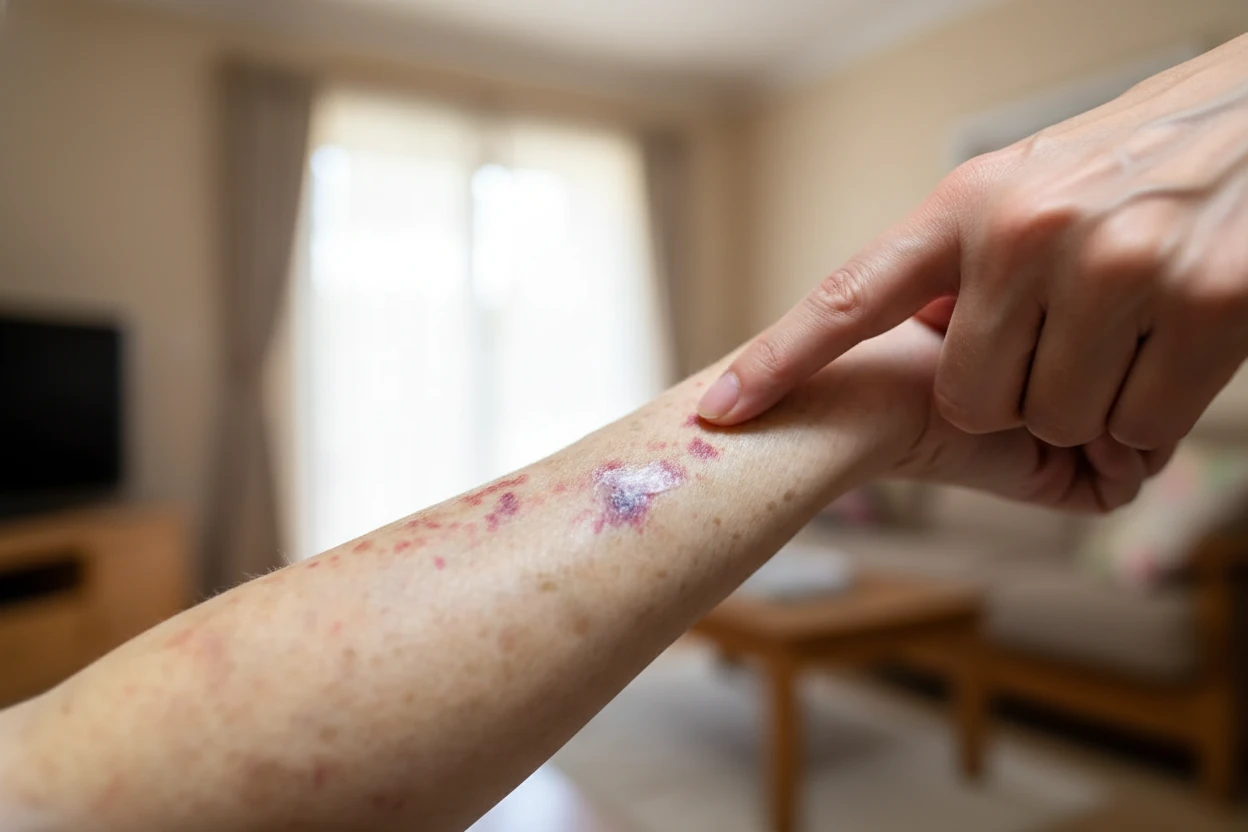
Petechiae are tiny red, purple, or brown spots that appear on the skin or mucous membranes due to bleeding from small blood vessels called capillaries1 . These pinpoint-sized spots are flat, painless, and do not itch, often resembling a rash but differing in key ways2 . While many cases of petechiae are benign and resolve on their own, they can also signal serious underlying health conditions requiring urgent evaluation2 3.
