Ticks are tiny arachnids that often go unnoticed when they bite, making tick bites a common but hidden health risk1 . These bites can transmit serious diseases such as Lyme disease and Rocky Mountain spotted fever, which require prompt recognition and treatment to prevent complications1 . Understanding how to identify ticks, recognize bite symptoms, and respond appropriately is essential for reducing the risk of tick-borne illnesses1 .
Identifying Ticks
Ticks belong to the order Ixodida and include more than 800 species worldwide, varying widely in size and color2 . They are arachnids, closely related to spiders and mites, and have eight legs2 . Their color ranges from reddish-brown to dark brown, and they can be very small, especially during their larval and nymph stages, making them difficult to spot2 1.
Ticks are obligate blood-feeding parasites that attach to hosts for extended periods, feeding on blood to grow and reproduce3 . Unlike many insects, ticks do not fly or jump but crawl onto hosts from vegetation1 . Their small size and painless bite often cause people to remain unaware of their presence1 .
Common Tick Bite Locations
Ticks are commonly found in wooded, brushy, or grassy areas where they wait for a host to pass by1 . After attaching to clothing or skin, ticks often crawl to warm, moist areas of the body before biting1 . Preferred bite sites include:
- Scalp and hairline1
- Armpits1
- Groin area1
- Behind the knees1
- Around the waist and belly button1
Ticks can bite any part of the body but favor thin or moist skin where attachment is easier1 . People living in or visiting wooded or grassy regions have a higher risk of tick exposure, especially during spring and summer when tick activity peaks1 .
Tick Bite Signs and Symptoms
Tick Bites vs. Other Insect Bite Stings
Tick bites often go unnoticed because ticks inject saliva with anesthetic properties, making the bite painless1 4. Unlike other bug bites, ticks remain attached to the skin for hours or days while feeding1 . The bite site may initially appear as a small red area, bump, or hard spot, sometimes with a visible tick still attached4 .
Key differences between tick bites and other insect bites include:
- Presence of an attached tick at the bite site, which does not leave immediately4
- Bites often occur in concealed, warm areas rather than exposed skin1 4
- Tick bites may develop a characteristic rash, such as the bull’s-eye pattern seen in Lyme disease, which is uncommon in other insect bites1 4
