Hemorrhage, or bleeding from damaged blood vessels, is a critical medical condition that can range from minor bruises to life-threatening internal bleeding. It is a leading cause of preventable death worldwide, especially in trauma cases, and requires timely recognition and treatment to avoid severe complications1 2. Understanding the types, symptoms, causes, diagnosis, and treatment options is essential for effective management and improved patient outcomes2 .
Types of Hemorrhage
The human circulatory system consists of arteries, veins, and capillaries, each playing distinct roles in blood transport3 . Hemorrhage can originate from any of these vascular beds, and the type of bleeding depends on the vessel involved:
- Arterial hemorrhage involves bleeding from arteries, which carry oxygenated blood away from the heart under high pressure. This bleeding is characterized by pulsatile, bright red blood and is the most dangerous type due to rapid and high-volume blood loss3 .
- Venous hemorrhage occurs from veins, which return deoxygenated blood to the heart. Venous bleeding is marked by a steady flow of dark red blood and is generally less severe than arterial bleeding but still requires prompt care3 .
- Capillary hemorrhage arises from the smallest blood vessels, capillaries, which connect arteries and veins and facilitate nutrient exchange. Capillary bleeding is slow, oozing, and often the least severe, sometimes resolving spontaneously though it can be painful3 .
In clinical observation, capillary hemorrhage appears as red blood welling up like water from a sponge. If an artery ruptures in an extremity, there is no pulsation below the rupture site, whereas venous rupture leads to intense swelling (edema) in the affected area4 . Additionally, blood vessel atony (loss of muscle tone) can cause hemorrhage by congestion, especially in dependent body parts3 .
💡 Did You Know?
A hemorrhage can be internal or external, with examples including hemothorax (blood between lungs and rib cage), intracranial hemorrhage (bleeding inside the brain), postpartum hemorrhage (severe vaginal bleeding after childbirth), and subarachnoid hemorrhage (bleeding between brain and protective tissues) 1.
Recognizing Hemorrhage Symptoms
Symptoms of hemorrhage vary widely depending on the bleeding type, location, and severity. Early recognition is critical to prevent serious outcomes.
External Hemorrhage Symptoms
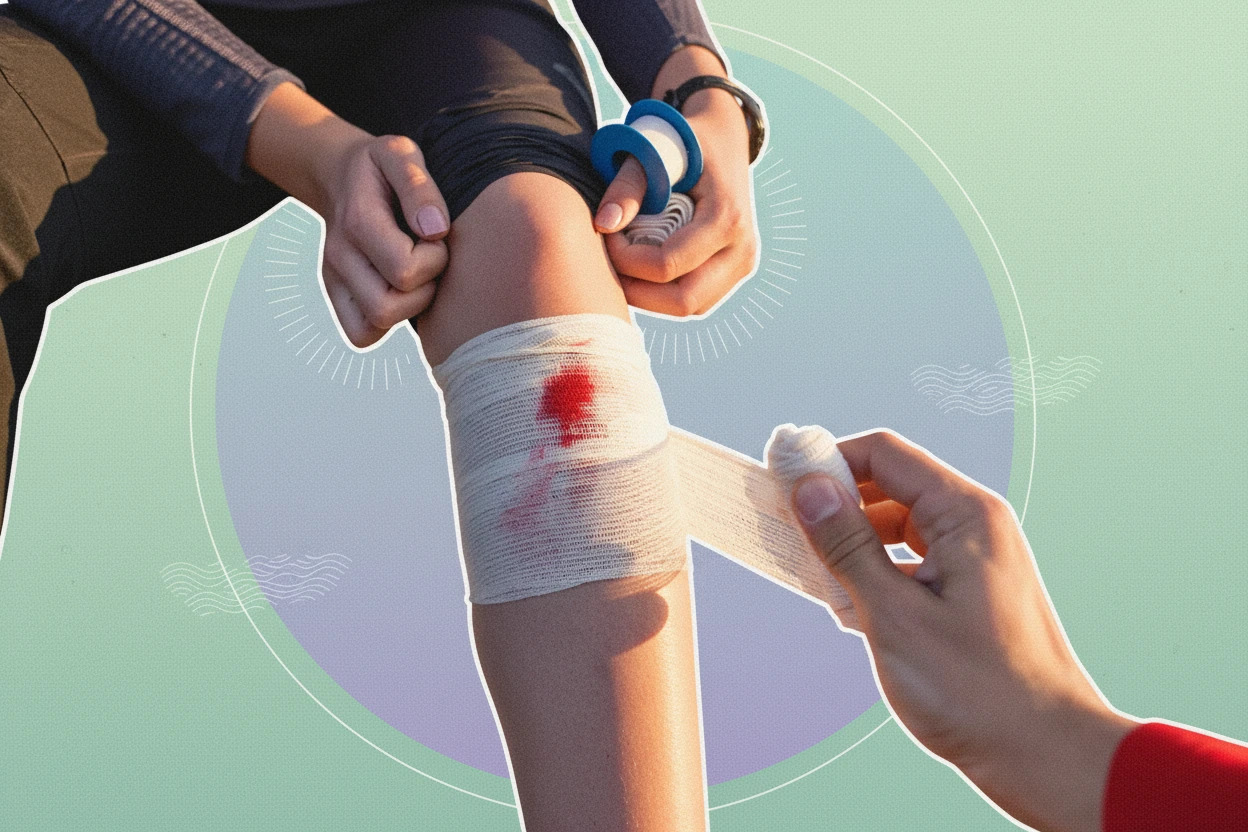
External bleeding is usually visible and easier to identify. It often results from skin breaks such as cuts, lacerations, or puncture wounds3 . Common signs include:
- Visible blood flow from the wound site3
- Bruising and localized swelling around the injury3
- Pain at the bleeding site3
- Pulsatile bright red blood in arterial bleeding or steady dark red blood in venous bleeding3
Minor external bleeding, like scrapes or small cuts, often stops spontaneously or with simple first aid3 . However, persistent or heavy bleeding requires medical evaluation.
Internal Hemorrhage Symptoms