Recognizing Petechiae Symptoms
Petechiae are small, flat, nonpalpable macules that measure less than 2 millimeters in diameter4 . They appear as grouped pinpoint hemorrhages that may mimic a rash but are distinct because they do not blanch (turn white) when pressed4 5. The color of petechiae ranges from red to violaceous or brownish, reflecting blood that has leaked into the skin6 . These spots commonly occur on the arms, legs, stomach, buttocks, and may also be found on mucous membranes such as inside the mouth or on the eyelids7 8.
Importantly, petechiae typically do not cause pain or itching6 . They may appear suddenly and can be isolated or widespread. When petechiae are accompanied by systemic symptoms such as fever, dizziness, syncope (fainting), respiratory difficulty, or neurological changes, urgent medical evaluation is necessary5 . These symptoms may indicate serious infections or hematologic disorders5 .
💡 Did You Know?
Petechiae are pinpoint-sized spots of bleeding under the skin or mucous membranes. The purple, red, or brown dots are not raised or itchy, and they're not a rash9 .
Common Causes of Petechiae
Petechiae are not a disease themselves but a clinical sign indicating underlying conditions3 . They result from capillary hemorrhage, where blood leaks from tiny blood vessels into the skin or mucous membranes3 10. The primary pathophysiological causes include thrombocytopenia (low platelet count), platelet dysfunction, coagulation disorders, and vascular fragility10 .
Risk Factors
- Mechanical trauma or strain: Prolonged straining from coughing, vomiting, childbirth, or heavy lifting can rupture capillaries, especially on the face, neck, and chest11 112.
- Infections: Severe bacterial infections such as meningococcemia and streptococcal infections, as well as viral infections like cytomegalovirus, mononucleosis, and viral hemorrhagic fevers, can cause petechiae3 112.
- Hematologic disorders: Conditions like leukemia, thrombocytopenia, and immune thrombocytopenic purpura lead to reduced platelet counts and bleeding manifestations including petechiae13 14.
- Autoimmune vasculitis: Diseases such as systemic lupus erythematosus (SLE) and IgA vasculitis (Henoch-Schönlein purpura) cause inflammation and damage to blood vessels, resulting in petechiae15 3.
- Nutritional deficiencies: Vitamin C deficiency (scurvy) impairs collagen synthesis, weakening blood vessel walls and causing petechiae16 17.
- Medications: Certain drugs including antibiotics (penicillin), anticonvulsants (phenytoin), NSAIDs, anticoagulants, and sedatives may induce petechiae as a side effect11 18.
- Genetic and connective tissue disorders: Conditions like Wiskott-Aldrich syndrome and Ehlers-Danlos syndrome increase vascular fragility and risk of petechiae19 3.
Many patients will notice a lot of scattered bright red dots on their arms or lower legs that occur with very little or no known trauma. It’s a sign that a person’s platelet count is extremely low14 .
How Petechiae Is Diagnosed
Diagnosis of petechiae begins with clinical observation of non-blanching, pinpoint-sized red or purple spots on the skin or mucous membranes20 . A detailed medical history and physical examination are essential to identify possible causes and associated symptoms5 .
Key diagnostic steps include:
- History taking: Inquiry about recent infections, trauma, drug use, nutritional status, familial bleeding disorders, and symptom onset5 .
- Physical examination: Inspection of lesion characteristics, distribution, and presence of other bleeding signs such as bruising or mucosal bleeding; assessment for hepatosplenomegaly and lymphadenopathy5 .
- Laboratory tests:
- Complete blood count (CBC) to evaluate platelet levels and other blood parameters5 .
- Blood cultures to detect bacteremia in infectious causes3 .
- Antineutrophil cytoplasmic antibody (ANCA) testing for vasculitis-related petechiae21 .
- C-reactive protein (CRP) to assess systemic inflammation5 .
- Urinalysis to check for hematuria or proteinuria indicating systemic involvement5 .
Petechiae result from capillary hemorrhage due to factors like thrombocytopenia, platelet defects, coagulation abnormalities, or vascular fragility3 10. Understanding the circulatory system's microvascular network, especially capillaries connecting arteries and veins, helps explain how these tiny blood vessels can leak blood into the skin22 .
