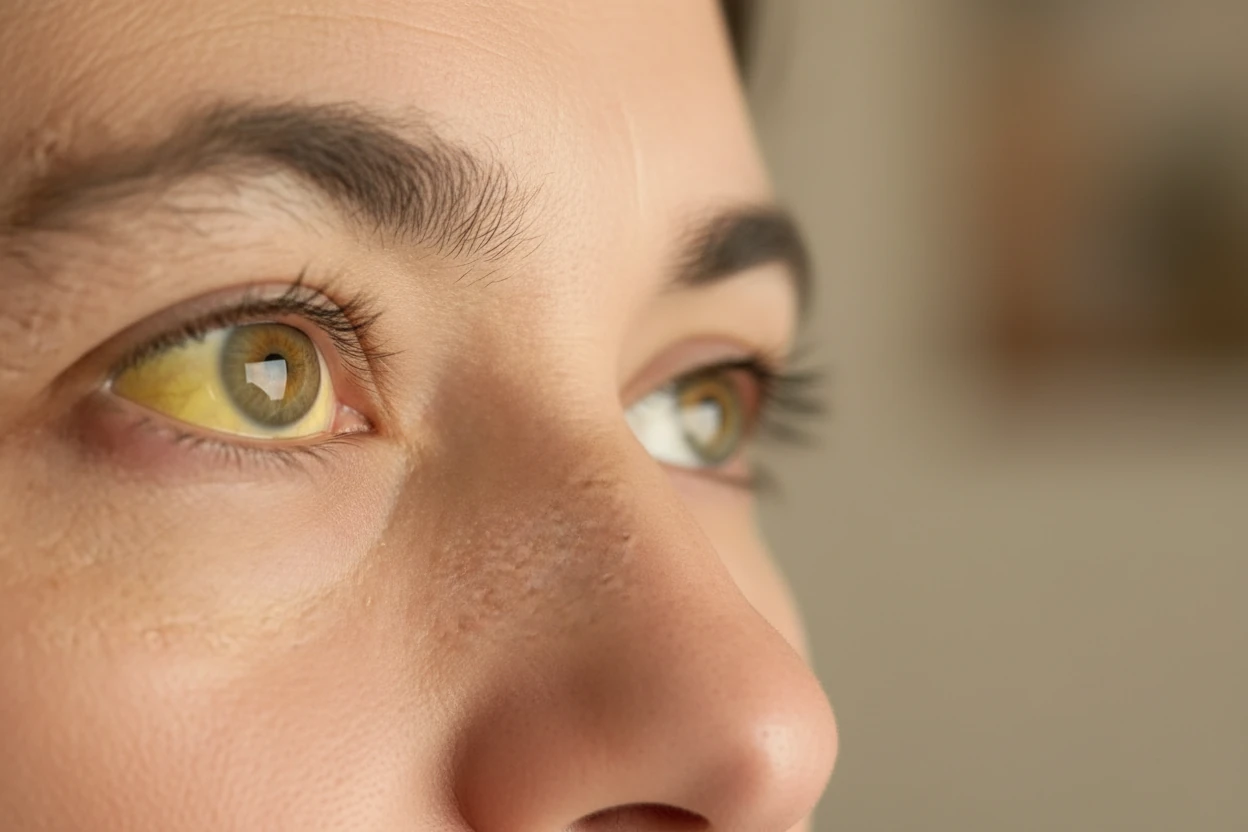
High bilirubin levels, or hyperbilirubinemia, affect hundreds of thousands of newborns worldwide each year and remain a significant cause of preventable disability in low-resource settings1 . Elevated bilirubin can lead to jaundice, a yellowing of the skin and eyes, signaling underlying liver or blood disorders2 . While often benign, especially in newborns, high bilirubin levels require careful monitoring and sometimes treatment to prevent serious complications such as neurological damage3 1.
