel cell carcinoma is an uncommon neuroendocrine tumor of the skin4 . Other common skin cancers include:
- Basal cell carcinoma: The most frequently diagnosed skin cancer in the U.S., often presenting as a non-healing sore or lesion5 .
- Squamous cell carcinoma: The second most common skin cancer, typically appearing as a persistent sore or scaly patch5 .
- Melanoma: The most dangerous form of skin cancer, usually manifesting as a pigmented or dark lesion on the skin5 .
Unlike basal and squamous cell carcinomas, Merkel cell carcinoma is rare but more aggressive, with a higher risk of early metastasis and worse prognosis5 3.
Merkel Cell Carcinoma Symptoms
Merkel cell carcinoma often begins as a solitary, painless nodule that grows quickly6 . The lesion is usually firm, red to violaceous (purple), and may appear on chronically sun-exposed areas such as the head, neck, and extremities6 7. Key symptoms include:
- Rapid enlargement of the lesion6 .
- Painless, firm nodules with red to purple coloring6 .
- Possible satellite nodules near the primary lesion6 .
- Ulceration and bleeding in advanced stages6 .
- Regional spread to nearby lymph nodes6 .
MCC lesions can be mistaken for insect bites, cysts, or pimples due to their appearance8 . In white individuals, lesions most often appear on the head or neck, while in Black individuals, they are more common on the legs2 1.
Merkel cell carcinoma often looks harmless at first, resembling a pimple or insect bite, but it grows rapidly and can spread quickly to lymph nodes and other organs. Early recognition of these painless, fast-growing bumps is essential for better outcomes3 8.
Causes and Risk Factors
Merkel cell carcinoma arises from uncontrolled growth of neuroendocrine cells in the skin, historically thought to be Merkel cells but now believed to originate from related precursor cells9 . The development of MCC involves genetic mutations and DNA damage, often caused by chronic ultraviolet (UV) exposure9 . Additionally, infection with Merkel cell polyomavirus (MCV) is detected in approximately 60-80% of MCC tumors9 .
Risk Factors
Several factors increase the risk of developing MCC:
- Age: Most patients are older than 50, with incidence rising in the elderly2 3.
- UV exposure: Chronic sun exposure causes DNA mutations that promote cancer development9 3.
- Merkel cell polyomavirus (MCV): A common virus that usually causes no symptoms but can drive tumorigenesis in some cases9 10.
- Immune suppression: Conditions or treatments that weaken the immune system increase MCC risk7 10.
- Skin type: Fair-skinned individuals are more susceptible, though MCC can occur in all skin types1 8.
- History of other skin cancers: Previous basal or squamous cell carcinomas raise the risk7 .
In most parts of the world, the majority of Merkel cell carcinomas (MCCs) are caused by the monoclonal integration of Merkel cell polyomavirus (MCPyV), and the remainder are associated with exposure to ultraviolet light10 .
Diagnosis and Staging
Diagnosis of Merkel cell carcinoma begins with a thorough skin examination by a dermatologist, including palpation of regional lymph nodes and a detailed medical history focusing on symptom duration and UV exposure5 . Definitive diagnosis requires a skin biopsy, which can be performed using various methods:
- Shave biopsy: Removal of superficial skin layers5 .
- Punch biopsy: Extraction of a cylindrical sample including deeper skin layers5 .
- Excisional biopsy: Complete removal of the lesion5 .
- Incisional biopsy: Partial removal of a larger lesion5 .
Immunohistochemical testing confirms the neuroendocrine nature of MCC11 . Because MCC frequently spreads to lymph nodes early, sentinel lymph node biopsy is an important staging tool to detect microscopic metastasis11 712.
