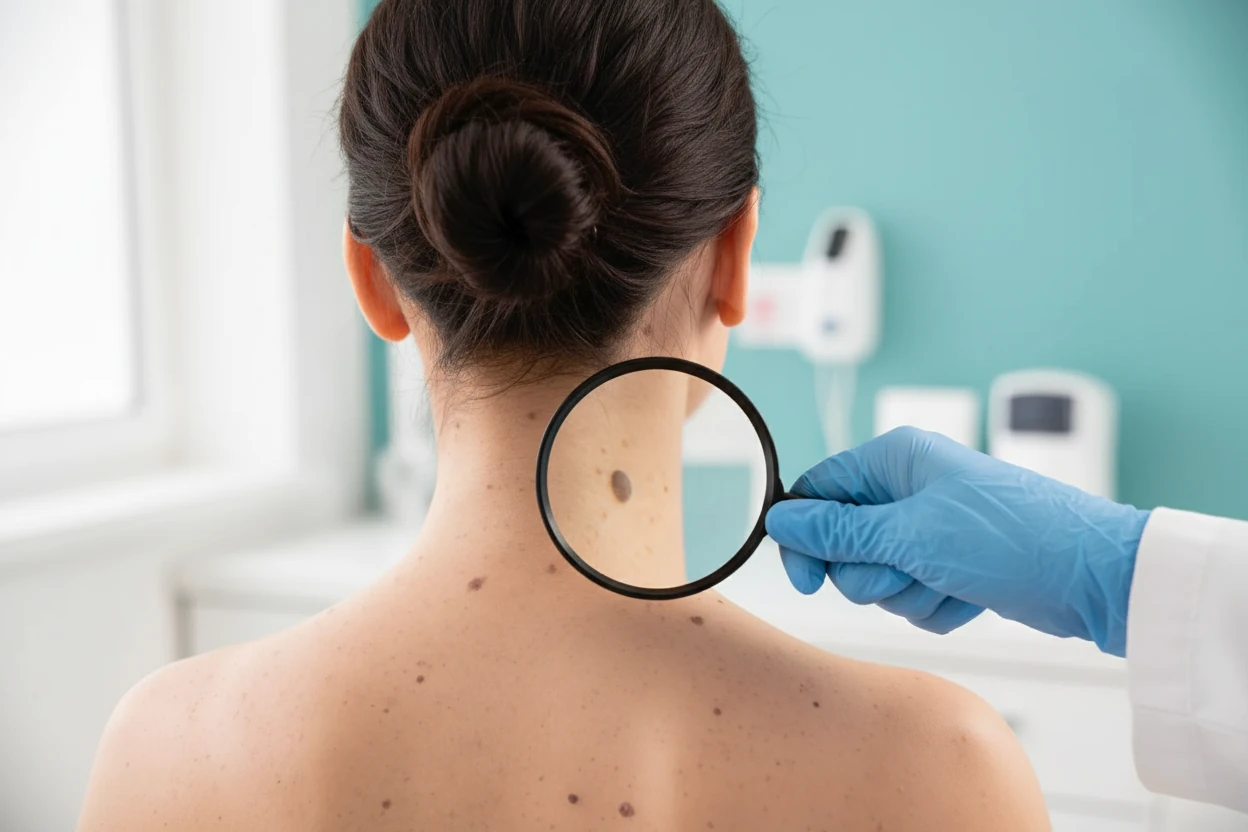
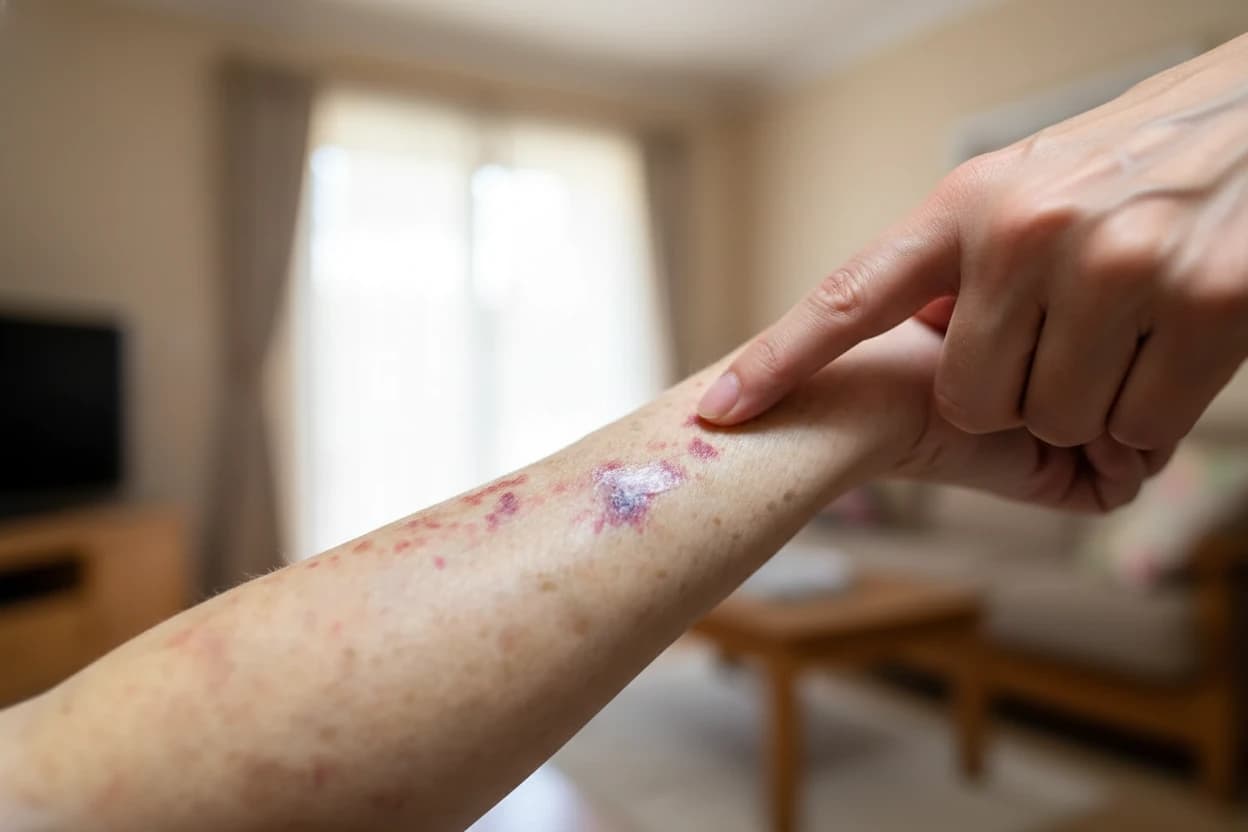
Melanoma is the most aggressive form of skin cancer, known for its rapid growth and potential to spread to other parts of the body. Its incidence has been rising globally, particularly in regions with high ultraviolet (UV) exposure, such as Australia and New Zealand1 2. Early detection is crucial because melanoma caught in its initial stages is often curable with surgery, while advanced melanoma requires more complex treatments3 4.
Identifying Cancerous Moles
Cancerous moles, or melanomas, originate from melanocytes, the pigment-producing cells of the skin responsible for melanin, which gives skin its color5 1. Unlike typical moles, which are usually uniform in color and shape, cancerous moles often exhibit irregular features. Most melanomas develop on sun-exposed areas such as the arms, back, face, and legs, but they can also appear in less exposed or hidden areas like the soles of the feet, palms, under nails, and even inside the body including the eyes and mucous membranes5 6.
