Each year in the United States, healthcare providers perform intubation millions of times, primarily in operating rooms and emergency settings1 . Intubation is a lifesaving procedure that helps patients breathe when they cannot do so on their own by placing a tube into the airway2 . This procedure is essential in emergencies, surgeries, and critical care to maintain oxygen delivery and protect the lungs1 .
The Intubation Procedure
Intubation involves inserting a flexible tube called an endotracheal tube into the trachea (windpipe) to secure the airway and allow for oxygen delivery or mechanical ventilation3 . There are two main routes for intubation: through the mouth (orotracheal) and through the nose (nasotracheal). The choice depends on the clinical situation, patient anatomy, and surgical needs4 .
Through the Mouth
Orotracheal intubation is the most common method, especially in emergencies and surgeries, because it is faster and generally less uncomfortable than nasal intubation3 5. The procedure typically involves the following steps:
- The patient is positioned lying flat on their back, and sedation or anesthesia is administered to reduce discomfort and suppress airway reflexes6 1.
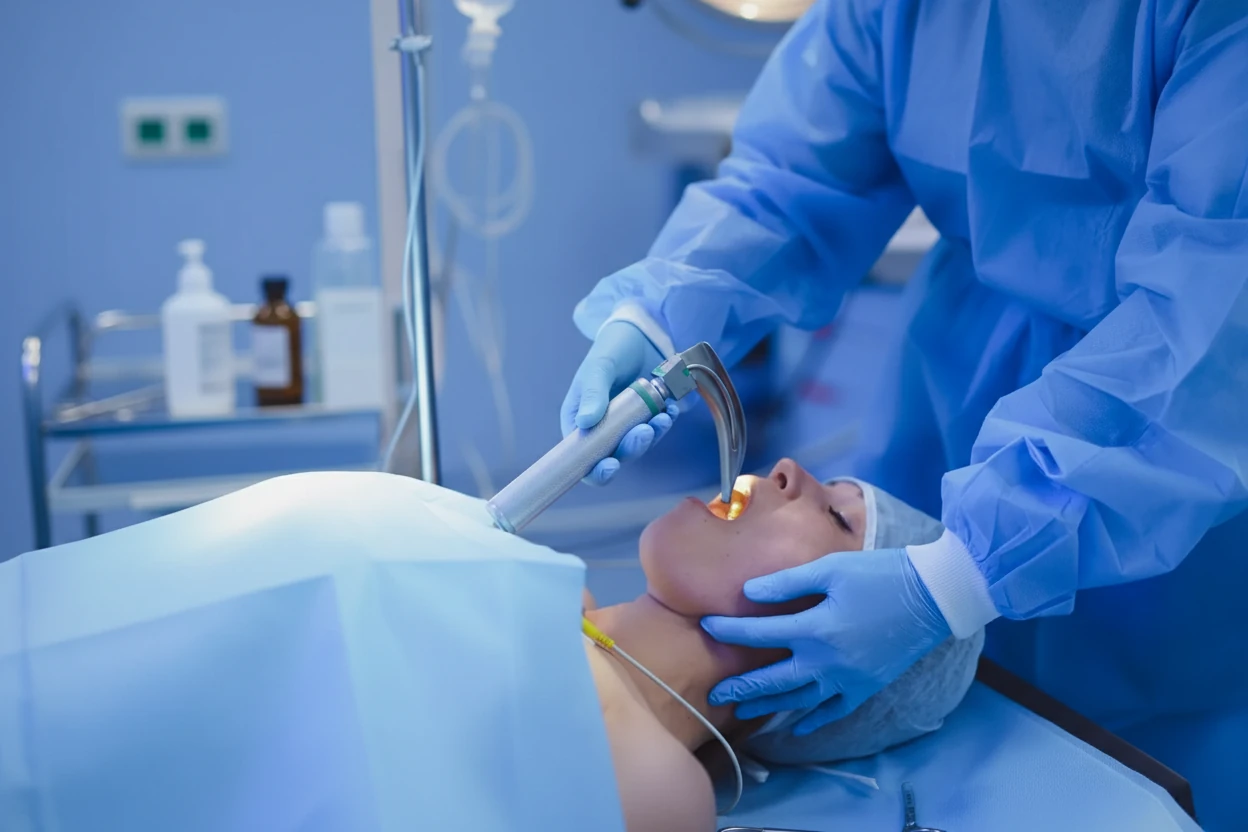
- A healthcare provider uses a laryngoscope, a device with a light and sometimes a camera (video laryngoscope), to visualize the vocal cords and upper airway7 3.
