Postural Orthostatic Tachycardia Syndrome (POTS) affects about 0.2% of the population, mainly women aged 15 to 50 years1 . It is a chronic disorder characterized by an excessive increase in heart rate upon standing, leading to symptoms like lightheadedness, palpitations, and fatigue2 . Although the exact cause of POTS is complex and varies among patients, treatment focuses on improving symptoms and quality of life through a combination of lifestyle changes and medications3 . Many patients experience symptom improvement over time with appropriate management, although the condition rarely resolves completely4 .
Treatment Approaches
Managing POTS requires a comprehensive approach that combines non-pharmacological strategies with pharmacologic therapies when necessary5 . The syndrome involves multiple mechanisms, including cardiovascular deconditioning, blood volume depletion, and autonomic nervous system dysfunction, which contribute to symptoms and functional disability6 7. Early initiation of physical reconditioning and volume expansion is recommended to counteract these effects8 6.
Exercise training is a cornerstone of treatment and is recommended as a complementary therapy according to international guidelines8 . Because cardiovascular deconditioning plays a significant role in POTS, improving physical conditioning helps reduce symptoms and improve function6 . Pharmacologic treatments are generally reserved for patients with severe or refractory symptoms and aim to support lifestyle interventions by controlling heart rate and blood pressure9 10.
Multidisciplinary care involving patient education, symptom management, and psychosocial support is essential for optimal outcomes11 12. Treatment plans should be individualized based on symptom severity, subtype of POTS, and patient response13 .
“While POTS has been around for decades, it's largely been ignored by our medical system. Historically, the response has been to dismiss these symptoms as being due to women's 'anxiety' and to them being 'overwhelmed.'”
— Brit Adler, Johns Hopkins POTS Program14
Lifestyle Modifications
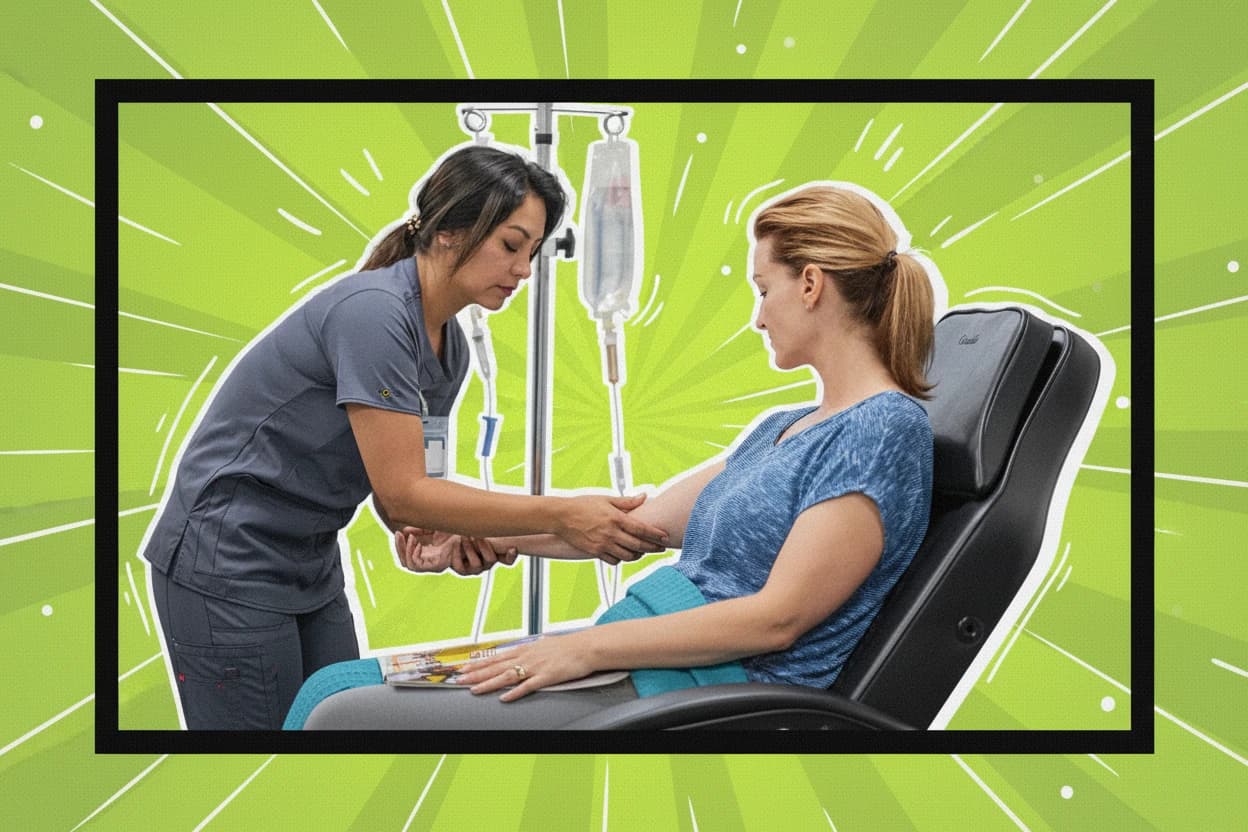
Lifestyle changes form the foundation of POTS management and focus on improving blood volume, reducing venous pooling, and enhancing orthostatic tolerance5 12. Patients are encouraged to increase fluid intake to about 2 to 3 liters daily and to consume more salt to expand blood volume and improve circulation6 3.
