Metabolic dysfunction-associated steatohepatitis (MASH) is a progressive liver disease that often develops silently and can lead to serious complications such as cirrhosis and liver cancer1 . Many patients with MASH are asymptomatic in early stages, making diagnosis challenging and often reliant on routine blood tests and imaging studies2 . Early identification and management of MASH are crucial to prevent liver damage and associated metabolic and cardiovascular risks3 .
Initial Evaluation and Medical History
The initial evaluation for suspected MASH begins with a thorough medical history and physical examination focused on identifying metabolic risk factors and excluding other liver diseases3 . Key components include assessing alcohol consumption, medication use, and lifestyle factors to rule out alternative causes of liver injury3 . Because early MASH is often asymptomatic, clinicians should maintain a high index of suspicion in patients with metabolic syndrome features2 .
Symptoms, when present, are usually nonspecific and may include fatigue, abdominal discomfort, or general weakness2 . Physical signs of advanced liver disease in MASH patients include jaundice, abdominal swelling (ascites), peripheral edema, and neurological symptoms such as confusion due to hepatic encephalopathy2 . Screening for metabolic risk factors such as hypertension, obesity, type 2 diabetes, and dyslipidemia is essential during the initial assessment3 .
- Evaluate alcohol intake and exclude alcoholic liver disease3 .
- Review medication history for drugs associated with liver injury3 .
- Assess lifestyle factors including diet and physical activity3 .
- Screen for metabolic syndrome components: hypertension, obesity, diabetes, dyslipidemia3 .
- Identify symptoms and signs suggestive of advanced liver disease2 .
Early MASH is frequently asymptomatic, requiring laboratory and imaging studies for detection. Exclusion of other liver diseases is essential in the diagnostic workup of MASH2 3.
Diagnostic Blood Tests
Blood tests play a pivotal role in detecting liver injury and assessing metabolic status in patients suspected of having MASH2 . Common laboratory evaluations include liver enzymes such as alanine aminotransferase (ALT) and aspartate aminotransferase (AST), which are frequently elevated in MASH due to hepatocellular injury2 . Additionally, fibrosis markers and lipid profiles help assess liver fibrosis severity and metabolic dysfunction3 .
Dyslipidemia, characterized by elevated cholesterol and triglycerides, is commonly associated with MASH and should be evaluated4 . Non-invasive fibrosis panels, such as FibroTest, can estimate the degree of liver fibrosis and guide further diagnostic steps5 . Routine blood tests also include complete blood count (CBC) and comprehensive metabolic panel (CMP) to evaluate overall health and exclude other causes of liver disease6 .
- Measure liver enzymes ALT and AST to detect hepatocellular injury2 .
