Oropouche virus (OROV) is an emerging arbovirus that has caused over half a million infections primarily in tropical regions of the Americas. Recent cases in travelers to the United States highlight its potential for geographic expansion due to climate change and increased global travel1 2. This virus causes a febrile illness with symptoms similar to other tropical diseases, posing diagnostic challenges and raising public health concerns3 4.
Oropouche Virus Overview
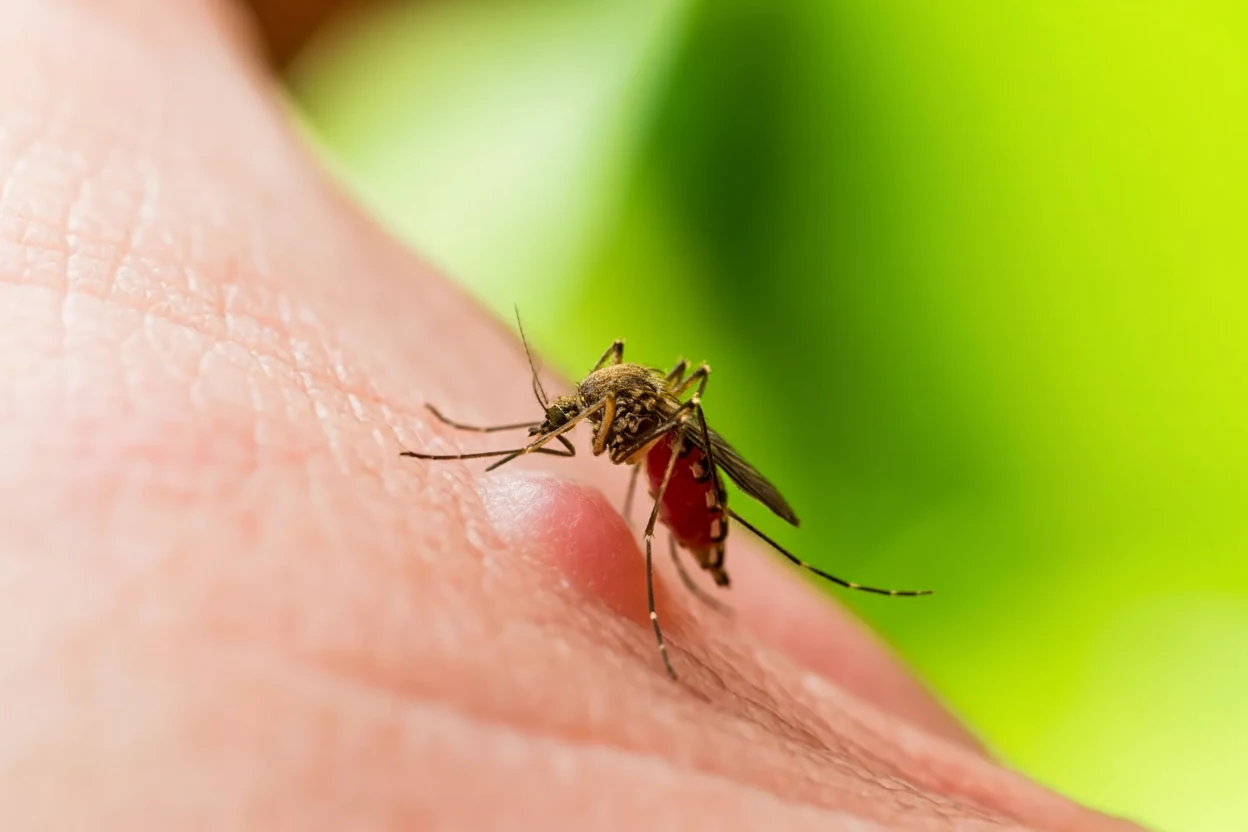
Oropouche virus belongs to the Orthobunyavirus genus within the Peribunyaviridae family and is primarily transmitted to humans through the bite of infected biting midges, especially Culicoides paraensis1 5. Some mosquito species may also act as vectors, although midges are the main transmitters1 3. The virus was first isolated in 1955 from a febrile patient in Trinidad and Tobago and later found in mosquitoes and sloths, which serve as natural reservoirs in sylvatic (wild) transmission cycles1 6.
The nickname "sloth fever" comes from the virus's isolation in a three-toed sloth in Brazil in 1960, highlighting the role of sloths as potential reservoirs alongside primates and birds1 67. Oropouche virus is endemic mainly in tropical South America, Central America, and the Caribbean, with outbreaks reported since its discovery. Although no local transmission has been documented in the United States, imported cases have been identified in travelers returning from endemic areas1 8.
Environmental factors such as climate change and increased human mobility contribute to the risk of Oropouche virus spreading beyond its traditional boundaries1 2. The virus's ability to cause urban outbreaks, facilitated by vector species thriving in human environments, underscores the need for surveillance and public health preparedness1 .