Exercise rehabilitation programs begin with adaptive approaches, such as graded exercise starting in a semi-recumbent or horizontal position, to minimize orthostatic stress11 6. Horizontal exercises like rowing, swimming, and recumbent biking are preferred initially before progressing to upright activities6 14. This gradual reconditioning helps improve cardiovascular function and reduces symptom severity7 .
POTS symptoms often worsen with heat, dehydration, and prolonged standing, making lifestyle adaptations crucial for symptom control and improved quality of life. 1213
Compression garments, including waist-high compression stockings with 30 mm Hg pressure and abdominal binders, are used to reduce venous pooling in the legs and abdomen, which can alleviate symptoms12 13. Physical counter-maneuvers such as leg crossing and calf muscle tensing during standing can also help reduce orthostatic intolerance12 .
Additional lifestyle strategies include:
- Avoiding prolonged standing and hot environments that exacerbate symptoms13 .
- Using mobility aids like walkers with seats to prevent falls and manage fatigue12 .
- Employing energy conservation techniques and pacing activities to manage daily fatigue12 .
- Eating smaller, more frequent meals to prevent postprandial symptom worsening12 .
- Elevating the head of the bed slightly to condition the body to orthostatic stress13 .
“In general, since most patients with POTS have trouble with fluid distribution, we typically start exercises either lying down or sitting in a supported position. We're trying to take gravity out of the equation.”
— Fin Mears, Johns Hopkins POTS Program14
Prescription Medications
Pharmacologic therapy is considered when non-pharmacological measures are insufficient to control symptoms or in cases of severe POTS9 10. Medications aim to improve blood volume, stabilize blood pressure, and control heart rate to facilitate participation in exercise and daily activities9 5.
Blood Volume and Blood Pressure Medications
Volume expanders and vasoconstrictors are commonly used off-label to increase blood volume and vascular tone9 10. Fludrocortisone, a mineralocorticoid, promotes sodium retention and plasma volume expansion, helping to improve orthostatic tolerance3 . Midodrine, an alpha-1 adrenergic agonist, causes vasoconstriction, which reduces venous pooling and increases venous return to the heart9 10.
Although midodrine is FDA-approved for orthostatic hypotension, it is frequently prescribed off-label for POTS9 10. Common side effects include supine hypertension, headache, and paresthesia9 10. Salt supplementation is often recommended alongside these medications to maximize blood volume expansion6 .
Heart Rate Medications
Beta-blockers and other heart rate-lowering agents may be used to control excessive tachycardia in POTS patients9 10. These medications help reduce palpitations and improve symptoms related to rapid heart rate9 . However, no medications are specifically approved by the FDA for POTS, and treatment is tailored to individual patient needs and responses9 3.
POTS Prognosis and Outlook
POTS is not associated with increased mortality, and many patients experience symptom improvement or remission over months to years with appropriate management4 5. However, quality of life can be significantly impaired, often comparable to chronic conditions such as heart failure15 . Functional impairment varies widely; some patients are unable to work or attend school, while others maintain daily activities15 .
Symptom severity fluctuates over time, requiring ongoing adjustments in treatment strategies4 5. Younger age at onset is associated with a more favorable prognosis, with over half of patients no longer meeting POTS diagnostic criteria within five years3 . Despite this, many patients continue to experience symptoms such as fatigue, anxiety, and sleep disturbances even with treatment3 .
While POTS rarely resolves spontaneously, most patients benefit from a multimodal treatment approach that improves symptoms and quality of life over time. 34
Daily Management of POTS
- Living with POTS involves practical strategies to manage symptoms and maintain function, with patients benefiting from education about their condition and psychosocial support to cope with the chronic nature of the syndrome12 .
- Mobility aids, workplace or school accommodations, and energy conservation techniques help patients manage daily activities and reduce symptom burden16 12.
- Patients are advised to avoid triggers such as prolonged standing, heat exposure, and dehydration13 .
- Cooling strategies, including cooling vests, can alleviate heat-induced symptom worsening12 .
- Physical counter-maneuvers and pacing activities are useful for managing orthostatic intolerance and fatigue12 .
- Regular follow-up with healthcare providers is important to adjust treatment plans as symptoms change over time4 .
- Patient education remains a cornerstone of management, empowering individuals to participate actively in their care3 .