- Assess fibrosis markers using panels like FibroTest for fibrosis staging5 .
- Evaluate lipid profile for dyslipidemia, including cholesterol and triglycerides4 .
- Perform CBC and CMP to assess general health and exclude other conditions6 .
- Use non-invasive fibrosis scores such as FIB-4 to stratify fibrosis risk7 .
"Diagnosis of MASLD can be challenging because most patients are asymptomatic and are only identified by routine blood tests that show elevated liver enzymes." 8
Liver Imaging Procedures
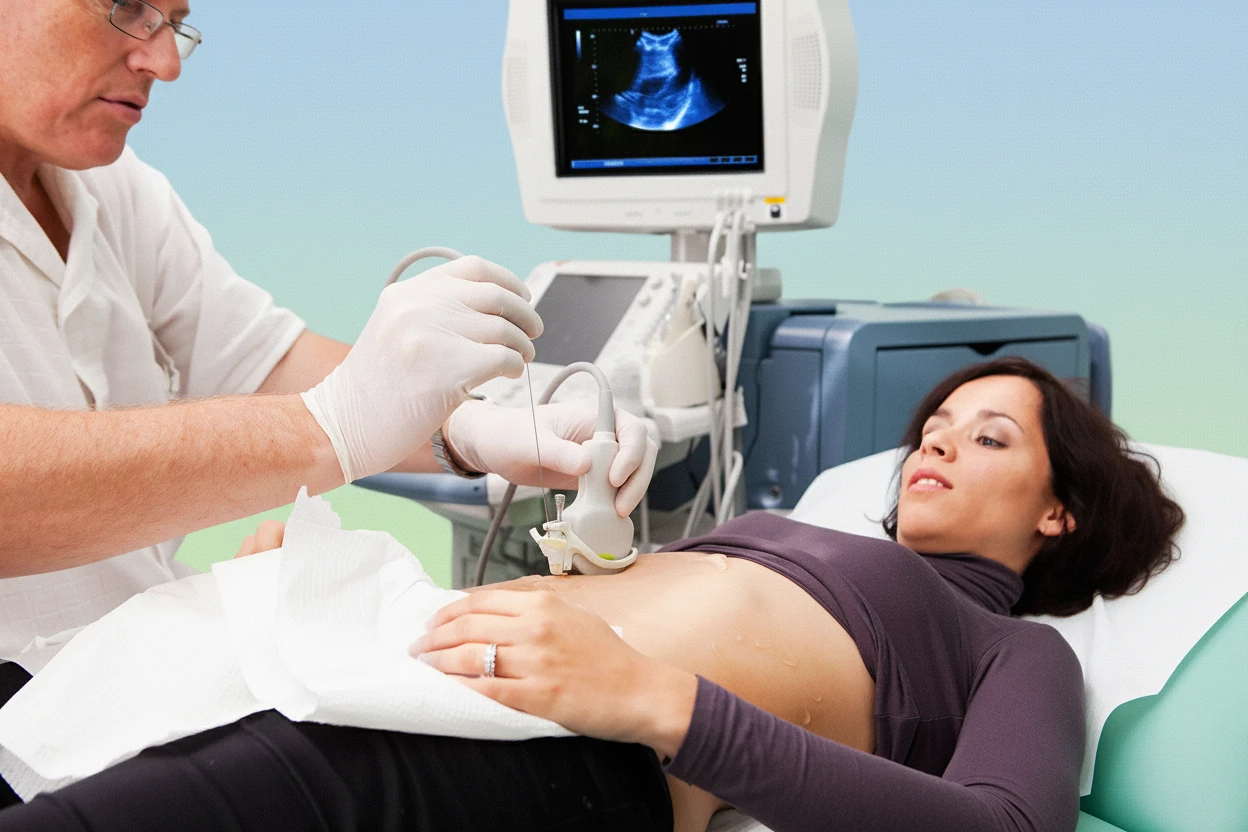
Imaging studies are essential to detect hepatic steatosis (fat accumulation) and assess liver fibrosis non-invasively in MASH patients2 . Ultrasound is the first-line imaging modality used to identify fatty infiltration and changes in liver texture3 . Computed tomography (CT) scans provide detailed cross-sectional images useful for evaluating liver morphology and fat content2 .
Advanced imaging techniques include acoustic radiation force impulse (ARFI) elastography and FibroScan, which measure liver stiffness as a surrogate for fibrosis severity5 . Magnetic resonance elastography (MRE) offers the most accurate non-invasive quantification of liver fibrosis and inflammation, enhancing diagnostic precision5 . These imaging tools help reduce the need for invasive liver biopsy in many cases.
- Use ultrasound to detect hepatic steatosis and liver texture changes3 .
- Employ CT scans for detailed liver morphology and fat content assessment2 .
- Apply ARFI elastography to measure liver stiffness and fibrosis5 .
- Utilize FibroScan (transient elastography) for non-invasive fibrosis and steatosis evaluation5 .
- Consider MRE for precise quantification of fibrosis and inflammation5 .
Imaging modalities are essential for detecting liver fat accumulation and fibrosis in MASH, with magnetic resonance elastography (MRE) providing the most accurate non-invasive quantification2 5.
Liver Biopsy Procedure
Liver biopsy remains the gold standard for definitive diagnosis and staging of MASH, especially when non-invasive tests yield inconclusive results5 . The procedure involves obtaining a small tissue sample from the liver, typically via percutaneous needle insertion, for microscopic examination5 . Laparoscopic liver biopsy is an alternative method using a camera-guided instrument to collect tissue5 .
Histological analysis of biopsy specimens allows pathologists to assess the severity of inflammation, fibrosis, and steatosis, which are critical for accurate staging and prognosis1 . The Kleiner scoring system is commonly used to grade fibrosis and steatohepatitis severity in MASH1 . Despite its invasiveness, biopsy provides essential information that guides treatment decisions.
- Perform percutaneous liver biopsy to obtain tissue for histological analysis5 .
- Consider laparoscopic biopsy as an alternative method for tissue sampling5 .
