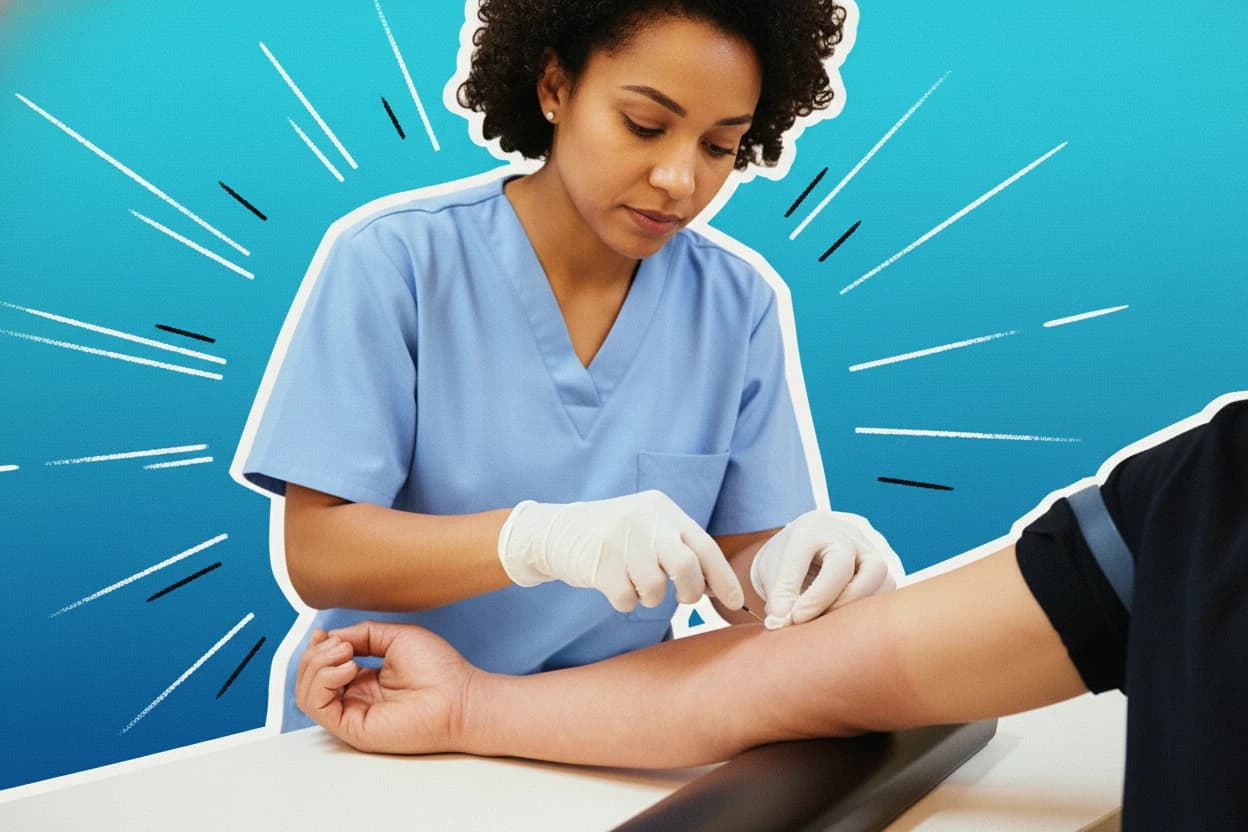
Raynaud's disease affects many people worldwide, causing some areas of the body, especially fingers and toes, to feel numb and cold in response to cold temperatures or stress1 . This condition results from spasms in small blood vessels that limit blood flow, leading to noticeable color changes and discomfort2 . While often mild, Raynaud's can significantly impact quality of life, particularly when linked to other health conditions3 .
Types of Raynaud's Disease
Raynaud's disease, also known as Raynaud's phenomenon, is characterized by episodic excessive narrowing (vasoconstriction) of blood vessels in the fingers and toes, typically triggered by cold or emotional stress4 . It occurs in two main forms: primary and secondary.
