Breast cancer screening through mammography is a critical tool in early cancer detection, with AI technology increasingly integrated to enhance accuracy and efficiency. Studies show that AI-assisted mammograms can improve cancer detection rates by up to 20%, particularly benefiting women with dense breast tissue where traditional mammography struggles1 2. However, the cost-effectiveness and clinical impact of AI remain under evaluation, with ongoing research addressing its real-world utility and ethical considerations3 1.
How AI Reads Mammograms
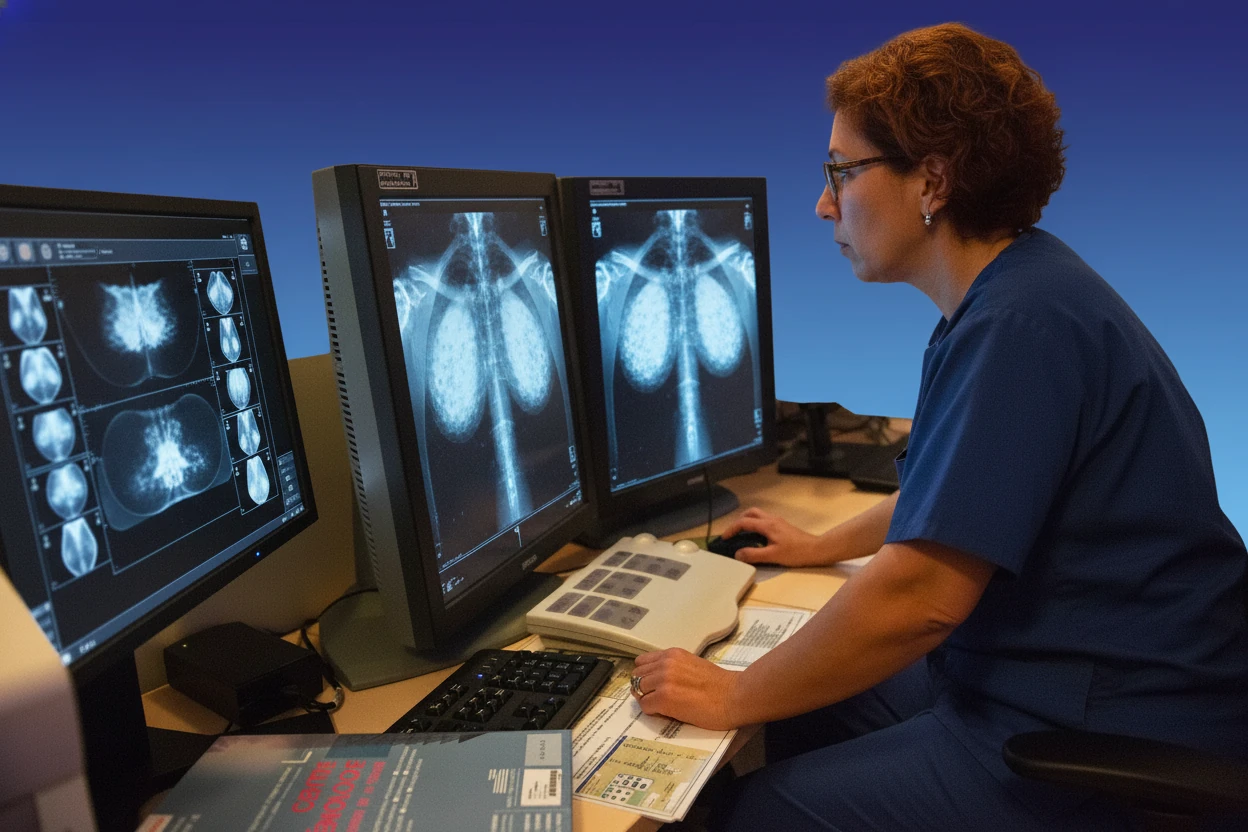
Mammography remains the primary imaging method for breast cancer screening, producing high-resolution grayscale images that reveal variations in breast tissue density essential for detecting malignancies4 . Experienced radiologists identify suspicious patterns in these images through trained visual recognition5 . AI algorithms, especially those based on deep learning, analyze mammograms by detecting subtle imaging features that may be missed by human readers6 7.
AI systems function as decision support tools by rapidly scanning mammographic patterns and highlighting suspicious regions for radiologist review, effectively serving as a second reader or triage mechanism6 74. This approach can improve detection rates and streamline workflow by prioritizing cases that require closer attention4 . The AI analyzes multiple views of the breast, including craniocaudal and mediolateral oblique images, to assess the likelihood of malignancy2 .
Key mechanisms of AI mammogram reading include:
- Detecting subtle variations in tissue density and texture indicative of cancer4 .
- Highlighting suspicious areas on mammograms to assist radiologists in decision-making6 7.