- Reactions to tick bites may develop gradually over days, unlike immediate reactions typical of mosquito or flea bites4
Symptoms of Tick-Borne Diseases
While many tick bites do not cause illness, some transmit pathogens that lead to serious diseases1 . Symptoms of tick-borne illnesses usually develop within 3 to 30 days after the bite and can include:
- Rash (varies by disease) 1
- Fever and chills1
- Headache1
- Muscle and joint aches1
- Fatigue and weakness1
- Swollen lymph nodes5
Two common tick-borne diseases with distinct rash patterns are:
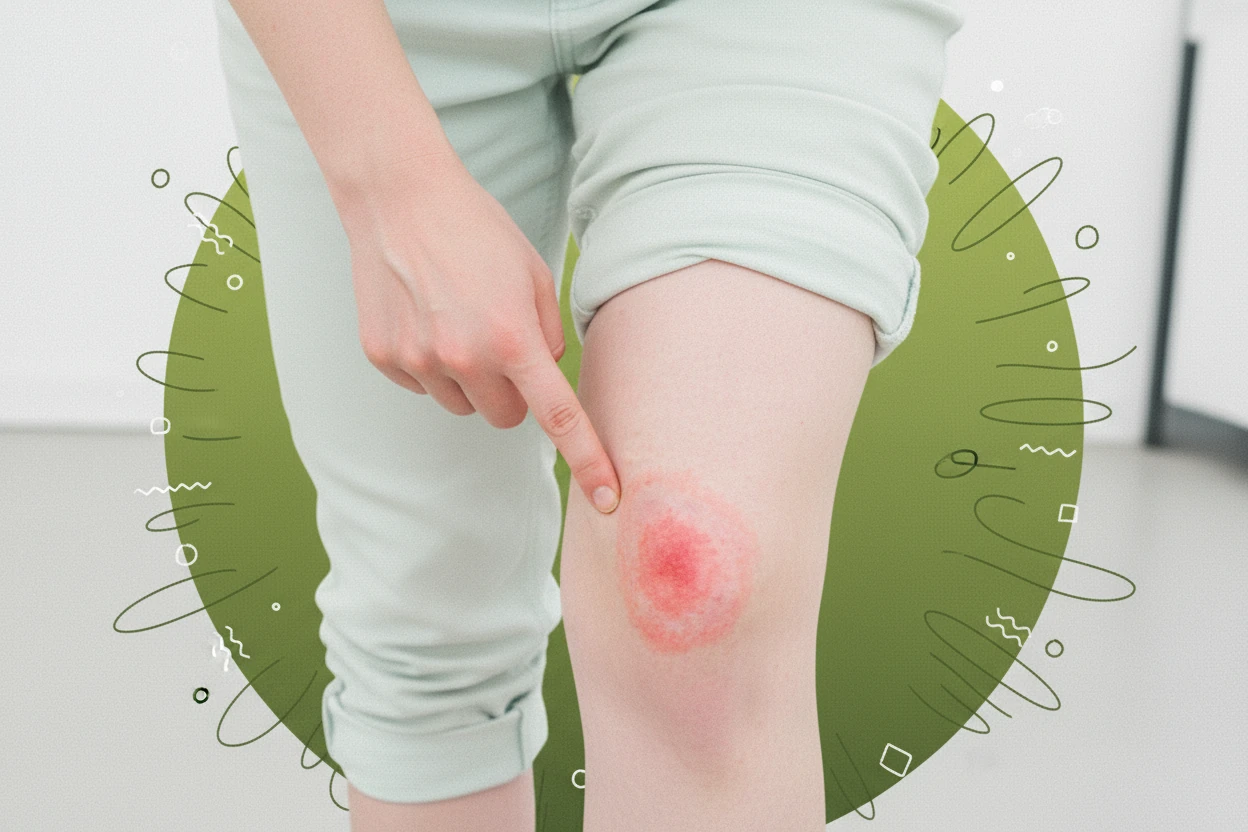
- Lyme Disease: The hallmark rash, erythema migrans, often appears as an expanding red ring with central clearing, resembling a bull’s-eye. It typically develops within 3 to 30 days after a tick bite but may vary in appearance and location6 75.
- Rocky Mountain Spotted Fever (RMSF): This disease causes a rash with small red or pink spots that usually begin 2 to 4 days after fever onset. The rash often starts on the wrists, forearms, ankles, and legs before spreading1 8. The rash is typically not itchy8 .
Other tick-borne illnesses include anaplasmosis, babesiosis, southern tick-associated rash illness (STARI), and tick paralysis, each with varying symptoms1 4.
“I’m seeing the impacts of tick-borne diseases, and I urge everyone to take preventative measures.”
— Stephanie Lareau, Virginia Tech Carilion School of Medicine9
Immediate Tick Bite Response
How To Remove a Tick
Proper tick removal is critical to reduce the risk of infection. The Centers for Disease Control and Prevention (CDC) recommends the following steps:
- Use fine-tipped tweezers or specialized tick removal tools to grasp the tick as close to the skin surface as possible1 .
- Pull upward with steady, even pressure without twisting or jerking to avoid breaking off the tick’s mouthparts1 .
- Avoid crushing the tick’s body or using methods like petroleum jelly, heat, or nail polish, which are ineffective and may increase infection risk1 4.
- After removal, clean the bite area thoroughly with soap and water, rubbing alcohol, or an iodine scrub1 4.
- Save the tick in a sealed container if possible, noting its appearance and the time it was attached, to assist healthcare providers if symptoms develop1 4.
Ticks that are firmly attached and do not brush off easily are likely feeding and should be removed promptly3 .