- The endotracheal tube is carefully guided through the mouth, past the vocal cords, and into the trachea3 1.
- A small balloon (cuff) at the end of the tube is inflated to secure the tube in place and prevent stomach contents from entering the lungs (aspiration) 1.
- The tube is secured outside the mouth with tape or straps to prevent movement2 .
- Proper tube placement is confirmed by clinical signs, listening to breath sounds, capnography (measuring exhaled carbon dioxide), and imaging such as chest X-ray3 2.
Orotracheal intubation usually takes less than a minute in emergencies and is often performed by trained medical teams in hospitals or prehospital settings2 .
Through the Nose
Nasotracheal intubation involves inserting the tube through the nostril and is used primarily in specific surgical cases involving the head, mouth, or neck, or when oral intubation is contraindicated8 54. The procedure includes:
- Sedation or topical anesthesia to ease discomfort, especially if the patient is awake9 8.
- The tube is gently passed through the nasal passage into the throat.
- A laryngoscope or fiberoptic scope guides the tube between the vocal cords into the trachea8 1.
- The cuff is inflated and the tube secured externally, similar to oral intubation8 .
- Confirmation of tube placement is done with clinical assessment and imaging3 .
Nasotracheal intubation is generally slower and may cause nasal bleeding (epistaxis), which is the most common complication of this route5 . It is preferred when oral access is limited or to avoid additional trauma to the neck10 .
Intubation can help save your life when you can't breathe. A healthcare provider uses a laryngoscope to guide an endotracheal tube into your mouth or nose, voice box, and then trachea. The tube keeps your airway open so you can get air into your lungs2 .
Reasons for Intubation
Intubation is primarily performed to secure the airway and ensure adequate oxygenation and ventilation in critically ill or injured patients11 . Common reasons include:
- Respiratory failure from trauma, pneumonia, emphysema, or other lung diseases11 3.
- Cardiac failure leading to inadequate breathing11 .
- Neurological impairment causing loss of airway reflexes and risk of aspiration6 .
- Need for general anesthesia during surgery when spontaneous breathing is suppressed3 1.
- Airway obstruction or blockage that prevents normal breathing12 .
- Protection of the lungs from aspiration of stomach contents, blood, or foreign material6 13.
- Facilitation of diagnostic or therapeutic airway procedures14 .
Mechanical ventilation is often delivered through the endotracheal tube to support or replace spontaneous breathing in these conditions3 .
Endotracheal intubation is an essential skill performed by multiple medical specialists to secure a patient's airway as well as provide oxygenation and ventilation.
— Andrea C. Alvarado, Jackson Memorial Hospital, University of Miami15
Contraindications for Intubation
While intubation is lifesaving, it is not always appropriate. Contraindications or situations requiring caution include:
- Severe maxillofacial trauma with distorted anatomy or heavy bleeding, which may obstruct oropharyngeal intubation16 17.
- Cervical spine injuries where neck manipulation during intubation could worsen damage18 19.
- Blocked pharynx or airway obstruction that prevents safe tube placement17 .
- Conditions where less invasive respiratory support may be effective, such as non-invasive ventilation11 12.
In these cases, alternative airway management strategies or delayed intubation may be considered to minimize harm17 .
What to Expect During Intubation
Intubation is often performed emergently, requiring rapid decision-making and patient assessment11 . The process generally involves:
- Administration of sedatives and paralytic agents to facilitate tube insertion and reduce discomfort or reflexes6 20.