- Use histological scoring systems like Kleiner’s score to stage fibrosis and inflammation1 .
- Assess inflammation, fibrosis, and steatosis severity microscopically1 .
- Reserve biopsy for cases where non-invasive tests are inconclusive or for staging before treatment5 .
"Liver biopsy remains the definitive method for diagnosing and staging MASH, allowing detailed assessment of fibrosis and inflammation."
— Ko et al. 1
MASH Disease Stages
MASH progression is classified into stages based on the extent of liver fibrosis observed histologically1 . Accurate staging is crucial for prognosis and guiding therapy. The fibrosis stages are:
- Stage 1: Minimal perisinusoidal or portal fibrosis1 .
- Stage 2: Portal and periportal fibrosis without bridging1 .
- Stage 3: Bridging fibrosis connecting portal areas1 .
- Stage 4: Cirrhosis characterized by architectural distortion and regenerative nodules1 .
Disease severity increases with fibrosis stage, with advanced stages associated with higher risks of liver failure, hepatocellular carcinoma, and mortality1 . Non-invasive tests can estimate fibrosis stage but cannot replace biopsy for detailed microscopic features such as ballooning and lobular inflammation5 .
| Fibrosis Stage | Description | Clinical Implication |
|---|---|---|
| Stage 1 | Minimal perisinusoidal or portal fibrosis | Early disease, often asymptomatic1 |
| Stage 2 | Portal and periportal fibrosis without bridging | Moderate fibrosis, risk of progression1 |
| Stage 3 | Bridging fibrosis connecting portal areas | Advanced fibrosis, increased complications1 |
| Stage 4 | Cirrhosis with architectural distortion | High risk of liver failure and cancer1 |
| Sources: 1 | ||
Screening for Related Health Issues
Screening for comorbid conditions is integral to the diagnosis and management of MASH due to its strong association with metabolic and cardiovascular diseases3 . Patients with MASH often have hypertension, type 2 diabetes, dyslipidemia, and obesity, which contribute to disease progression and overall morbidity3 9.
Excluding other liver diseases such as alcoholic liver disease, viral hepatitis, and drug-induced liver injury is essential to avoid misdiagnosis3 . Screening for cardiovascular disease and diabetes is recommended because these conditions frequently coexist with MASH and influence patient outcomes9 . Regular monitoring for complications like hepatocellular carcinoma is advised in advanced fibrosis stages1 .
- Screen for hypertension, diabetes, and dyslipidemia in all patients with MASH3 .
- Exclude alcoholic liver disease through detailed history and laboratory tests3 .
- Test for viral hepatitis to rule out alternative liver injury causes3 .
- Assess for drug-induced liver injury based on medication history3 .
- Monitor for cardiovascular disease due to increased risk in MASH patients9 .
MASH is considered the hepatic manifestation of metabolic syndrome, linking it closely to cardiovascular and metabolic comorbidities10 .
Diagnosis Summary
Diagnosing MASH involves a multi-step approach combining clinical evaluation, laboratory testing, imaging, and sometimes liver biopsy5 . Early diagnosis is challenging because many patients are asymptomatic and identified incidentally through elevated liver enzymes or imaging findings8 . Exclusion of other liver diseases is critical to confirm MASH diagnosis3 .
"Despite high disease burden, MASH is underdiagnosed; prompt diagnosis and management are crucial for improving outcomes."
— Eskridge et al. 2
Non-invasive tests such as fibrosis scores (e.g., FIB-4), elastography (FibroScan, ARFI), and advanced imaging (MRE) are increasingly used to assess fibrosis and steatosis severity, reducing the need for biopsy in many cases5 7. However, liver biopsy remains the definitive method for staging and confirming diagnosis when non-invasive tests are inconclusive or when precise histological information is needed1 .
Screening for metabolic risk factors and related comorbidities is essential to guide comprehensive management and improve patient outcomes3 9. Early intervention with lifestyle changes and pharmacotherapy can slow disease progression and reduce complications11 .
- Begin with detailed history and physical exam to evaluate metabolic risk and exclude other causes3 .
- Use blood tests to detect liver enzyme abnormalities and assess fibrosis risk2 .
- Employ imaging techniques to identify steatosis and estimate fibrosis5 .
- Reserve liver biopsy for definitive diagnosis and staging when necessary1 .
- Screen and manage associated metabolic and cardiovascular conditions3 9.