Internal bleeding occurs inside the body and may not be immediately apparent. Symptoms depend on the anatomical site and extent of blood loss3 . Common signs include:
- Blood in vomit, stool, or urine3
- Abdominal pain or swelling indicating intra-abdominal bleeding3
- Visual disturbances such as double vision (diplopia) or blurred vision in intracranial hemorrhage5
- Changes in skin color, including pallor or bruising3
- Paresthesia (tingling or numbness) in limbs3
Medullary hemorrhage, a type of brainstem bleed, often presents with vertigo, headache, diplopia, and limb weakness5 . Internal hemorrhage can rapidly progress to life-threatening conditions if untreated.
Hypovolemic Shock Symptoms
Hypovolemic shock results from rapid loss of a significant portion of circulating blood volume, leading to insufficient oxygen delivery to tissues and organs3 . Symptoms include:
- Dizziness, fatigue, and weakness3
- Increased heart rate (tachycardia) and low blood pressure (hypotension) 3
- Confusion, seizures, or loss of consciousness in severe cases3
- Shortness of breath (dyspnea) 3
- Cold, clammy skin and pallor3
Shock can develop when more than 20% of blood volume is lost, regardless of bleeding site, and requires urgent intervention3 .
Profuse hemorrhage can induce constitutional symptoms and may cause death within seconds if not promptly controlled. Recognizing early signs of shock is vital to prevent irreversible organ damage4 6.
Common Causes of Hemorrhage
Hemorrhage results from damage or disruption to blood vessels due to various causes:
- Trauma: Accidents, falls, penetrating injuries, and crushing wounds can cause vessel rupture and bleeding3 .
- Medical conditions: Diseases such as liver disease, cancer, diabetes, vitamin K deficiency, and hypertension increase bleeding risk3 .
- Bleeding disorders: Hereditary or acquired conditions like hemophilia and von Willebrand disease impair normal clotting and predispose to hemorrhage7 .
- Medications: Drugs that affect hemostasis, including anticoagulants (heparin, warfarin) and antiplatelet agents (aspirin), elevate bleeding risk7 .
- Vascular abnormalities: Aneurysms, arteriovenous malformations, and amyloid angiopathy can weaken vessel walls and cause spontaneous hemorrhage8 .
Risk Factors
Certain factors increase the likelihood of hemorrhage:
- Age and gender influence bleeding risk, with older adults and males often more affected9 3.
- Comorbidities such as diabetes, irritable bowel syndrome, and hypertension contribute to vessel fragility and bleeding tendency9 3.
- Obstetric factors, especially in postpartum hemorrhage, can lead to severe bleeding after childbirth10 .
- Family history of bleeding disorders raises individual risk7 .
- Use of blood-thinning medications or presence of chronic health conditions increases susceptibility7 .
Postpartum haemorrhage is the most dangerous childbirth complication since it can escalate with such alarming speed. While it is not always predictable, deaths are preventable with the right care10 .