Petechiae Treatment Options
Treatment of petechiae focuses on addressing the underlying cause rather than the spots themselves5 . Many benign cases resolve spontaneously without intervention4 . However, serious causes require targeted therapies.
Management approaches include:
- Infections: Appropriate antimicrobial therapy such as antibiotics or antivirals3 .
- Hematologic disorders: Platelet transfusions for severe thrombocytopenia; chemotherapy and supportive care for hematologic malignancies like leukemia13 .
- Autoimmune vasculitis: Corticosteroids and immunosuppressants to control inflammation15 .
- Nutritional deficiencies: Vitamin C supplementation for scurvy-related petechiae16 .
- Mechanical trauma: Local cold application to reduce capillary bleeding12 .
- Immune thrombocytopenic purpura: Intravenous immunoglobulin (IVIG) therapy may be used13 .
- Persistent pigmented purpuric dermatoses: Laser therapy can be considered6 .
Clinicians emphasize thorough evaluation including history, physical examination, and laboratory investigations to guide treatment decisions5 .
We would recommend people come in and have a complete blood count done so we can quantify their platelet number and determine whether they might benefit from treatments to try to bring that platelet count up14 .
Preventing Petechiae
Prevention of petechiae primarily involves managing the underlying diseases and minimizing factors that cause capillary damage or clotting abnormalities3 . Key preventive strategies include:
- Avoiding alcohol to reduce vascular injury23 .
- Maintaining good hygiene to prevent infections3 .
- Ensuring balanced nutrition and hydration to support vessel integrity and clotting function16 3.
- Avoiding excessive strain or trauma to the skin to prevent capillary rupture12 .
- Smoking cessation to improve vascular health23 .
- Reviewing medications to identify and adjust drugs that may cause petechiae3 .
- Weight management to decrease vascular stress12 .
Close observation is important to detect any progression or complications early5 .
Potential Complications
While petechiae themselves do not cause complications, the underlying causes can lead to serious health issues if untreated3 . Potential complications include:
- Hemorrhage due to severe thrombocytopenia or coagulation disorders19 .
- Sepsis and multi-organ failure in infectious etiologies such as meningococcemia24 .
- Organ damage from systemic autoimmune vasculitis15 .
- Increased risk of thrombotic and ischemic events in vascular diseases associated with petechiae25 .
- Anemia and decreased physical capacity from chronic blood loss or bone marrow failure17 .
Effective prevention and early treatment of the root cause are essential to reduce morbidity and mortality linked to petechiae3 5.
Petechiae Summary
Petechiae are small, flat, non-itchy red or purple spots caused by bleeding from tiny blood vessels under the skin or mucous membranes2 . They serve as a clinical sign of various conditions ranging from benign mechanical causes to life-threatening infections and hematologic disorders3 4. Diagnosis relies on clinical examination and targeted laboratory tests to identify the underlying cause5 . Treatment is cause-specific and may include antibiotics, immunosuppressants, vitamin supplementation, or supportive care3 1315. Prevention focuses on managing underlying diseases, avoiding vascular injury, and maintaining overall health3 16.
Prompt medical evaluation is crucial when petechiae occur with systemic symptoms such as fever, dizziness, or respiratory difficulty to prevent serious complications5 .
Petechiae FAQs
Are petechiae a disease?
No, petechiae are a sign of an underlying condition, not a disease themselves3 .
Can petechiae go away on their own?
Yes, petechiae from benign causes such as mechanical trauma often resolve spontaneously within days to weeks4 12.
When should I see a doctor for petechiae?
Seek medical attention if petechiae appear with systemic symptoms like fever, confusion, difficulty breathing, or if the spots spread rapidly5 2.
What conditions cause petechiae?
Common causes include infections, autoimmune diseases, blood disorders, nutritional deficiencies, medications, and trauma3 11.
Can petechiae indicate leukemia?
Yes, petechiae can be an early sign of leukemia due to low platelet counts from bone marrow failure14 .