- Serving as a triage tool to prioritize mammograms for detailed human review4 .
- Reducing subjectivity and variability in interpretation by standardizing image analysis5 .
This combination of human expertise and AI analysis aims to enhance the accuracy of breast cancer detection while maintaining the radiologist's critical role in diagnosis6 74.
AI Mammogram Accuracy and Benefits
Artificial intelligence has demonstrated high diagnostic accuracy in mammography, often matching or surpassing the performance of human radiologists1 8. Large-scale studies report that AI assistance can increase cancer detection rates by approximately 20%, identifying more cancers per 1,000 screened women than radiologists alone9 1011. This improvement is particularly notable in women with dense breast tissue, where conventional mammography sensitivity is reduced due to tissue masking1 12.
Additional benefits of AI-assisted mammography include:
“The nice thing about AI is that it doesn’t get tired. It’s not going to replace the job or the expertise of radiologists, but I think it’s only going to enhance our ability to detect more and more breast cancers.”
— Dr. Lisa Abramson, Associate Professor of Radiology, Mount Sinai20
- Lower recall rates and fewer unnecessary follow-up procedures, reducing patient anxiety and healthcare costs10 13.
- Significant reductions in radiologist reading time, ranging from 17% to 91%, by triaging normal mammograms and prioritizing suspicious cases1 .
- Enhanced detection of interval cancers that were missed in prior screenings, potentially leading to earlier diagnosis and treatment2 .
- Support for radiologists with varying levels of experience, improving overall diagnostic consistency and accuracy14 1.
- Potential to alleviate radiologist workload and address shortages, especially in underserved regions lacking specialized breast imaging experts6 13.
Prospective studies such as the MASAI trial and the PRAIM study have confirmed that AI-supported double reading improves cancer detection without increasing recall rates, indicating that AI integration can enhance screening program metrics2 1. AI's ability to flag subtle abnormalities invisible to the human eye contributes to these gains, particularly in complex cases6 7.
However, limitations remain. AI performance depends heavily on the quality and diversity of the training datasets, and biases in these data can lead to unequal diagnostic accuracy across demographic groups15 1617. Furthermore, the long-term impact of AI-assisted screening on clinical outcomes such as mortality reduction is still under investigation18 19.
“It’s incredibly subjective when a human reads a mammogram. Maybe it’s going to reduce the disparities in how these things are read.”
— Dr. Otis Brawley, Johns Hopkins University20
| Benefit | Description | Reference |
|---|---|---|
| Increased Cancer Detection Rate | AI improves detection by about 20%, especially in dense breast tissue cases | 91 |
| Reduced Recall Rates | AI assistance lowers false positives and unnecessary follow-ups | 1013 |
| Reading Time Reduction | AI triaging can cut radiologist reading time by up to 91% | 1 |
| Consistency Across Readers | Enhances accuracy for less experienced radiologists | 141 |
| Support in Underserved Areas | Provides decision support where breast imaging specialists are scarce | 613 |
Cost of AI Mammogram Analysis
The decision to pay extra for AI-assisted mammogram reading involves weighing individual risk tolerance, financial considerations, and access to expert radiologists16 21. AI mammogram analysis is often offered as an optional add-on, with out-of-pocket costs typically ranging from $40 to $50 per screening, as insurance coverage and billing codes for AI interpretation are not yet established21 3.
“I don’t love all this AI stuff, but I definitely love this for me or anyone else in my position. No matter how it was found, I’m glad it was found.”
— Deirdre Hall, patient who paid $50 for AI mammogram analysis20
Radiology practices vary in how they handle AI-related charges. Some large academic centers, such as Massachusetts General Hospital, provide AI analysis at no additional cost to patients, aiming to promote equity and avoid financial barriers21 3. In contrast, some commercial imaging networks charge patients directly, which may limit access for lower-income populations21 .
Key considerations regarding AI mammogram costs include:
- AI analysis is generally a supplementary tool, not a replacement for expert radiologist interpretation4 16.
- The lack of insurance billing codes for AI mammography means patients often pay out of pocket21 3.
- Some patients may find reassurance in AI-assisted readings, potentially reducing anxiety related to mammogram results21 .
- Ethical concerns exist about equitable access if AI is only available to those who can afford extra fees21 .
-
Large trials are underway to establish the clinical and economic value of AI in mammography, which may influence future coverage decisions21 2.
-
Individual breast cancer risk and personal preference for additional screening accuracy16 .
- Availability and expertise of radiologists at the screening center6 4.
- Regional differences in healthcare infrastructure and access to breast imaging specialists13 .
- Ongoing research outcomes that may lead to insurance reimbursement for AI services21 .
- Potential reduction in downstream costs due to fewer false positives and unnecessary procedures10 .