Stages of Merkel Cell Carcinoma
Staging determines the extent of cancer spread and guides treatment decisions. The stages include:
| Stage | Description | Notes |
|---|---|---|
| 0 | Cancer confined to the epidermis (skin's outer layer) | Early, localized disease3 |
| I | Tumor ≤2 cm without lymph node involvement | Localized tumor3 |
| II | Tumor >2 cm without lymph node involvement | Larger localized tumor3 |
| III | Regional lymph node involvement | Cancer spread to nearby lymph nodes3 |
| IV | Distant metastasis to organs | Advanced disease with distant spread3 |
| Sources: 3 | ||
Early-stage MCC has a better prognosis, but many patients present with regional or distant metastases due to the cancer’s aggressive nature3 .
Sentinel lymph node biopsy is critical because MCC often spreads to lymph nodes before becoming clinically apparent. Early detection of nodal involvement improves treatment planning12 .
Merkel Cell Carcinoma Treatment
Treatment aims to achieve complete remission or cure when possible. Because MCC grows rapidly and metastasizes early, management often requires a combination of therapies5 13.
- Surgical excision: Wide local excision with 1 to 2 cm margins is the primary treatment for localized MCC5 . Mohs micrographic surgery may be used to precisely remove cancer while sparing healthy tissue5 .
- Sentinel lymph node biopsy and lymphadenectomy: Performed to assess and remove affected lymph nodes5 .
- Radiation therapy: Adjuvant radiotherapy after surgery reduces local recurrence and improves control5 13.
- Chemotherapy: Reserved for metastatic or unresectable cases; however, responses are often short-lived5 .
- Immunotherapy: Immune checkpoint inhibitors targeting PD-1/PD-L1 pathways have shown promising durable responses in advanced MCC10 .
Both virus-positive and virus-negative MCCs are immunogenic, and inhibition of the programmed cell death protein 1 (PD-1)–programmed death-ligand 1 (PD-L1) immune checkpoint has proved to be highly effective in treating patients with metastatic MCC; however, not all patients have a durable response to immunotherapy10 .
Early-stage MCC can often be cured with surgery and radiation, but advanced disease requires multimodal treatment12 .
Prevention Strategies
Preventing Merkel cell carcinoma focuses mainly on reducing UV exposure and protecting the skin. Key prevention measures include:
- Seeking shade during peak sunlight hours7 .
- Wearing protective clothing such as long sleeves and wide-brimmed hats7 .
- Using broad-spectrum sunscreen with an SPF of at least 30 daily2 1.
- Avoiding tanning beds and artificial UV sources1 .
- Regular skin self-examinations to detect new or changing lesions early1 .
Although some MCC cases occur despite preventive efforts, these strategies can lower the risk of developing MCC and other skin cancers7 .
Related Skin Conditions
Patients with Merkel cell carcinoma have an increased risk of developing other skin cancers, including basal cell carcinoma, squamous cell carcinoma, and melanoma5 . MCC can also be confused with benign skin lesions such as cysts, insect bites, or pimples due to its appearance8 . Awareness of these related conditions is important for accurate diagnosis and ongoing skin health monitoring.
Living With Merkel Cell Carcinoma
Living with MCC requires careful long-term follow-up due to the risk of recurrence and development of additional skin cancers5 . Patients often need regular skin exams and monitoring for symptoms of metastasis. Multidisciplinary care involving dermatologists, oncologists, and other specialists is essential to manage treatment side effects and maintain quality of life5 .
MCC survivors should remain vigilant for new skin lesions and maintain regular follow-up visits, as they have a higher chance of developing recurrent MCC or other skin cancers5 .
Frequently Asked Questions
Can Merkel cell carcinoma be cured?
Early-stage MCC can often be cured with surgery and radiation therapy. About 70% of patients survive five years after diagnosis, but prognosis worsens with advanced disease5 .
How is MCC different from other skin cancers?
MCC is rarer and more aggressive than basal or squamous cell carcinoma. It grows rapidly and has a high risk of early metastasis5 3.
What are the signs to watch for?
Look for a painless, fast-growing, firm bump that is red, purple, or skin-colored, especially on sun-exposed areas like the head and neck6 2.
Is immunotherapy effective for MCC?
Immunotherapy targeting PD-1/PD-L1 has improved outcomes in metastatic MCC, but not all patients respond durably10 .