Typical moles are generally:
- Uniformly colored (brown, tan, or black) 57
- Round or oval in shape5 7
- Flat or slightly raised5 7
- Usually smaller than 6 millimeters in diameter5 7
- Stable in appearance over many years5 7
Cancerous moles may show one or more of the following characteristics:
- Asymmetry: One half does not match the other half5 7
- Irregular, notched, or blurred borders5 7
- Multiple colors or uneven color distribution, including shades of brown, black, red, white, or blue5 7
- Diameter larger than 6 millimeters, though melanomas can be smaller5 7
- Evolution: Changes in size, shape, color, or elevation over time5 7
- Additional signs such as itching, bleeding, oozing, or tenderness5 7
Because some melanomas do not fit the classic ABCDE pattern, any new, changing, or unusual spot should be evaluated by a healthcare professional8 7. This is especially important for people with darker skin, as melanomas in these individuals often appear in hidden areas like palms, soles, and under nails5 8.
Melanoma Causes and Risk Factors
Melanoma arises from malignant transformation of melanocytes, driven by complex interactions between genetic, environmental, and epigenetic factors1 910. The primary modifiable cause is exposure to ultraviolet (UV) radiation from sunlight and artificial sources like tanning beds11 12. UV radiation damages the DNA in skin cells, leading to mutations that disrupt normal cell growth and death11 12.
Key risk factors for melanoma include:
- Ultraviolet (UV) exposure: Both UVA and UVB rays cause DNA damage in melanocytes, increasing melanoma risk11 12
- Genetic predisposition: Mutations in genes such as CDKN2A, BRAF, NRAS, and MC1R increase susceptibility10 12
- High number of moles: Having more than 50 typical moles or dysplastic (atypical) nevi raises risk13 12
- Fair skin phenotype: Light skin, freckles, red or blonde hair, and light-colored eyes are associated with higher melanoma risk13 12
- History of sunburns: Especially blistering sunburns during childhood13 12
- Family history: A first-degree relative with melanoma increases individual risk13 12
- Living near the equator or at high elevation: Greater UV exposure in these locations12
- Weakened immune system: Conditions or medications that suppress immunity can elevate risk13 12
Inherited gene mutations, though less common, can significantly increase melanoma risk. Familial melanomas often involve mutations in tumor suppressor genes like CDKN2A, CDK4, or BAP110 12. Some rare conditions, such as xeroderma pigmentosum, impair DNA repair and heighten melanoma susceptibility12 .
Melanoma has the highest mutational burden of any cancer, partially attributed to UV-induced DNA damage3 .
Melanoma Warning Signs
The earliest sign of melanoma is often a new mole or a change in an existing mole's size, shape, or color7 5. The American Academy of Dermatology promotes the ABCDE rule to help recognize suspicious moles:
- A - Asymmetry: One half of the mole differs from the other5 7
- B - Border: Edges are irregular, scalloped, or poorly defined5 7
- C - Color: Uneven shades or multiple colors within the mole5 7
- D - Diameter: Larger than 6 millimeters (about the size of a pencil eraser) 57
- E - Evolving: Changes in size, shape, color, or symptoms such as itching or bleeding5 7
Other warning signs include:
- A sore that does not heal7
- Spread of pigment beyond the mole's border into surrounding skin7
- Redness or swelling beyond the mole7
- Itchiness, tenderness, or pain in the area7
- Scaliness, oozing, or bleeding from the mole7
Melanomas can also develop in hidden areas such as under nails (acral lentiginous melanoma), on palms or soles, in the eye (ocular melanoma), or mucous membranes lining the mouth, nose, anus, or genitals5 6. These hidden melanomas may present as dark streaks, irregular patches, or unexplained spots and require medical evaluation.
The first melanoma signs and symptoms often are a change in an existing mole or the development of a new pigmented or unusual-looking growth on the skin5 .
Diagnosis of Atypical Moles and Melanoma
Early detection of melanoma greatly improves treatment outcomes, as localized melanoma is often curable by surgical removal3 14. Diagnosis begins with a thorough skin examination by a healthcare professional, who inspects the skin from head to toe for suspicious moles or lesions15 .
Diagnostic methods include:
Descriptions of vertical growth, bleeding, oozing, and itch were features of thicker melanomas irrespective of pathological type19 .