Treatment
Most tick bites heal without complications. However, if a tick-borne disease is suspected or symptoms develop, early treatment is essential1 . Antibiotics such as doxycycline are commonly used to treat Lyme disease and other bacterial tick-borne infections1 5. Some viral tick-borne diseases have no specific treatments and require supportive care1 .
Treatment effectiveness improves with early diagnosis, reducing the risk of serious complications such as cardiac, neurological, or renal involvement1 6. Untreated infections can lead to prolonged symptoms or severe illness1 .
When to Seek Medical Care
Contact a healthcare provider if:
- The tick was attached for more than 24 hours or appears engorged (rounded) 14.
- You develop symptoms such as rash, fever, headache, muscle aches, joint pain, or swollen lymph nodes within 30 days of a tick bite1 4.
- You notice a bull’s-eye or other expanding rash around the bite site1 6.
- You are unsure if the entire tick was removed or if the bite site is painful, blistered, or infected1 4.
Although ticks can be submitted to laboratories for pathogen testing, the CDC advises against routine tick testing due to variability in test quality and interpretation1 . A positive tick test does not confirm infection transmission, and a negative result does not rule out disease1 . Symptoms usually appear before test results are available, so clinical evaluation is paramount1 .
Removing a tick within 36 hours can reduce the risk of Lyme disease transmission.
— Stephanie Lareau, Virginia Tech Carilion School of Medicine9
Tick Bite Prevention
Preventing tick bites is the most effective way to avoid tick-borne diseases. Key prevention strategies include:
- Avoiding wooded, brushy, and grassy areas where ticks thrive, especially during peak activity in spring and summer1 9.
- Wearing light-colored clothing to spot ticks more easily, with long sleeves and pants tucked into socks1 9.
- Using EPA-approved insect repellents containing DEET, picaridin, or other effective ingredients on exposed skin1 9.
- Treating clothing, shoes, and gear with permethrin, an insecticide that kills ticks on contact1 9.
- Performing thorough tick checks on yourself, family members, and pets after outdoor activities, paying close attention to common bite sites1 9.
- Washing clothes in hot water and drying on high heat to kill ticks on clothing1 9.
- Keeping grass mowed and removing leaf litter and brush from yards to reduce tick habitats1 9.
Pets can carry ticks into the home, so regular inspection and veterinary tick control are important1 .
Key Takeaways
- Ticks are small arachnids that feed on blood and can transmit serious diseases such as Lyme disease and Rocky Mountain spotted fever2 1.
- Tick bites often go unnoticed due to their painless nature and small size, especially in larval and nymph stages1 .
- Common tick bite sites include the scalp, armpits, groin, behind knees, and waist1 .
- Early symptoms of tick-borne diseases include rash, fever, headache, muscle aches, and fatigue, typically appearing within 3 to 30 days after a bite1 6.
- Prompt and proper tick removal using fine-tipped tweezers reduces infection risk1 .
- Prevention through protective clothing, repellents, and tick checks is essential to reduce tick bite risk1 9.
- Seek medical care if symptoms develop or if the tick was attached for an extended period1 .
Frequently Asked Questions
Q: How can I tell if a tick is still attached after removal?
A: After removing a tick, inspect the bite site closely. If you see a small black dot, the tick’s head or mouthparts may remain embedded. Use sanitized tweezers to remove any remnants or seek medical advice if unsure4 .
Q: Can I get Lyme disease without seeing a tick bite?
A: Yes, many people do not notice tick bites because ticks are small and their bites painless. Symptoms or characteristic rashes often prompt diagnosis1 5.
Q: Should I have the tick tested for disease?
A: Routine tick testing is not recommended due to variability in test accuracy and interpretation. Clinical symptoms guide diagnosis and treatment more reliably1 .
Q: What should I do if I develop a rash after a tick bite?
A: Seek medical evaluation promptly. Early treatment of tick-borne diseases improves outcomes and prevents complications1 6.