How Hemorrhage Is Diagnosed
Diagnosis of hemorrhage relies on a thorough clinical assessment and targeted investigations:
- A detailed history and physical examination are essential to identify bleeding sites and assess severity11 3.
- Vital signs monitoring helps detect shock or ongoing blood loss3 .
- Laboratory tests evaluate anemia, coagulation status, platelet counts, and infection markers3 .
- Imaging studies such as computed tomography (CT) and magnetic resonance imaging (MRI) localize internal bleeding and assess organ involvement3 .
- Angiography uses contrast and X-rays to visualize blood vessels and pinpoint bleeding sources3 .
- Endoscopy allows direct visualization of the gastrointestinal tract to detect and manage internal bleeding3 .
Risk factors including age, comorbidities, and medication use are considered during diagnosis to tailor management9 7.
Hemorrhage Care and Treatment
Effective hemorrhage management involves immediate first aid and advanced in-hospital treatments depending on severity and location.
First Aid
Initial care focuses on controlling bleeding to prevent shock and complications:
- Apply direct pressure to the wound using a clean cloth or sterile bandage3 .
- Elevate the bleeding limb above heart level if possible to reduce blood flow3 .
- For minor external bleeding, wound cleansing with mild soap and water is recommended3 .
- Use a tourniquet as a last resort for severe extremity bleeding, applied 2-3 inches above the injury3 .
- If a tourniquet is unavailable, wound packing with gauze or a clean cloth can help control bleeding3 .
- Maintain pressure until professional medical help arrives3 .
Emergency medical services should be contacted immediately for major bleeding or signs of shock3 .
In-Hospital Treatments
Hospital care aims to stop bleeding, treat underlying causes, and support recovery:
- Surgical or angiographic interventions are primary methods to control life-threatening hemorrhage12 13.
- Blood transfusions and intravenous fluids restore circulating volume and oxygen delivery2 .
- Medications such as tranexamic acid (TXA) promote clot formation by inhibiting fibrin breakdown and reduce mortality when given early after injury2 4.
- Vitamin K injections may be used for coagulopathy related to deficiency or anticoagulant use3 .
- Advanced imaging guides targeted treatment and monitors response3 .
Comprehensive medical training and clear treatment protocols improve patient outcomes in hemorrhage management14 .
Women affected by PPH need care that is fast, feasible, effective and drives progress towards eliminating PPH-related deaths. These guidelines take a proactive approach of readiness, recognition and response10 .
Potential Hemorrhage Complications
Uncontrolled hemorrhage can lead to severe and sometimes fatal complications:
- Hypovolemic shock: Rapid blood loss causes inadequate tissue perfusion and oxygenation, leading to organ failure6 3.
- Coagulopathies: Bleeding disorders or massive transfusions can disrupt normal clotting mechanisms3 .
- Multiorgan failure: Prolonged shock damages vital organs including kidneys, liver, and brain3 .
- Sepsis: Infection risk increases with open wounds and invasive procedures3 .
- Death may occur within minutes in cases of profuse hemorrhage without timely intervention4 .
First aid combined with definitive medical care improves survival and reduces morbidity13 .
Hemorrhage Overview
Hemorrhage is the loss of blood from damaged blood vessels, which can be internal or external1 . It is a leading cause of death, especially in trauma patients aged 1 to 46 years2 . The severity of hemorrhage ranges from minor bruises to catastrophic bleeding in vital organs like the brain15 1. Rapid blood loss can cause hypovolemic shock, characterized by low blood pressure, hypoxia, and multi-organ dysfunction3 6.
Survival depends on the bleeding site, volume lost, and speed of treatment. For example, intracerebral hemorrhage has a 30-day mortality rate up to 40%, with most survivors experiencing severe disability15 . Losing more than 40% of total blood volume can be fatal4 . Early recognition, prompt first aid, and advanced medical care are essential to improve outcomes2 .
Frequently Asked Questions
What is hemorrhage?
Hemorrhage is bleeding from any injured blood vessel, which can be minor or severe depending on the cause and location3 .
What causes hemorrhage?
Common causes include trauma, underlying diseases, bleeding disorders, and medications that affect clotting3 7.
What are the signs of hemorrhage?
Symptoms include visible bleeding, pain, dizziness, weakness, pallor, and in severe cases, shock3 .
How is hemorrhage treated?
Treatment depends on bleeding severity and site, ranging from first aid with pressure application to surgical intervention and blood transfusions3 .
When should I seek medical help?
Immediate medical attention is needed for heavy bleeding, persistent bleeding, signs of shock, or suspected internal hemorrhage3 .