Primary Raynaud's Disease
Primary Raynaud's disease, also called idiopathic Raynaud's phenomenon, occurs without any underlying medical condition5 . It is the most common form and usually affects younger individuals, especially women under 30 years of age6 . The exact cause is unknown, but genetic and hormonal factors likely contribute4 . Primary Raynaud's is generally milder and does not lead to tissue damage7 .
- It typically begins in teenage years or early adulthood2 .
- There is often a family history, indicating genetic predisposition8 .
- Symptoms are usually reversible and transient, with no lasting harm9 .
- Women are more commonly affected than men10 .
- It is more prevalent in people living in colder climates1 .
Secondary Raynaud's Disease
Secondary Raynaud's disease occurs in association with other medical conditions, especially those affecting blood vessels, such as connective tissue diseases like scleroderma and lupus5 . It tends to be more severe and can lead to persistent digital ischemia, ulcers, and even gangrene9 .
- Common underlying causes include autoimmune diseases such as systemic sclerosis, lupus, and rheumatoid arthritis4 .
- It may also result from exposure to certain medications, including beta blockers and ergotamine11 .
- Occupational factors like using vibrating tools can precipitate symptoms11 .
- Secondary Raynaud's often develops later in life, typically between ages 35 and 4012 .
- Patients may experience persistent symptoms and complications requiring specialized care13 .
Raynaud's phenomenon can present as a primary symptom without underlying disease or secondary to various medical conditions or therapies, with the majority of individuals having the primary form14 9.
Symptoms of Raynaud's
Raynaud's disease manifests as episodes of vasospasm that reduce blood flow to the extremities, primarily fingers and toes, often triggered by cold or emotional stress15 . These episodes cause characteristic color changes and sensory symptoms.
- The classic triphasic color change includes:
- White (pallor) due to ischemia and reduced blood flow13 .
- Blue (cyanosis) from de-oxygenation of blood4 .
- Red (rubor) as blood flow returns during reperfusion15 .
- Affected areas may feel cold, numb, or painful during attacks16 .
- Paresthesias such as tingling or pins and needles are common13 .
- Episodes are usually transient, lasting from minutes to a few hours17 .
- In secondary Raynaud's, symptoms can be more severe and persistent, sometimes leading to ulcers or gangrene9 .
- Other areas such as the nose, lips, ears, and nipples can also be affected1 .
Raynaud's syndrome causes spasms in small blood vessels in fingers and toes, limiting blood flow and leading to symptoms like skin color changes, cold skin, and a pins and needles sensation. Common triggers include cold weather and stress2 .
Causes and Risk Factors
Raynaud's phenomenon results from an exaggerated vasoconstrictive response of peripheral blood vessels to cold or emotional stress4 . This vasospasm limits blood flow, causing the characteristic symptoms.
- Vasoconstriction is a normal reflex to conserve body heat but is exaggerated in Raynaud's18 .
- Genetic and hormonal factors play a role, especially in primary Raynaud's4 .
- The condition reflects an abnormal response of the blood vessels to stimuli like cold and stress19 .
- Secondary Raynaud's is linked to diseases affecting blood vessels and connective tissues4 .
- Certain medications and occupational exposures can trigger or worsen symptoms11 .
Risk Factors
- Female sex, especially women under 30, is a strong risk factor for primary Raynaud's6 .
- Family history increases the likelihood of developing the condition8 .
- Living in colder climates is associated with higher prevalence1 .
- Autoimmune and connective tissue diseases increase risk for secondary Raynaud's4 .
- Use of medications such as beta blockers, ergotamine, and some chemotherapeutic agents can provoke symptoms11 .
- Occupational exposure to vibrating tools or repetitive trauma may contribute11 .
Raynaud's disease causes some areas of the body such as fingers and toes to feel numb and cold in response to cold temperatures or stress due to vasospasm of small blood vessels1 .
Diagnosing Raynaud's Disease
Diagnosis of Raynaud's disease is primarily clinical, relying on patient history and physical examination4 . There is no single definitive test, but several investigations help differentiate primary from secondary forms.
- Detailed history includes symptom description, triggers, and family history20 .