- Visual examination: Assessment of moles using the ABCDE criteria and clinical judgment8 15
- Dermoscopy: Use of a magnifying tool with light to examine skin lesions more closely8 15
- Monitoring: Photographing and measuring moles over time to detect changes8
- Biopsy: Surgical removal of the mole or lesion for microscopic examination, which is the gold standard for diagnosis8 15
If melanoma is confirmed, further tests may be performed to determine the stage and extent of spread. Sentinel lymph node biopsy is often used for melanomas thicker than 0.8 mm or with ulceration to check for lymph node involvement16 17. Imaging studies such as CT, MRI, or PET scans may be used in advanced cases to detect metastases17 .
Delayed presentation is common, often due to lack of awareness or failure to recognize early signs18 19. Public health campaigns emphasize the importance of regular skin self-examination and prompt medical evaluation of changing lesions20 .
“I recommend making a dermatology appointment as soon as you see a worrying new or changing spot.”
— Mika Tabata8
Melanoma Treatment Options
Treatment depends on the stage and molecular characteristics of the melanoma. Early-stage melanoma is often curable with surgery, while advanced disease requires systemic therapies.
Surgery
Surgical excision is the primary treatment for localized melanoma. The procedure involves removing the melanoma along with a margin of healthy skin to ensure complete removal3 17. This is usually done under local anesthesia in an outpatient setting15 . For melanomas that have spread to nearby lymph nodes, lymphadenectomy (removal of lymph nodes) may be necessary17 . Surgery can also be used to remove metastatic tumors in some cases17 .
Therapies
For advanced or metastatic melanoma, systemic therapies have transformed outcomes:
- Immunotherapy: Drugs that stimulate the immune system to attack melanoma cells, such as anti-PD-1 and anti-CTLA-4 monoclonal antibodies (e.g., nivolumab and ipilimumab) 421
- Targeted therapy: Drugs targeting specific gene mutations in melanoma cells, such as BRAF and MEK inhibitors, used in patients with BRAF mutations22 12
- Radiation therapy: High-energy rays to shrink tumors and control symptoms17
- Emerging treatments: Research is ongoing into neoantigen vaccines and adoptive cell transfer to overcome resistance23 24
Despite advances, resistance to therapy remains a challenge, and five-year survival for metastatic melanoma is still low, underscoring the importance of early detection14 4.
The combination of the anti-PD-1 directed monoclonal antibodies nivolumab and ipilimumab has shown remarkable clinical responses4 .
Skin Cancer Prevention Strategies
Preventing melanoma focuses primarily on reducing UV exposure, the main modifiable risk factor11 13. Effective prevention measures include:
- Avoiding tanning beds and lamps, which emit carcinogenic UV radiation12 13
- Limiting sun exposure, especially during peak hours between 10 a.m. and 4 p.m. 1213
- Wearing protective clothing such as wide-brimmed hats, long sleeves, and UV-blocking sunglasses12 13
- Applying broad-spectrum sunscreen with SPF 30 or higher year-round, reapplying every two hours or after swimming or sweating12 13
- Regular skin self-examination and professional skin checks, especially for high-risk individuals with many moles or family history of melanoma13 20
Population-wide screening programs and public health campaigns have contributed to a reduction in thin melanoma incidence among young people, demonstrating the effectiveness of primary prevention25 13.
Regular use of sunscreen and protective clothing can significantly reduce the risk of melanoma by limiting UV-induced DNA damage in skin cells13 .
Key Takeaways
- Melanoma is a dangerous skin cancer originating from pigment-producing melanocytes and is highly curable if detected early1 3.
- The main cause of melanoma is UV radiation from sunlight and tanning devices, which damages DNA and leads to mutations11 12.
- The ABCDE rule helps identify suspicious moles: Asymmetry, Border irregularity, Color variation, Diameter >6 mm, and Evolution5 7.
- Diagnosis relies on clinical examination, dermoscopy, and biopsy, with sentinel lymph node biopsy used for staging thicker melanomas8 16.
- Treatment includes surgical excision for early disease and immunotherapy or targeted therapy for advanced melanoma3 4.
- Prevention strategies focus on sun protection, avoiding tanning beds, and regular skin checks to catch melanoma early13 25.