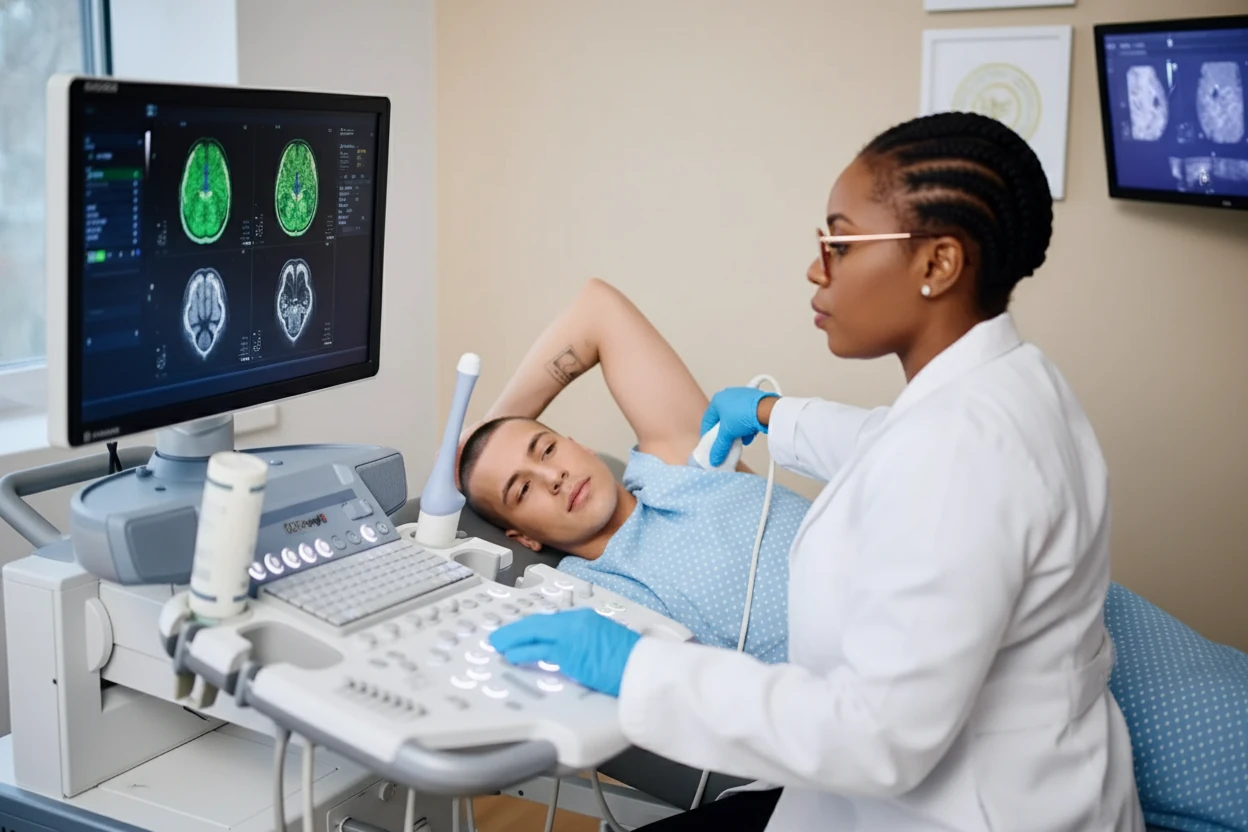
Breast cancer remains a leading cause of cancer-related deaths among women, with early detection playing a critical role in improving survival and quality of life1 . While screening mammograms are widely accessible at no cost under most insurance plans, follow-up diagnostic imaging after abnormal results often incurs significant out-of-pocket expenses for patients2 . These costs can deter women from completing necessary follow-up tests, leading to delayed diagnoses and potentially more advanced disease1 .
Cost Barriers to Breast Cancer Imaging
Despite the Affordable Care Act (ACA) mandating coverage of annual screening mammograms without cost-sharing for most private insurance plans, follow-up imaging after an abnormal mammogram is typically classified as diagnostic and may require patient cost-sharing2 . This distinction means that while initial screening is free, additional tests such as diagnostic mammograms, ultrasounds, MRIs, or biopsies often result in substantial out-of-pocket costs for patients2 .
Women enrolled in insurance plans with higher out-of-pocket costs undergo significantly fewer subsequent diagnostic breast procedures compared to those with lower out-of-pocket costs3 . High-deductible health plans, in particular, are associated with the greatest financial burden, with out-of-pocket costs accounting for nearly half of the total cost of follow-up diagnostic testing4 . Geographic disparities also exist, with patients in certain states facing higher out-of-pocket expenses than others1 .
Non-financial barriers such as childcare, travel, and logistical challenges further compound the difficulty of accessing follow-up imaging2 . These financial and practical obstacles contribute to delays or avoidance of recommended diagnostic testing, undermining the benefits of early breast cancer detection.