Normal and Elevated Bilirubin Levels
Bilirubin is a yellow pigment formed from the breakdown of old red blood cells. The liver processes bilirubin, making it water-soluble (conjugated) so it can be excreted in bile and stool. Normal total bilirubin levels in adults and children typically range from 0.2 to 1.3 mg/dL, with levels above this considered elevated2 4. Clinical jaundice usually becomes visible when serum bilirubin exceeds 2.5 to 3 mg/dL5 4.
Levels in Newborns
Newborns commonly experience higher bilirubin levels due to increased red blood cell turnover and immature liver function. Normal total bilirubin in newborns ranges from 1.0 to 12.0 mg/dL4 . Jaundice is very common and usually benign in term and late preterm infants, but critical hyperbilirubinemia is uncommon and can cause long-term neurological impairment if untreated3 . Guidelines recommend monitoring bilirubin levels using nomograms like the Bhutani curve, especially in the first days after birth3 .
| Age of Newborn | Typical Bilirubin Range (mg/dL) 24 |
|---|---|
| 1 day | 1.4 – 8.7 |
| 1–2 days | 3.4 – 11.5 |
| 2–5 days | 1.5 – 12.0 |
| Over 5 days | 0.3 – 1.2 |
| Sources: 24 | |
Early discharge of healthy newborns, particularly those with breastfeeding not fully established, may delay diagnosis of significant hyperbilirubinemia3 .
Causes of High Bilirubin
High bilirubin levels can result from problems occurring before bilirubin reaches the liver (pre-hepatic), within the liver (hepatic), or after the liver (post-hepatic) 65.
- Pre-hepatic causes involve increased bilirubin production, often due to hemolysis (breakdown of red blood cells) 65.
- Hepatic causes include impaired liver uptake, conjugation, or excretion of bilirubin due to liver diseases or genetic conditions6 5.
- Post-hepatic causes involve obstruction of bile flow from the liver to the intestines, such as gallstones or tumors6 5.
Alcohol-Related Liver Disease
Alcohol-related liver disease impairs the liver’s ability to process bilirubin, leading to elevated levels in the blood. Chronic alcohol use can cause liver inflammation and damage, reducing bilirubin clearance7 8.
Cirrhosis
Cirrhosis, the scarring of liver tissue, disrupts normal liver function including bilirubin metabolism. This can cause both conjugated and unconjugated hyperbilirubinemia, often accompanied by other signs of liver failure6 8.
Gallstones
Gallstones can block bile ducts, preventing bilirubin from being excreted into the intestines. This post-hepatic obstruction causes conjugated bilirubin to build up in the blood, leading to jaundice and dark urine6 28.
Gilbert Syndrome
Gilbert syndrome is a common hereditary condition characterized by intermittent mild unconjugated hyperbilirubinemia without liver disease or hemolysis. It results from reduced activity of the enzyme that conjugates bilirubin in the liver9 . Most patients are asymptomatic, and bilirubin levels rarely exceed 5 mg/dL9 .
Hemolytic Anemia
Hemolytic anemia causes excessive breakdown of red blood cells, increasing bilirubin production beyond the liver’s capacity to conjugate and excrete it. This leads to elevated unconjugated bilirubin levels6 2.
Hepatitis
Hepatitis, inflammation of the liver often due to viral infection, impairs bilirubin processing. This hepatic dysfunction can cause both conjugated and unconjugated hyperbilirubinemia, depending on the severity and type of hepatitis6 108.
Symptoms of Hyperbilirubinemia
The hallmark symptom of elevated bilirubin is jaundice, a yellow discoloration of the skin and the whites of the eyes (scleral icterus) 658. Jaundice typically appears when serum bilirubin exceeds 2.5 to 3 mg/dL5 .
Few term newborns with hyperbilirubinemia have serious underlying pathology. Jaundice is considered pathologic if it presents within the first 24 hours after birth, the total serum bilirubin level rises by more than 5 mg per dL (86 µmol per L) per day or is higher than 17 mg per dL (290 µmol per L), or an infant has signs and symptoms suggestive of serious illness14 .