💡 Did You Know?
Oropouche virus is spread to people primarily by the bite of infected biting midges. Some mosquitoes can also spread the virus. The virus has been reported in parts of South America, Central America, and the Caribbean5 .
Symptoms of Oropouche Virus
Oropouche virus infection typically causes an acute febrile illness with an incubation period ranging from 3 to 10 days after exposure1 9. Approximately 60% of infected individuals develop symptoms, which usually last between 3 to 6 days but can sometimes persist or relapse days to weeks later1 3.
Common symptoms include:
- Sudden onset of high fever1 3
- Severe headache1 9
- Muscle aches (myalgia) and joint pains (arthralgia) 13
- Chills and fatigue1 4
- Eye pain and photophobia (sensitivity to light) 19
- Nausea, vomiting, and diarrhea1 9
- Maculopapular rash1 4
Neurological complications such as aseptic meningitis and encephalitis are rare but have been documented in a small percentage of cases (up to 4%) 193. Guillain-Barré syndrome (GBS), a serious neurological disorder, has also been reported following Oropouche virus infection in some patients9 .
Fatalities are uncommon but have been reported, particularly in Brazil, including two deaths in previously healthy adults in 20241 102. Pregnant individuals face increased risks, with documented cases of vertical transmission leading to fetal death, miscarriage, and congenital abnormalities such as microcephaly1 107. Older adults and immunocompromised persons are also at higher risk for severe disease1 .
Summary of key symptoms and risks:
- Incubation: 3–10 days1 9
- Symptomatic illness in ~60% of cases1 3
- Symptoms last 3–6 days, with possible relapses1 3
- Rare neurological complications: meningitis, encephalitis, GBS1 9
- Rare fatalities reported, mostly in Brazil1 2
- Pregnancy risks: fetal death, miscarriage, microcephaly1 10
- Higher severity risk in older and immunocompromised individuals1
Oropouche virus disease symptoms overlap with other tropical infections like dengue and chikungunya, making laboratory diagnosis essential. Neurological complications, though rare, can be severe, and pregnant women face particular risks including fetal harm10 9.
Oropouche Virus Treatment
There are currently no FDA-approved antiviral drugs or vaccines for Oropouche virus infection, so treatment is primarily supportive and aimed at relieving symptoms1 1110. Most infections are self-limiting and resolve without complications within about a week, although recovery can take longer in some cases1 2.
Supportive care includes:
- Rest to aid recovery1 9
- Hydration to prevent dehydration from fever, vomiting, or diarrhea1 7
- Use of over-the-counter analgesics and antipyretics such as acetaminophen to reduce fever and pain1 79
Patients are advised to avoid aspirin and non-steroidal anti-inflammatory drugs (NSAIDs) due to the risk of bleeding complications7 9. In rare cases with severe neurological involvement or complications, hospitalization and specialized medical care may be necessary1 9.
Relapses of symptoms can occur days to weeks after initial recovery, requiring ongoing monitoring1 3. Pregnant patients and those with weakened immune systems should be closely observed due to the increased risk of severe outcomes1 .
Climate change and increased global travel contribute to the emergence of vector-borne diseases like Oropouche virus in new regions. Vigilance and vector control are key to preventing outbreaks beyond endemic areas1 2.
Oropouche virus disease is caused by the Oropouche virus (OROV) and can cause fever, headache, joint pain, muscle pain, chills, nausea, vomiting, and rash. Most people recover on their own, but the disease can cause severe symptoms in some patients1 .
Preventing Oropouche Virus
Prevention of Oropouche virus infection relies on avoiding bites from infected biting midges and mosquitoes, as no vaccine or specific prophylactic treatment currently exists1 1110. Personal protective measures and vector control are the main strategies to reduce infection risk.
💡 Did You Know?
The best way to protect yourself and your family from Oropouche virus is to prevent bites from biting midges and mosquitoes by using repellents, protective clothing, and avoiding peak vector activity times5 .
Key prevention measures include:
- Using insect repellents effective against midges and mosquitoes1 10
- Wearing long-sleeved shirts and long pants to minimize exposed skin1 10
- Sleeping under insecticide-treated bed nets or using fine mesh screens on windows and doors1 10
- Avoiding outdoor activities during peak vector activity times, typically dawn and dusk1 10
- Eliminating or avoiding vector breeding sites such as standing water1 10
Travel advisories recommend that pregnant individuals avoid travel to endemic areas due to the risk of fetal complications1 10. Clinicians should consider recent travel history in patients presenting with compatible symptoms to facilitate timely diagnosis and management1 12.
Surveillance and public health monitoring remain important to detect any potential local transmission in the United States, although current risk is low1 122.