- Positioning the patient to optimize airway visualization, usually lying flat with the head tilted back1 .
- Use of a laryngoscope or video laryngoscope to visualize the vocal cords7 .
- Insertion of the endotracheal tube through the mouth or nose into the trachea3 .
- Inflation of the cuff to secure the tube and prevent aspiration1 .
- Confirmation of correct placement by clinical signs, capnography, and imaging3 .
Patients who are awake may receive topical anesthesia and sedation to ease discomfort and improve cooperation during awake intubation9 . Special precautions are taken in trauma patients to avoid neck movement and further injury18 .
Endotracheal intubation is an essential resuscitative procedure in the emergency setting. Direct and video laryngoscopy are the two most common approaches utilized for endotracheal intubation.
— Patricia Panakos, Jackson Health System15
Potential Risks of Intubation
Despite being a common and generally safe procedure, intubation carries potential risks, especially in emergency settings where preparation is limited12 . Risks include:
- Hypoxemia (low blood oxygen) due to unsuccessful or delayed intubation21 .
- Cardiovascular instability such as hypotension and bradycardia caused by sedatives, paralytics, or vagal stimulation during laryngoscopy20 .
- Trauma to the airway, including punctures, bleeding, or damage to the vocal cords, larynx, or trachea5 13.
- Dental injury during laryngoscope insertion5 .
- Aspiration of stomach contents or foreign material into the lungs during the procedure13 22.
- Nasal bleeding (epistaxis) with nasotracheal intubation5 .
- Infection risk, including pneumonia or sinus infections13 23.
- Post-extubation discomfort such as sore throat, hoarseness, and difficulty swallowing or speaking24 1.
After extubation, patients require close monitoring of respiratory function and oxygen levels, with supplemental oxygen or mechanical ventilation continued as needed25 3. Medications to manage anxiety and discomfort are often part of post-intubation care26 .
| Potential Risks of Intubation | Description |
|---|---|
| Hypoxemia | Low oxygen levels during or after intubation21 |
| Cardiovascular instability | Hypotension, bradycardia from medications or vagal stimulation20 |
| Airway trauma | Injury to vocal cords, larynx, trachea, or teeth5 |
| Aspiration | Inhalation of stomach contents or fluids13 |
| Infection | Pneumonia or sinus infections post-procedure13 |
| Sources: 2120513 | |
Intubation vs. Ventilator Use
Intubation and mechanical ventilation are related but distinct interventions. Intubation secures the airway by placing a tube into the trachea, while mechanical ventilation uses a machine to assist or replace spontaneous breathing3 . Key points include:
- Intubation is necessary to maintain airway patency and allow mechanical ventilation3 .
- Mechanical ventilation can be delivered non-invasively (e.g., mask) or invasively via an endotracheal tube3 .
- Patients on ventilators are gradually weaned off support as their respiratory function improves25 .
- Being intubated does not always mean a patient is on a ventilator; some may be intubated for airway protection without mechanical ventilation1 .
Intubation is the process of placing a tube that protects the airway, keeping an open passageway to the lungs. Ventilation is the process by which air is mechanically moved in and out of the lungs when someone is unable to do that by themselves1 .
Summary and Key Takeaways
- Intubation is a critical medical procedure used to secure the airway and support breathing in emergencies, surgery, and critical illness11 3.
- Orotracheal intubation through the mouth is the most common and fastest method, while nasotracheal intubation through the nose is used in specific surgical or trauma cases3 54.
- Indications include respiratory failure, airway obstruction, anesthesia, and protection against aspiration6 12.
- Contraindications include severe facial trauma, cervical spine injury, and situations where less invasive ventilation may suffice18 1617.
- Risks include hypoxemia, cardiovascular instability, airway trauma, aspiration, and infection, but benefits generally outweigh these risks20 135.
- Intubation and mechanical ventilation are related but distinct; intubation secures the airway, while ventilation supports breathing3 25.