Other symptoms depend on the underlying cause and may include:
- Itchy skin (pruritus) 118
- Dark urine and pale stools (especially in conjugated hyperbilirubinemia) 62
- Fatigue and weakness11
- Abdominal pain or swelling11
- Nausea and vomiting11
Symptoms in Infants
In newborns, hyperbilirubinemia primarily presents as jaundice. Additional signs of severe or progressing hyperbilirubinemia may include:
- Refusal to suck or feed poorly12
- High-pitched crying12
- Vomiting12
- Depressed primitive reflexes12
- Convulsions or stiffness12
If untreated, severe neonatal hyperbilirubinemia can lead to kernicterus, a form of bilirubin-induced brain damage causing permanent neurological impairment3 1.
Jaundice in newborns is common and usually resolves without intervention, but critical hyperbilirubinemia can cause serious brain damage if left untreated1 3.
Diagnosing High Bilirubin
Diagnosis begins with clinical observation of jaundice and confirmation by measuring serum bilirubin levels5 2. Blood tests differentiate between conjugated (direct) and unconjugated (indirect) bilirubin, helping to identify the underlying cause5 2.
Additional tests may include:
- Liver function tests (alkaline phosphatase, aminotransferases) 5
- Complete blood count to assess for hemolysis6
- Imaging studies (ultrasound, CT, MRI) to detect biliary obstruction or liver abnormalities5
- Urine bilirubin test, which is positive only in conjugated hyperbilirubinemia2
Diagnosis in Infants
In neonates, bilirubin levels are monitored closely, especially in the first 48 hours and again at 3–5 days of age3 . The Bhutani nomogram is used to assess risk based on bilirubin levels and age in hours3 .
Early signs of severe hyperbilirubinemia in infants include refusal to suck and depressed reflexes, while later signs may include high-pitched cry, convulsions, and vomiting12 . Prompt evaluation is critical to prevent kernicterus3 .
Phototherapy is the first-line treatment for elevated bilirubin in newborns, converting bilirubin into a water-soluble form for easier excretion13 3. Exchange transfusion is reserved for severe cases unresponsive to phototherapy1 14.
“Phototherapy should be instituted when the total serum bilirubin level is at or above 15 mg per dL (257 µmol per L) in infants 25 to 48 hours old, 18 mg per dL (308 µmol per L) in infants 49 to 72 hours old, and 20 mg per dL (342 µmol per L) in infants older than 72 hours.”
— Meredith L. Porter, American Academy of Family Physicians14
Key Takeaways
- Bilirubin is a yellow pigment formed from red blood cell breakdown and processed by the liver for excretion2 4.
- Normal bilirubin levels vary by age; newborns typically have higher levels than adults4 .
- Elevated bilirubin causes jaundice, which appears when serum levels exceed 2.5 to 3 mg/dL5 4.
- Causes of high bilirubin include increased production (hemolysis), liver dysfunction, and bile duct obstruction6 5.
- In newborns, hyperbilirubinemia is common and usually benign but requires monitoring to prevent neurological damage3 1.
Frequently Asked Questions
Is high bilirubin life-threatening?
High bilirubin itself is usually a sign of an underlying condition. In newborns, very high levels can cause brain damage (kernicterus) if untreated. In adults, it often signals liver or blood disorders that may require treatment3 12.
Who is at higher risk for elevated bilirubin?
Newborns, especially preterm infants, and adults with liver disease or hemolytic anemia are at higher risk for elevated bilirubin levels3 215.
Does high bilirubin always mean liver damage?
Not always. High bilirubin can result from increased red blood cell breakdown or genetic conditions like Gilbert syndrome without liver damage6 29.
How is high bilirubin treated?
Treatment depends on the cause. Newborns often receive phototherapy, while adults may need treatment for liver disease, gallstones, or hemolysis. Severe cases may require blood transfusions or surgery13 12.