- Screening mammography is covered without cost-sharing under the ACA for most private insurance plans2 .
- Follow-up imaging after abnormal mammograms often requires patient cost-sharing, including deductibles and copayments2 .
- Patients with higher out-of-pocket costs undergo fewer follow-up breast diagnostic procedures3 .
- High-deductible plans impose the highest out-of-pocket expenses for follow-up imaging4 .
- Non-financial barriers such as childcare and travel also hinder access to follow-up imaging2 .
“Out-of-pocket cost sharing is a significant barrier for individuals needing access to multiple early detection services to find cancer at an earlier stage when treatment is more effective. These additional expenses can lead to delayed or skipped medically necessary procedures, resulting in potentially life-threatening consequences. Removing cost sharing for each intervention in the screening process is a critical step toward ending cancer for everyone.”
— Lisa Lacasse, American Cancer Society Cancer Action Network1
Follow-Up Imaging for Early Detection
Follow-up imaging after an abnormal mammogram is essential because approximately 20% of abnormal mammograms are associated with breast cancer3 . Timely diagnostic testing, including diagnostic mammograms, ultrasounds, MRIs, and biopsies, allows for confirmation or exclusion of cancer and guides appropriate treatment2 .
Early detection through follow-up imaging is strongly linked to improved survival rates and better quality of life for patients2 . Delays in follow-up testing can result in diagnosis at a later stage, which is associated with more aggressive treatment, higher healthcare costs, and poorer outcomes2 . Studies show that patients without out-of-pocket costs for follow-up testing are significantly more likely to receive timely diagnostic procedures, with a 17.1% higher likelihood of follow-up within 14 days of an abnormal mammogram4 .
Moreover, out-of-pocket costs not only delay follow-up testing but also reduce the likelihood of patients returning for future screening mammograms. It is estimated that nearly 378,000 women may skip future mammograms due to fear of subsequent out-of-pocket costs for follow-up tests1 . This avoidance further increases the risk of late-stage breast cancer diagnoses.
- About 20% of abnormal mammograms lead to a breast cancer diagnosis3 .
- Timely follow-up imaging improves survival and quality of life2 .
- Patients without out-of-pocket costs are more likely to complete follow-up testing promptly4 .
- Delayed follow-up can lead to later-stage cancer diagnosis and higher treatment costs2 .
- Out-of-pocket costs contribute to decreased adherence to future screening mammograms1 .
High out-of-pocket costs for follow-up breast imaging significantly deter completion of recommended diagnostic tests. This financial barrier causes delays in diagnosis and treatment, increasing the risk of later-stage breast cancer and higher healthcare costs. Addressing these costs through policy changes and patient support is essential to improve outcomes. 14
Reducing Breast Imaging Costs
Reducing the financial burden of follow-up breast imaging is critical to improving adherence to diagnostic testing and early cancer detection. Several strategies can help patients manage or lower their out-of-pocket costs:
“Patients more likely to skip diagnostic imaging tend to be racial/ethnic minorities, have lower educational levels, lower-income households, are on Medicaid, or have no insurance. Prior research shows these groups have lower adherence to preventive services, including breast cancer screening, and worse breast cancer outcomes. Out-of-pocket payments may contribute to delays in seeking care, leading to delays in diagnosis and treatment, increased breast cancer mortality, and exacerbation of existing care gaps in women facing financial barriers.”
— Michael Ngo, MD, Boston Medical Center and Boston University Chobanian & Avedisian School of Medicine6
- Insurance Plan Selection: Patients should consider the cost-sharing mechanisms of insurance plans, as high-deductible plans are associated with higher out-of-pocket expenses for follow-up imaging4 .
- Financial Assistance Programs: Patients can inquire about free or low-cost imaging programs and healthcare services available locally6 .
- Negotiating Medical Bills: Contacting the billing department to negotiate costs or arrange interest-free payment plans can make follow-up testing more affordable6 .
- Policy Advocacy: Supporting legislation that eliminates out-of-pocket costs for follow-up diagnostic testing can reduce financial barriers at a systemic level1 .
- Addressing Non-Financial Barriers: Assistance with childcare, transportation, and scheduling can improve access to follow-up imaging2 .
Eliminating out-of-pocket cost sharing for follow-up tests could prevent over 7,500 later-stage breast cancer diagnoses annually and save the U.S. healthcare system an estimated $2.2 billion in lifetime treatment costs1 . Patients without cost-sharing are more likely to receive timely follow-up testing and maintain regular screening schedules, which ultimately leads to earlier detection and better outcomes4 .
| Follow-Up Test Type | Out-of-Pocket Cost Increase (2018–2023) | Notes |
|---|---|---|
| Biopsy | 96% increase ($228 to $447) | Highest increase among follow-up tests4 |
| Diagnostic Mammogram | 73% increase | Significant cost barrier4 |
| Ultrasound | 59% increase | Common follow-up imaging4 |
| MRI | 45% increase | Often recommended for detailed imaging4 |