- Physical exam focuses on color changes and signs of tissue damage4 .
- Nailfold capillaroscopy is the gold standard to distinguish primary from secondary Raynaud's by examining capillaries at the nailfold under magnification19 21.
- Blood tests, including antinuclear antibody (ANA) testing, help detect autoimmune diseases causing secondary Raynaud's4 21.
- Additional tests may rule out other vascular or systemic conditions20 .
| Diagnostic Tool | Purpose | Notes |
|---|---|---|
| Nailfold Capillaroscopy | Examines capillary abnormalities | Differentiates primary vs secondary19 21 |
| ANA Blood Test | Detects autoimmune antibodies | Positive in connective tissue diseases4 21 |
| Physical Examination | Observes color changes and tissue health | Essential for initial diagnosis4 20 |
| Medical History | Identifies triggers and family history | Guides diagnosis and management20 |
Raynaud's can inhibit lifestyle and leisure pursuits, hinder the ability to perform various jobs, and affect quality of life3 .
Diagnosis of Raynaud’s phenomenon is primarily clinical, based on history and physical examination4 .
Treatment Options
Treatment of Raynaud's disease aims to reduce the frequency and severity of attacks, relieve symptoms, and prevent complications such as ulcers and tissue damage9 . Management depends on whether the condition is primary or secondary.
- Avoidance of cold exposure and emotional stress is fundamental17 .
- Lifestyle changes include wearing warm clothing and protecting extremities11 .
- Pharmacologic treatments for more severe cases include calcium channel blockers and vasodilators22 .
- Intravenous prostaglandins may be used in severe ischemic attacks22 .
- Surgical options like sympathectomy are reserved for treatment-resistant cases23 .
- Severe cases with tissue damage may require hospitalization or surgical intervention16 .
Referral to a rheumatologist is recommended for evaluation and management, especially in secondary Raynaud's where underlying diseases require treatment24 25.
Prevention Strategies
Preventing Raynaud's attacks involves minimizing exposure to known triggers and adopting healthy lifestyle habits.
- Avoid cold environments and sudden temperature changes17 .
- Manage stress through relaxation techniques such as mindfulness or yoga17 .
- Stop smoking, as nicotine causes vasoconstriction and worsens symptoms11 17.
- Review medications with healthcare providers to avoid those that exacerbate symptoms, such as beta blockers and ergotamines11 .
- Regular exercise improves circulation but should be done cautiously in cold weather26 .
| Prevention Tips | Description |
|---|---|
| Keep Warm | Wear gloves, warm socks, and layered clothing11 17 |
| Stress Management | Use relaxation techniques to reduce attacks11 17 |
| Smoking Cessation | Avoid nicotine to prevent vasospasm11 17 |
| Medication Review | Discuss alternatives to exacerbating drugs11 |
| Avoid Rapid Temperature Changes | Prevent sudden vasospastic episodes17 |
Associated Conditions
Raynaud's disease is often linked to other vascular and autoimmune disorders, especially in its secondary form.
- Connective tissue diseases such as systemic sclerosis, lupus, rheumatoid arthritis, and Sjögren syndrome are common causes of secondary Raynaud's4 912.
- Peripheral arterial diseases like atherosclerosis can worsen symptoms16 .
- Thromboangiitis obliterans (Buerger disease) causes vascular inflammation that exacerbates ischemia16 .
- Carpal tunnel syndrome may co-occur and cause similar symptoms due to nerve compression15 .
- Secondary Raynaud's involves complex vascular and immune mechanisms4 .
Raynaud’s phenomenon is a painful vascular condition in which abnormal vasoconstriction of the digital arteries causes blanching of the skin14 .
Managing Daily Life
Living with Raynaud's disease requires practical strategies to reduce symptoms and maintain quality of life.
- Patients should avoid cold exposure by dressing warmly and using hand warmers17 .
- Stress reduction techniques can decrease attack frequency17 .
- Smoking cessation is critical to improve circulation11 .
- Regular follow-up with healthcare providers helps monitor disease progression and prevent complications24 .
- Educating family and coworkers about the condition can improve support and understanding17 .